There are four types of basic tissues:
- Connective → Provides support
- Muscle → Movement
- Nervous → Provides control and communication
- Epithelial → To cover and protect the body
Epithelial tissue is present in two forms:
- As contiguous cells…
- that cover the body on the external surface (epithelial membrane)
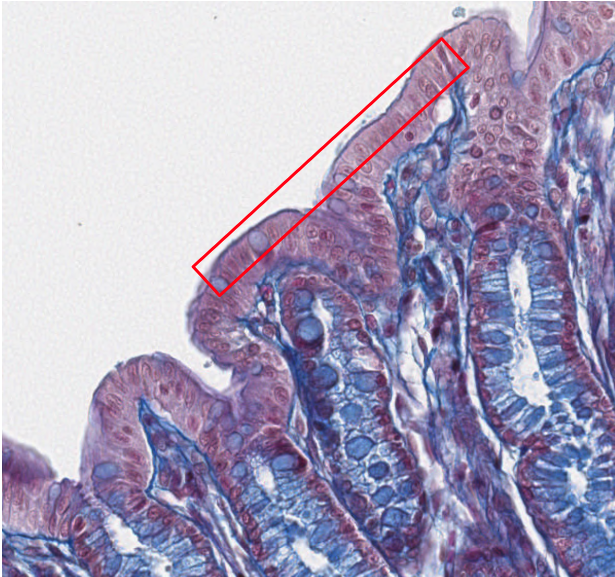
- or mucosa membranes that cover cavities connected to the outside (ex. digestive system)
- or serous membranes that line the body on its internal surface, as invagination of the epithelial tissue (ex. pelvic cavity).
- Glands which originate from invaginated epithelial cells.
Embryonic germ layers’ derivation of epithelial tissues
Ectoderm gives rise:
- Skin
- Oral mucosa
- Glands of the skin
- Mammary glands
Mesoderm:
- Serous membranes lining the body cavities
- Kidney
Endoderm:
- Liver
- Pancreas
- Respiratory and gastrontestinal tract
Functions of Epithelial Tissues
- Protection
- Secretion
- Absorption
- Selective permeability
- Detection of sensations: sensory epithelia
Epithelial Cell Polarity
An important aspect of an epithelium is its polarity.
Polarity is essential to carry out specific functions of the various organ systems.
Polarity is determined by the distribution of plasma membrane proteins and lipids and the rearrangement of the cytoskeleton.
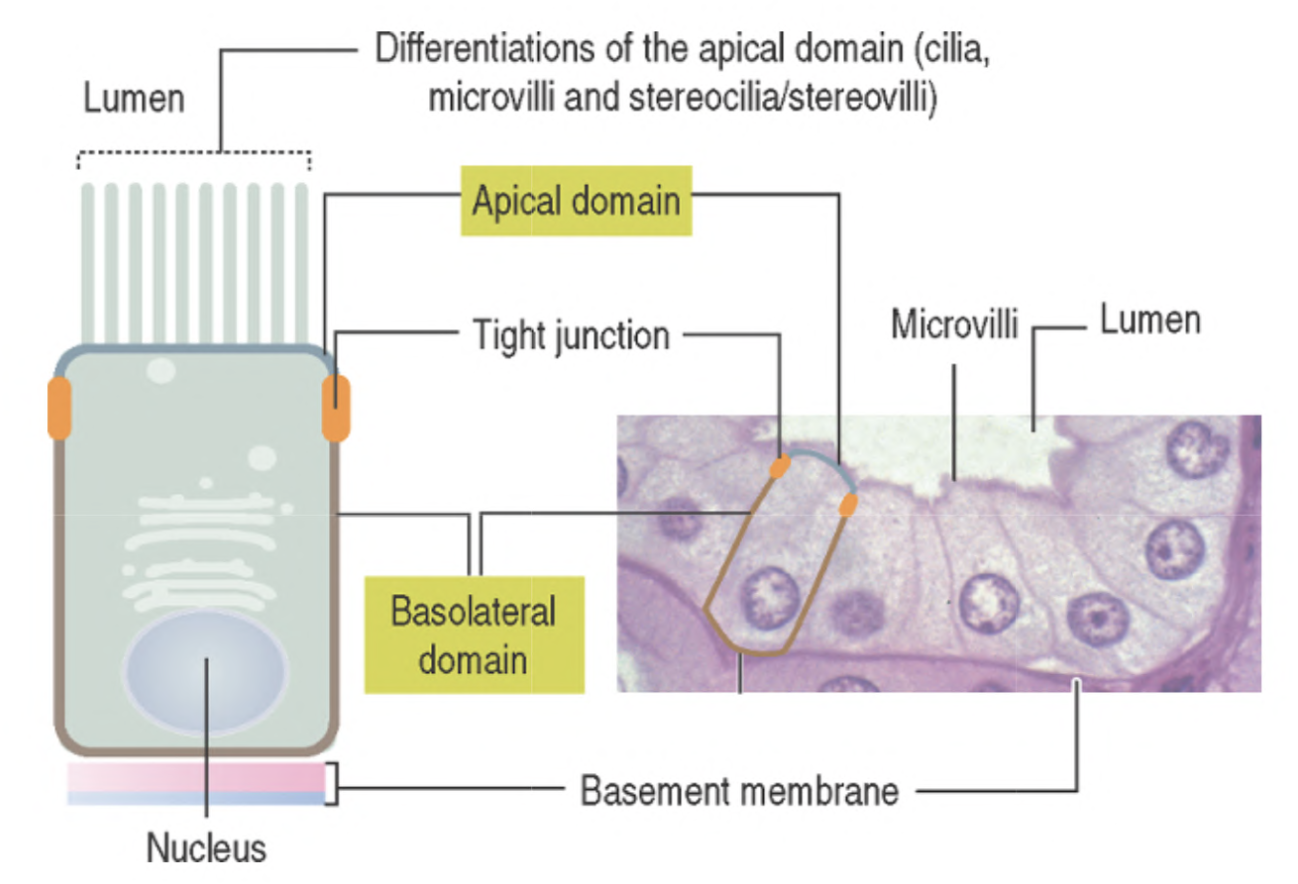
- The apical (uppermost) domain is exposed to the lumen or external environment and displays apical differentiations (cilia, microvilla, stereocilia).
- The lateral domain faces neighboring epithelial cells linked to each other by cell adhesion molecules and junctional complexes.
- Tight junctions that strictly attach these cells do not allow for proteins present in the basal domain to migrate to the apical domain.
- The basal domain is associated with a basal lamina that separates the epithelium from underlying connective tissue, representing the internal and nutritional supporting environment.
- The basal domain maintains the connection to the ECM.
- The basal lamina, of epithelial cell origin, is reinforced by components of the connective tissue.
- The basal lamina–connective tissue complex is the basement membrane.
From the functional perspective, sealing junctions segregate the plasma membrane of an epithelial cell into an apical domain and a basolateral domain.
This segregation is supported by the asymmetric distribution of transporting molecules, ensuring polarized secretory and absorptive functions of an epithelium.
For example,
the apical domain has structures important for the protection of the epithelial surface (such as cilia in the respiratory tract) or for the absorption of substances (such as microvilli in the intestinal epithelium).
In contrast, the basolateral domain facilitates directional transport functions prevented from trespassing the sealing junctions.
The nucleus can have different distributions:
- in the polar columnal cells we have the nucleus located in the basal domain,
- cuboidal cells have it in the center.
Important
- Epithelium is an avascular tissue, receives its nutrients from the vascular supply of the adjacent connective tissue.
- Tightly bound, closely packed cells, held together by junctional complexes, with little amount of extracellular matrix.
- Epithelium and connective tissue are separated from the basal lamina, and lay down on the basement membrane.
The Basement Membrane
It serves as reservoirs of growth factors that direct and fine-tune cellular functions.
Acellular region, as visible by light microscopy, is better defined by electron microscopy as having two constituents:
- the basal lamina, produced by epithelial cells,
- and the lamina reticularis (reticular lamina) manufactured by cells of the connective tissue.
https://unibo.smartzoom.com/s1241/course1776/f1777/i179
The basal lamina has two regions:
- the lamina lucida, a 50-nm-thick electron-lucent region just beneath the epithelium,
- consists mainly of the extracellular glycoproteins laminin and entactin as well as integrins and dystroglycans, transmembrane laminin receptors, that project from the epithelial cell membrane into the basal lamina.
- and the lamina densa, electron-dense region.
- comprises a meshwork of type IV collagen.
The lamina reticularis possesses fibronectin.
It’s a region of varying thickness, is manufactured by fibroblasts and is composed of type I and type III collagen.
It is the interface between the basal lamina and the underlying connective tissue, and its thickness varies with the amount of frictional force on the overlying epithelium.
http://www.histologyguide.com/slideview/MH-136-trachea/02-slide-1.html?x=47820&y=27660&z=100.0
Functions of the Basement Membrane
The main functions of basement membrane are:
- cell adhesion,
- diffusion barrier
- and regulation of cell growth.
- First, it forms an adhesion interface between epithelial cells and underlying extracellular matrix
- Second, the basement membrane acts as permeability barrier, with pore size depending on the charge and spatial arrangement of its component GAG.
- Third, basement membrane probably controls cell organization and differentiation by the mutual interaction of cell surface receptors and molecules in the extracellular matrix.
These interactions are the subject of intense research, particularly in the investigation of mechanisms that might prevent the spread and proliferation of cancer cells throughout the body.
Epithelia
- On the surface and lining layer(s)
- Cells close together
- No blood vessels
Histology classification
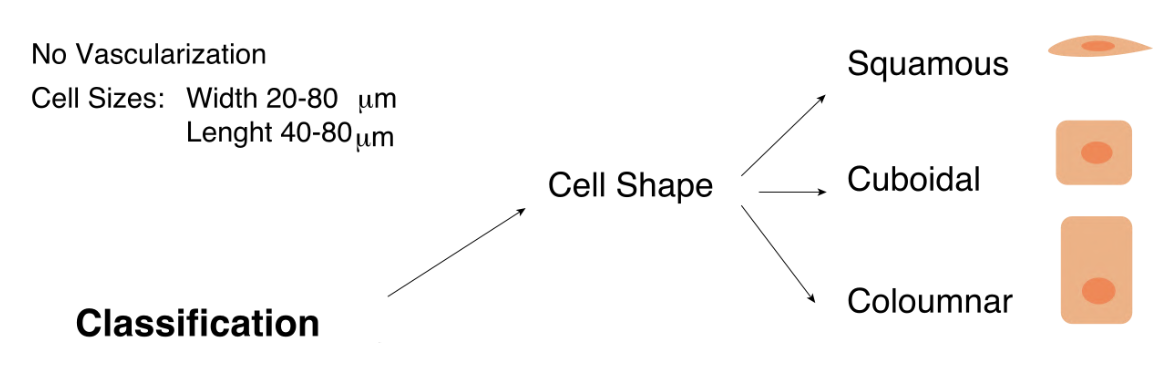
Classification of Epithelia
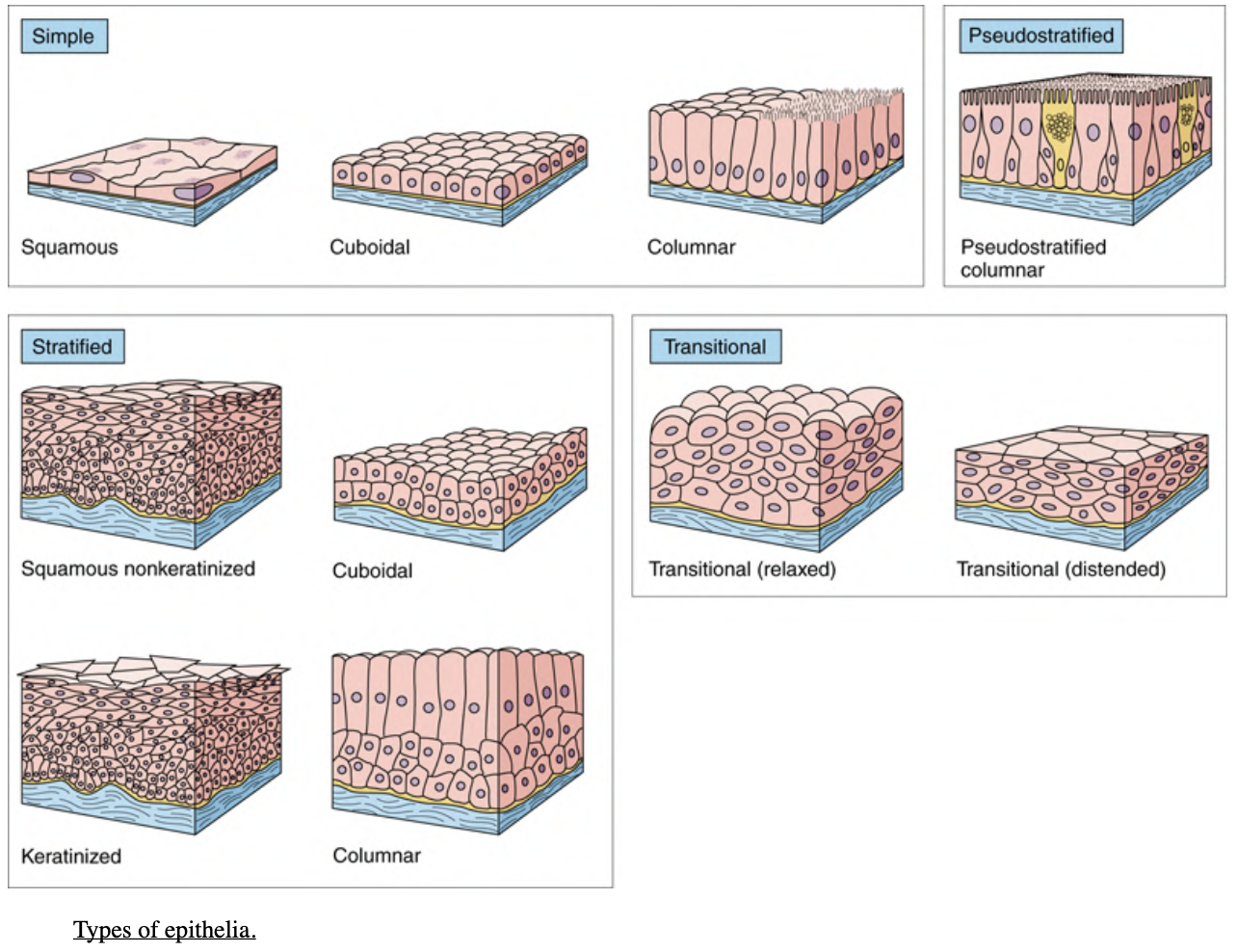
Epithelial membranes are classified according to the number of cell layers between the basal lamina and the free surface and by the morphology of the epithelial cells.
If the membrane is composed of a single layer of cells, it is called simple epithelium; if it is composed of more than one cell layer, it is called stratified epithelium.
The morphology of the cells may be:
- squamous (flat),
- cuboidal,
- or columnar when viewed in cross section.
Stratified epithelia are classified by the morphology of the cells in their superficial layer only.
In addition to these two major classes of epithelia, which are further identified by cellular morphology, there are two other distinct types:
- pseudostratified
- and transitional.
Histology Classification
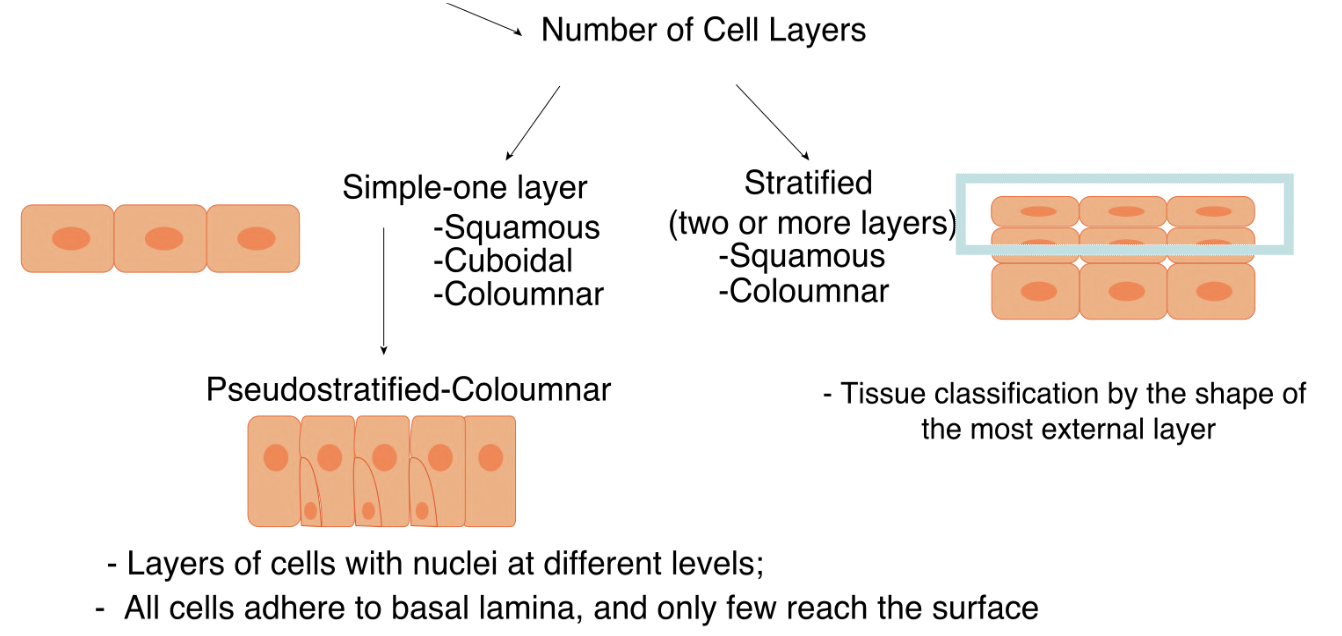
Simple Epithelia
Simple Squamous Epithelium
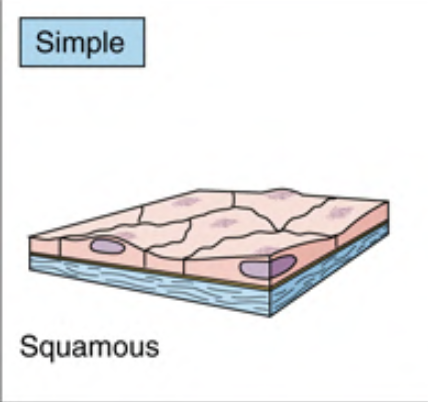
It’s composed of a single layer of tightly packed, thin polygonal cells.
When viewed from the surface, the epithelia sheet looks like a tile floor, with centrally placed nuclei.
Viewed in section, only some cells display nuclei because the plane section doesn’t encounter the nucleus.
Example
- Pulmunary alveoli
- Bowman capsule
- Endothelial lining of the blood vessels
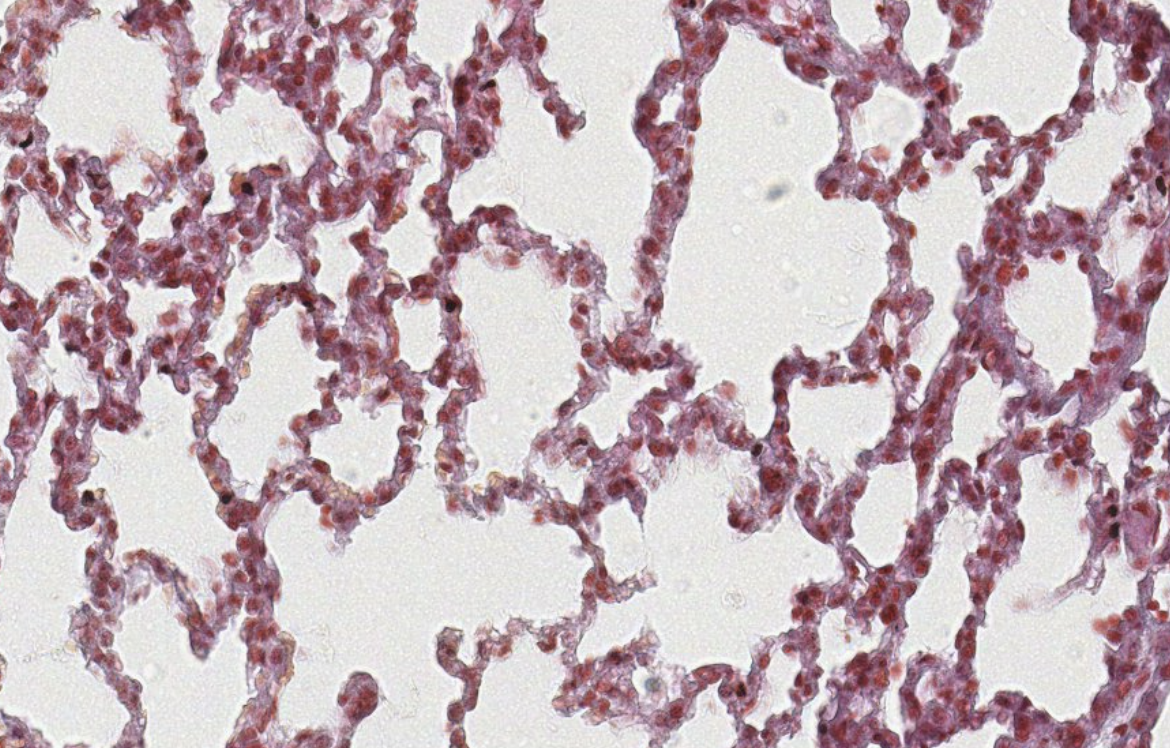
Classifying → 001 lung
To locate covering epithelium, look first at the empty spaces in the slide.
The covering epithelium is usually looking towards those empty spaces.
In the beginning, don’t zoom in, look at the big picture.
You can distinguish the cells by their nuclei.
001 lung slide → simple squamous epithelium.
these are the epithelia of the alveoli type 1.Then why are there clusters of cells sometimes? It’s usually collapsed tissue from the way it was collected. Always consider how the tissue was prepared and what consequences it might have on the structures you see.
Simple Cuboidal Epithelium
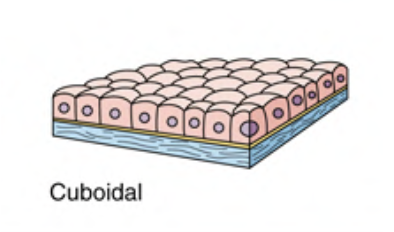
A single layer of cuboidal shaped cells.
Cells present a square profile with a centrally placed round nucleus.
Example
- Ducts of many glands
- Covering of the ovary
- Kidney tubules
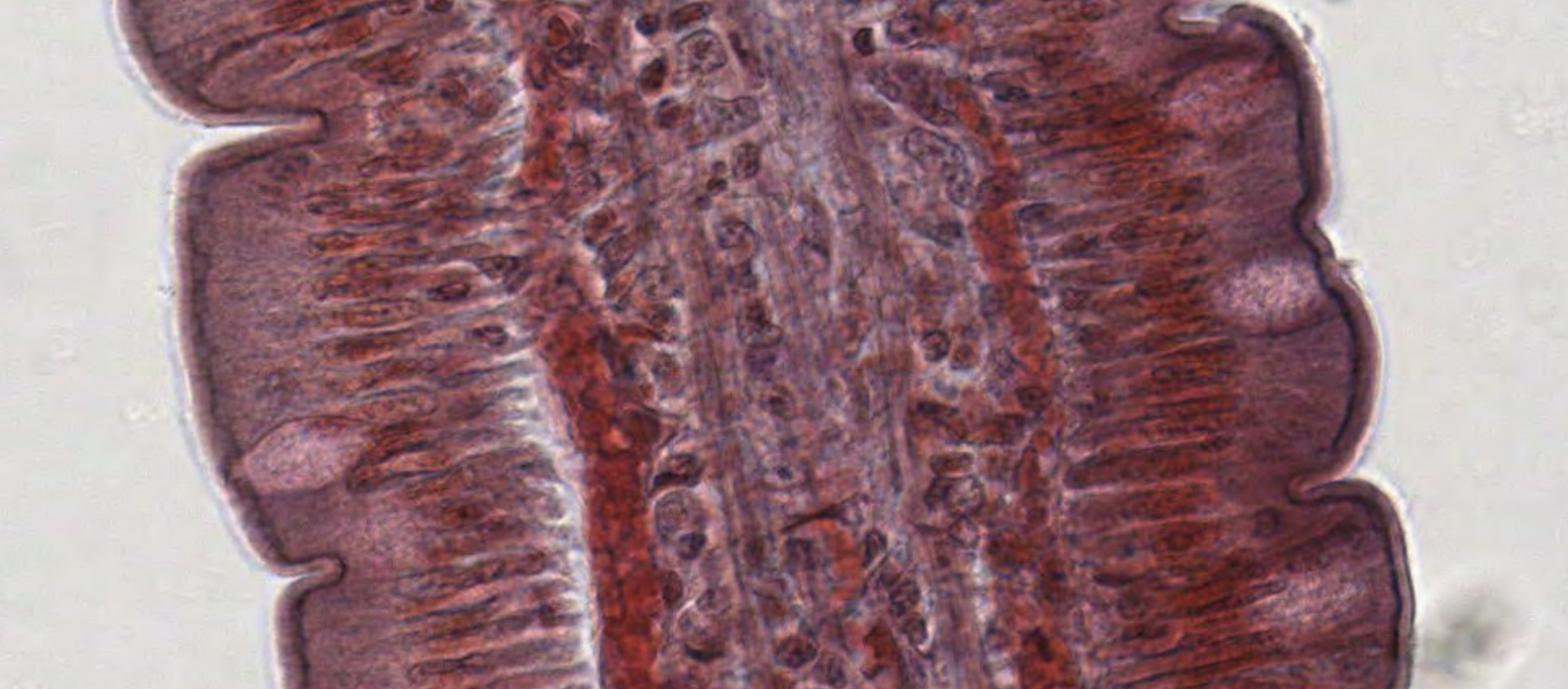
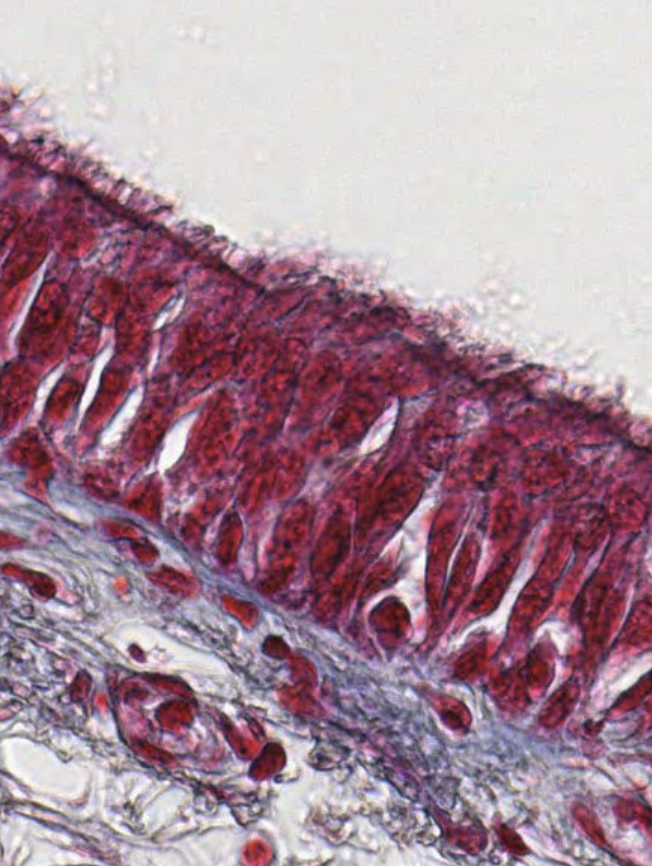
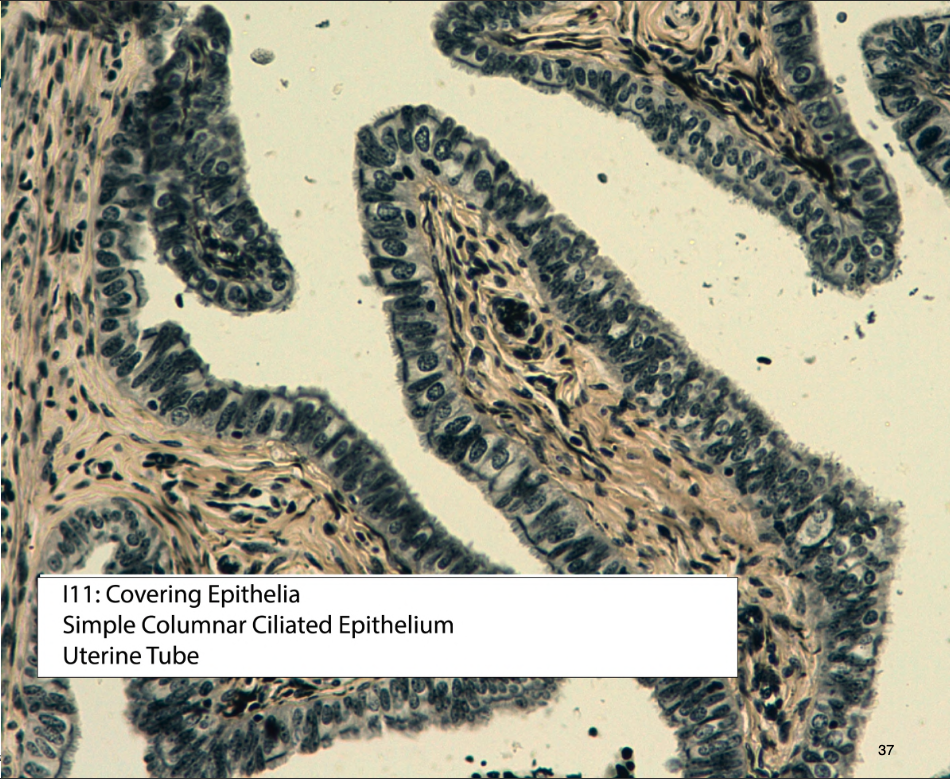
Simple Columnar (Cylindrical) Epithelium
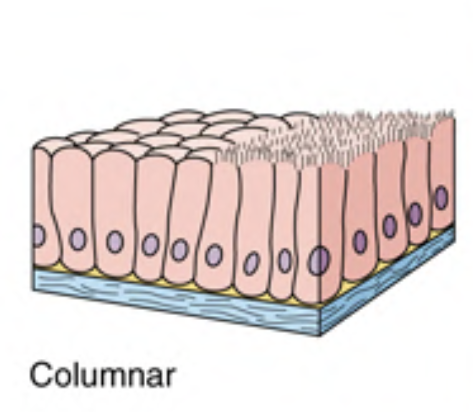
Single layer of tall, rectangular cells.
Nuclei are located at the same level in the basal half of the cell.
Example
- Digestive tract
- Gallbladder
- and large ducts of glands
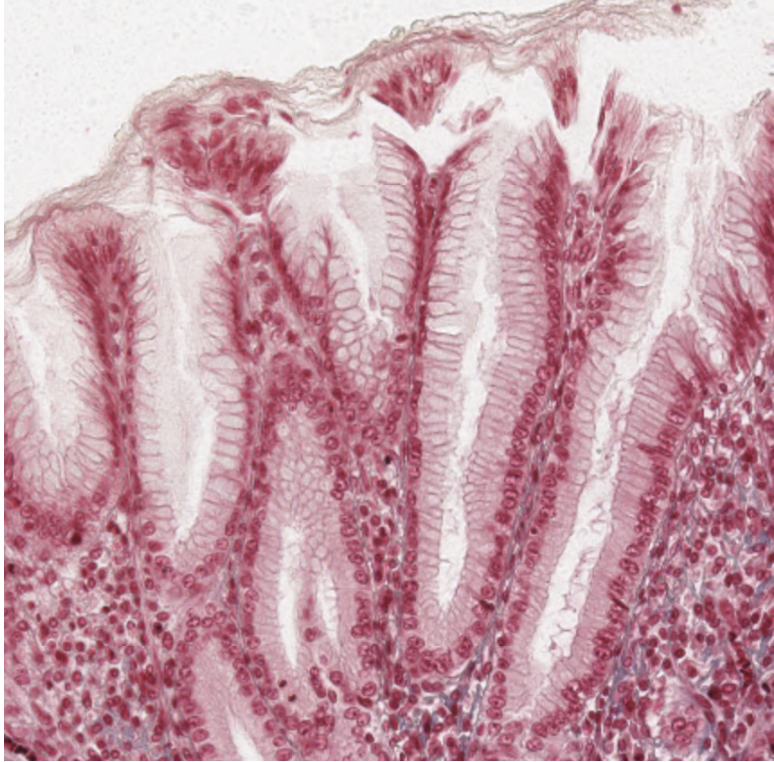
Simple columnar epithelium
Stratified Epithelia
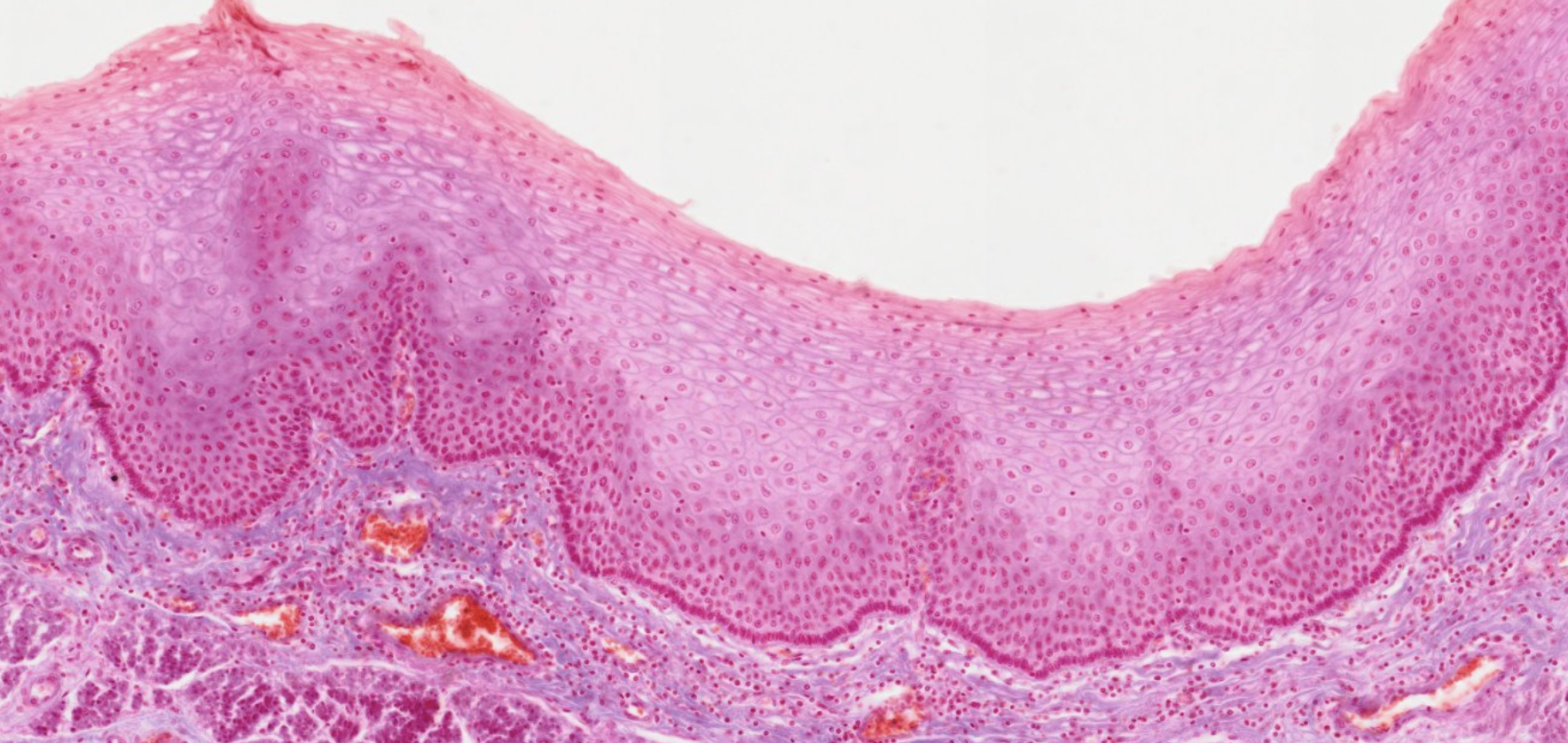
Stratified Squamous Epithelium
Stratified squamous epithelium is composed of several layers of cells.
Only the deepest layer is in contact with the basal lamina.
Example
- Lining the mouth
- Oral pharynx
- Vagina
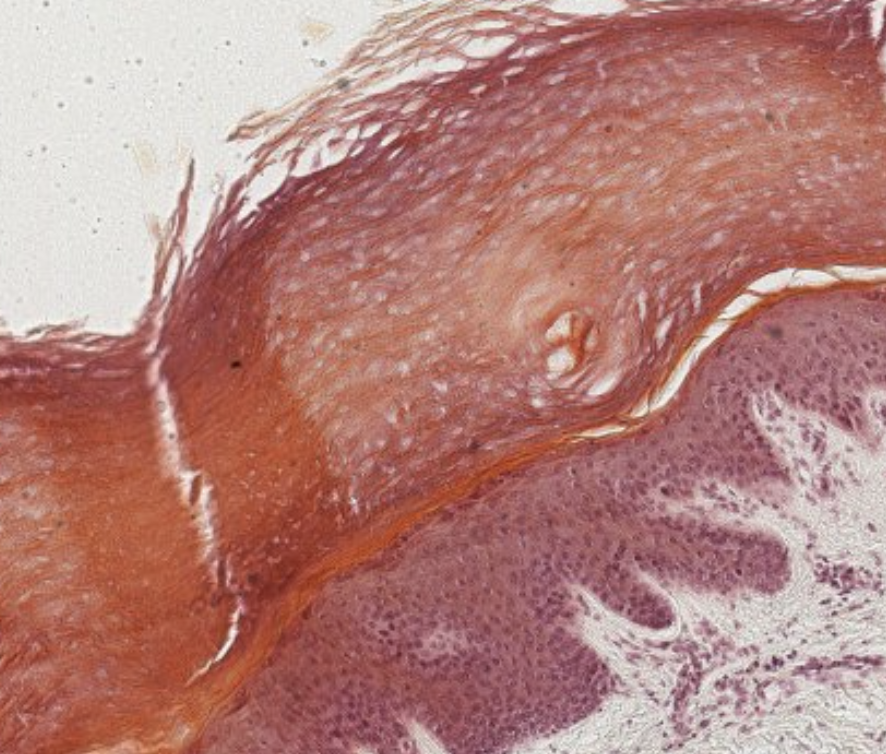
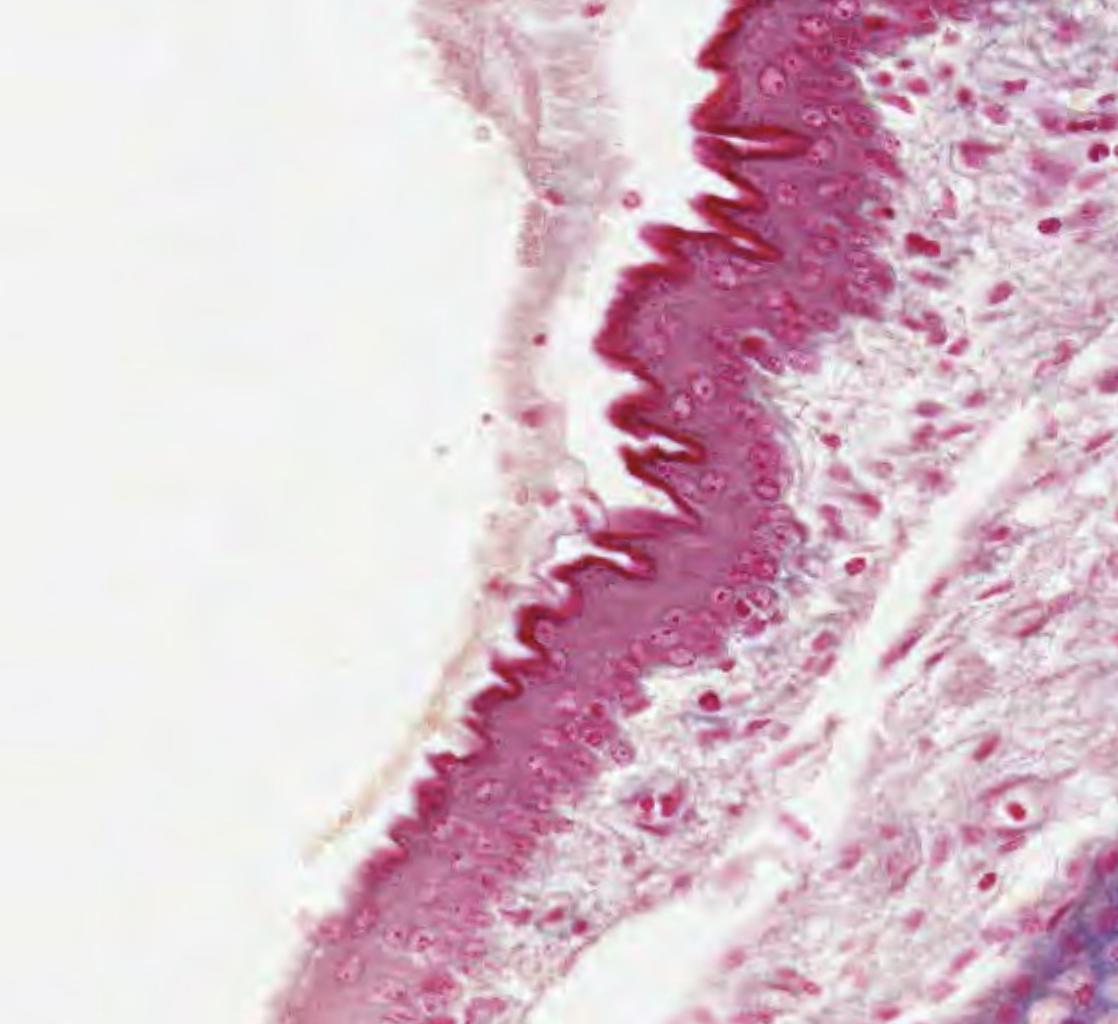
Stratified Squamous (Keratinized) Epithelium
Cells of the outmost layer are dead (no nucleus), non-nucleated and are filled with keratin.
Thick layer of keratin resists friction and it is impermeable to water.
By consequence, the tissues that present this type of epithelium are the ones destined to be exposed to friction, like the palm of the hand.
Why not inside the body? Because we don’t need it to stay “wet” since the inside of the body is not subjected to dehydration.
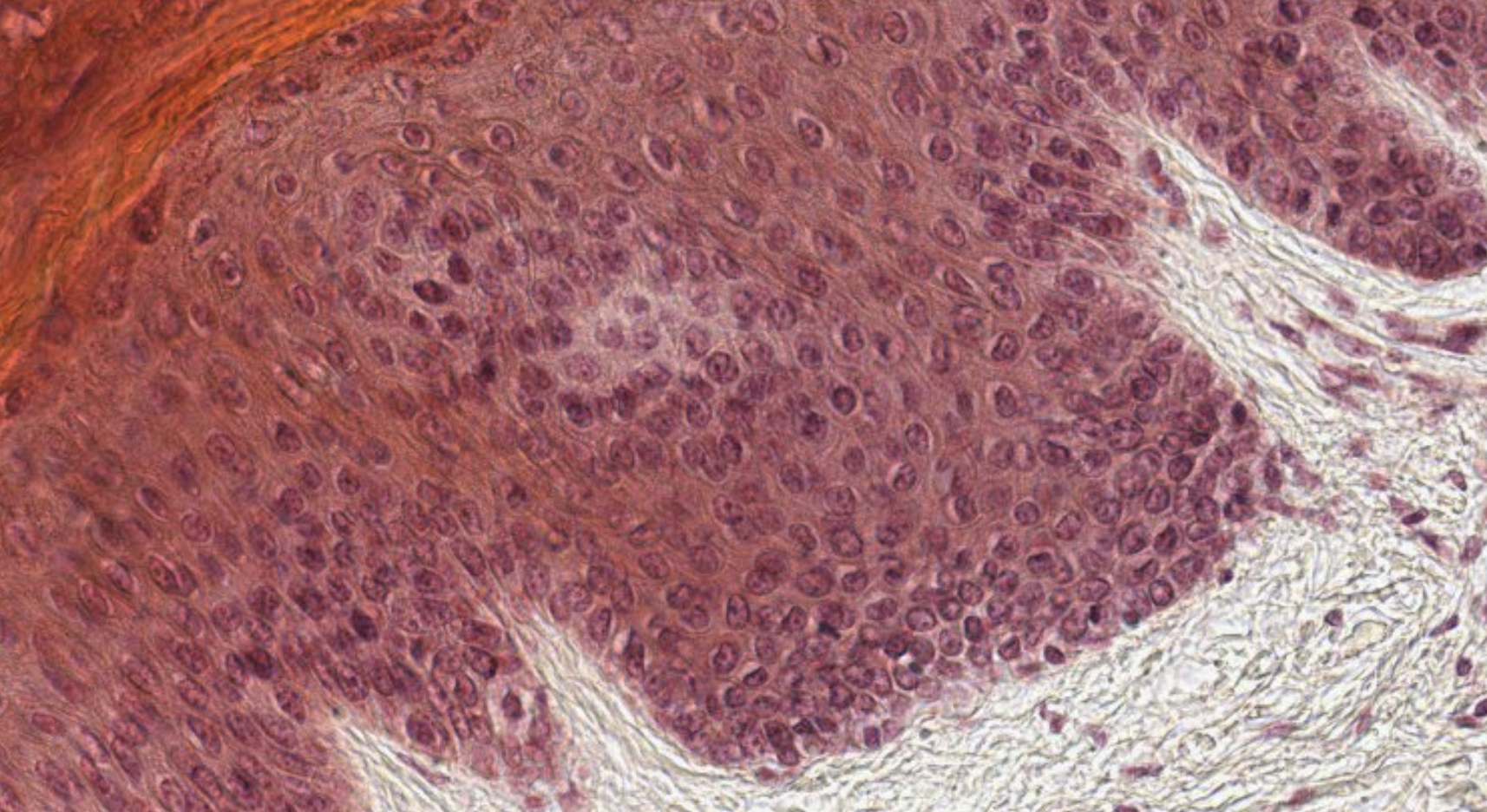
Classifying 005 skin
There isn’t only epithelium in this slide. It’s thick part, clearly stratified.
The squamous shape at the basal membrane tells us this is a stratified squamous epithelium. The cells at the bottom are rounded and crowded, so we can classify that as the basal layer. Those cells are migrating to the surface via “stratus spinosum” differentiation path. While they move to the periphery, we can see granules. Those granules are keratin, leading the cell to the stratus granulosum.
What’s this??? Those are dead, keratinized cells. Great! Stratified squamous keratinized epithelium.
Classifying this... 006 ovary??
cuboidal somehting. okay
Classifying... 008 small intestine
This looks odd. Simple columnar. There are microvilli but they’re not visible. We can see that the villi that we can see have “brush borders” which is the visual result of the appearance of the microvilli.
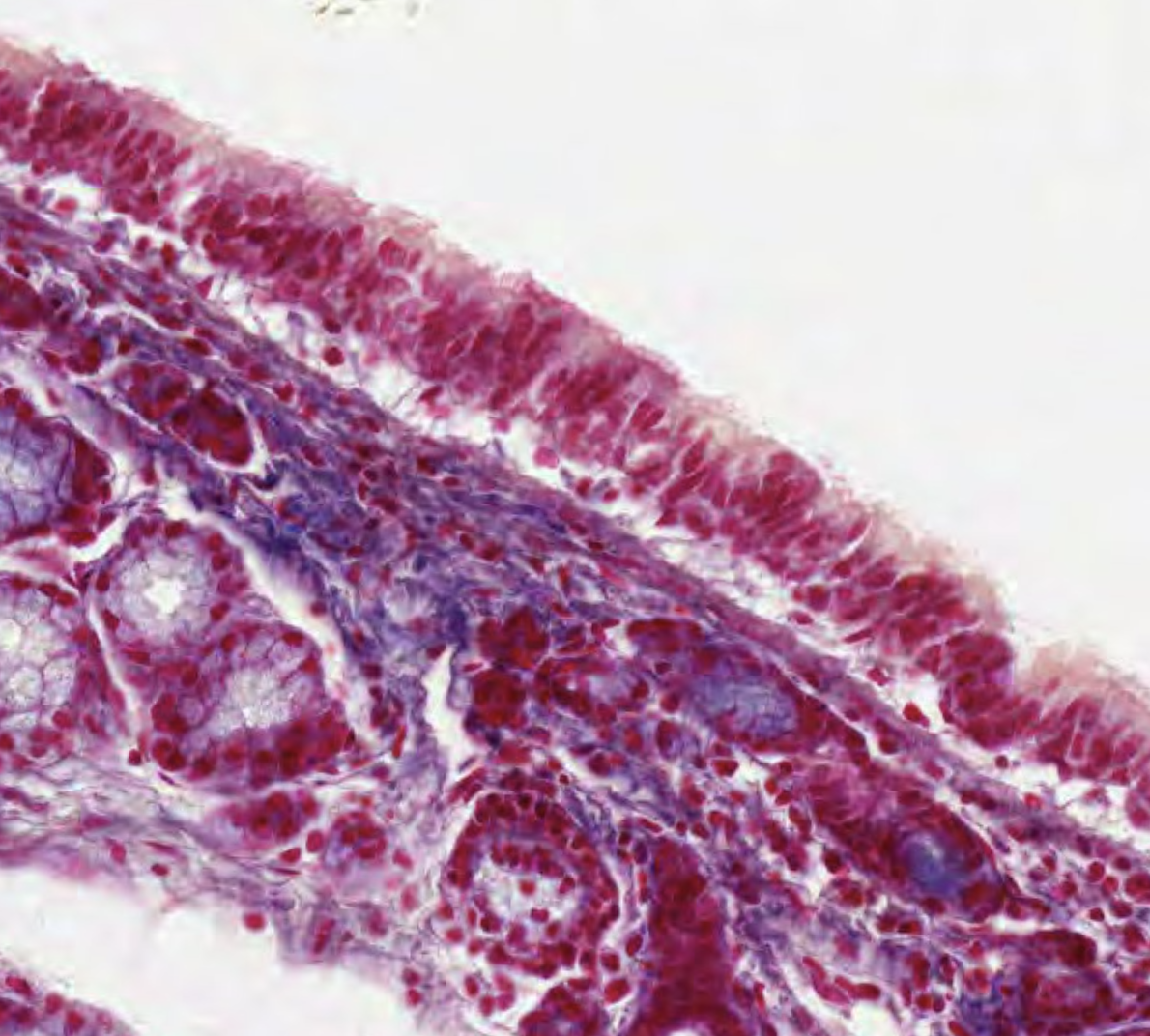
Classifying Trachea
This is stratified squamous. What’s here??? The white gray blobs?? Oh. Keratin. But this is an inner tissue? Why is it keratinized? Because food passes through there? this is the upper area of the tube. Ah. This is not human tissue. Areas of the esophagous that are close to the surface in animals (not humans) tend to have keratin.
This instead is pseudostratified with cilia. Seeing cilia can help recognize that the tissue is pseudostratified.
Stratified Cuboidal/Columnar Epithelium
Two layers of cuboidal cells exist only in the duct of some sweat glands,
Special Types
Pseudostratified Epithelium
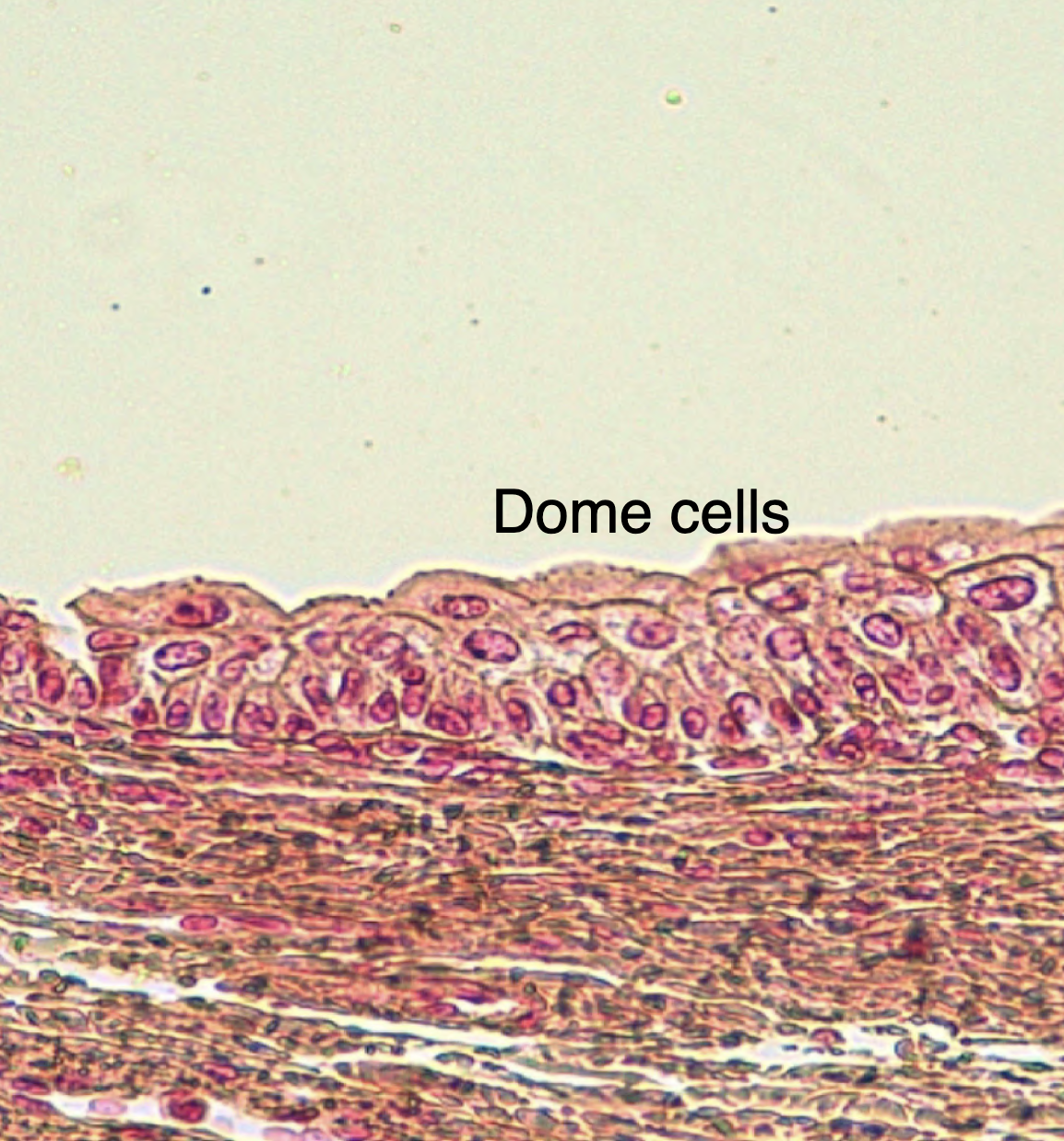
Transitional Epithelium (Urothelium)
Several layers of cells with the outmost layer larger and composed of dome/umbrella shaped cells.
It was erroneously believed to be in transition between stratified columnar and squamous epithelium.
Distinct type located in the urinary system
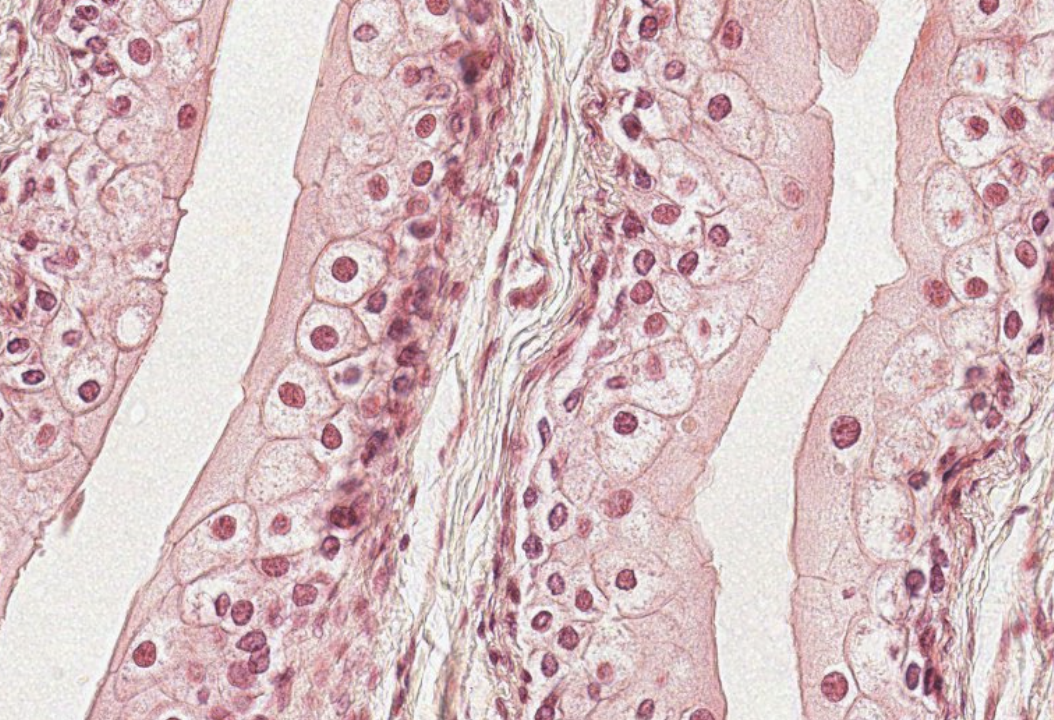
The most superficial cells are occasionally binucleated and become flattened when the bladder is filled with urine (transitional state). These cells can stretch!
Transitional Epi!
These dome cells are the ones that are helping you classify this tissue as a transitional epithelium.
This is a relaxed bladder. These dome cells look like umbrellas covering other cells!
This is a full bladder. These fully stretched dome cells are smooth and completely flat!! Brazy…
https://unibo.smartzoom.com/s1241/course1776/f1777/i1810/
Histology
More differences to classify:
- Polarity and cell surface specializations
- Cell-cell Junctions
- Epigenetic regulation of stem cell homeostasis
Apical Domain & Surface Specializations
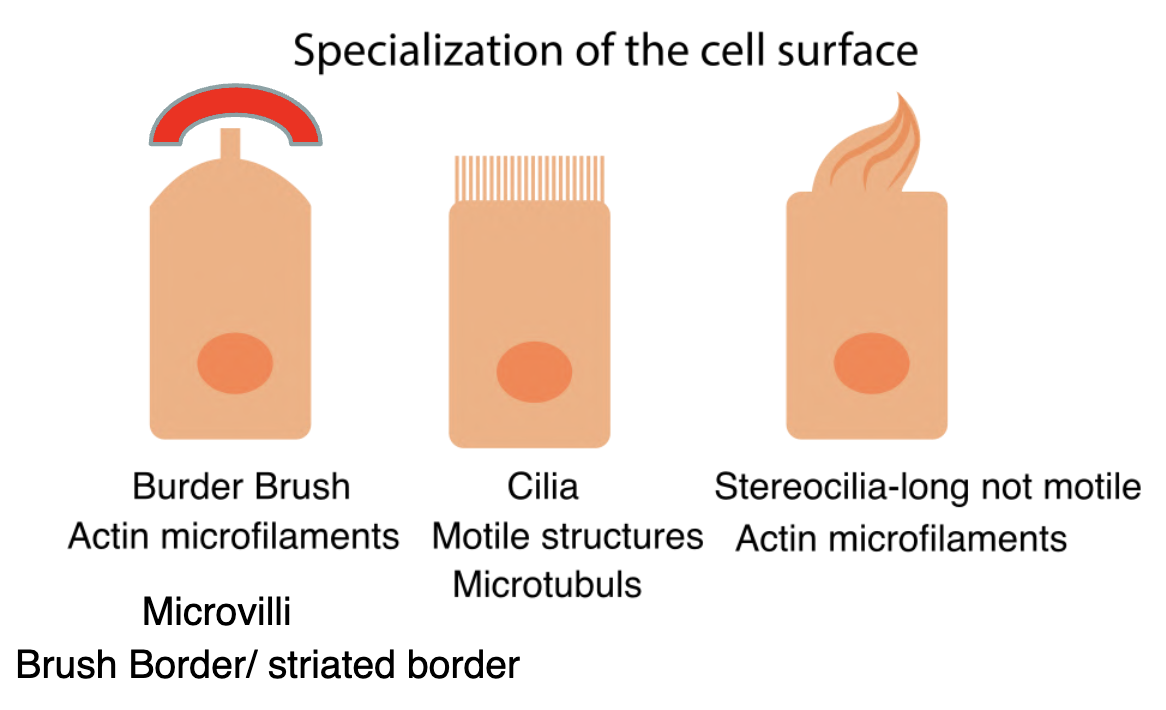
Cilia
There are two types of **cilia:
- multiple motile cilia
- and a single or a primary non-motile cilium.
Ciliogenesis, the assembly process of both types of cilia, is initiated by the basal body, a structure originated from a basal body precursor located in the centrosome.
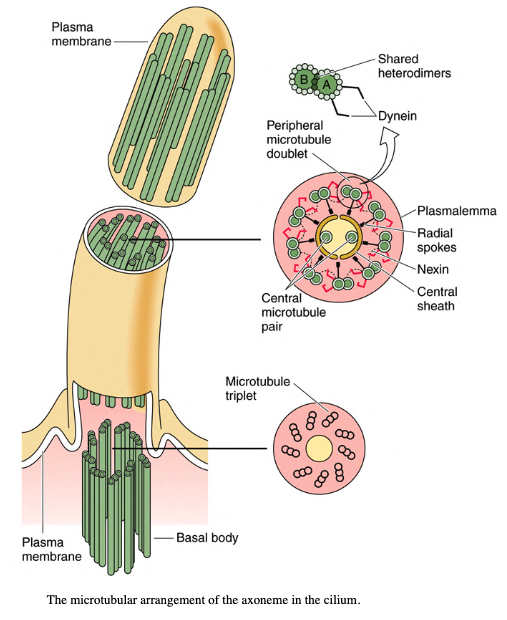
Cilia are motile, hair-like projections (diameter, 0.2 μm; length, 7 to 10 μm) that emanate from the surface of certain epithelial cells.
In the ciliated epithelia of the respiratory system (e.g., trachea and bronchi) and in the oviduct, there may be hundreds of cilia on the luminal surface of the cells.
The core of the cilium contains a complex of microtubules called the axoneme.
The axoneme is composed of a constant number of longitudinal microtubules arranged in a consistent 9 + 2 centrally placed microtubules (singlets) are evenly surrounded by nine doublets of microtubules.
Microvilli / Single or primary non-motile cilium
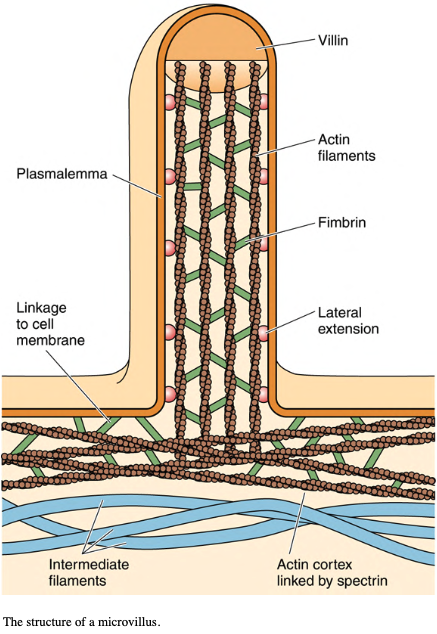
Microvilli are cylindrical, membrane- bound projections of the cytoplasm emanating from the apical surface of the cells.
Microvilli represent the striated border/ brush border of the intestinal absorptive cells and in the kidney proximal tubule cells observed by light microscopy.
In less active cells, microvilli may be sparse and short; in intestinal epithelia, where the major function is transport and absorption, they are crowded and 1 to 2 μm in length. Increasing the surface area of the cells.
Each microvillus contains a core of 25 to 30 actin filaments, cross-linked by villin, attached at the tip and extending into the cytoplasm, where the actin filaments are embedded into the terminal web.
The terminal web is a complex of actin and spectrin molecules as well as intermediate filaments located at the cortex of the epithelial cells.
Microvilli/brush border or striated border
How cells define polarity
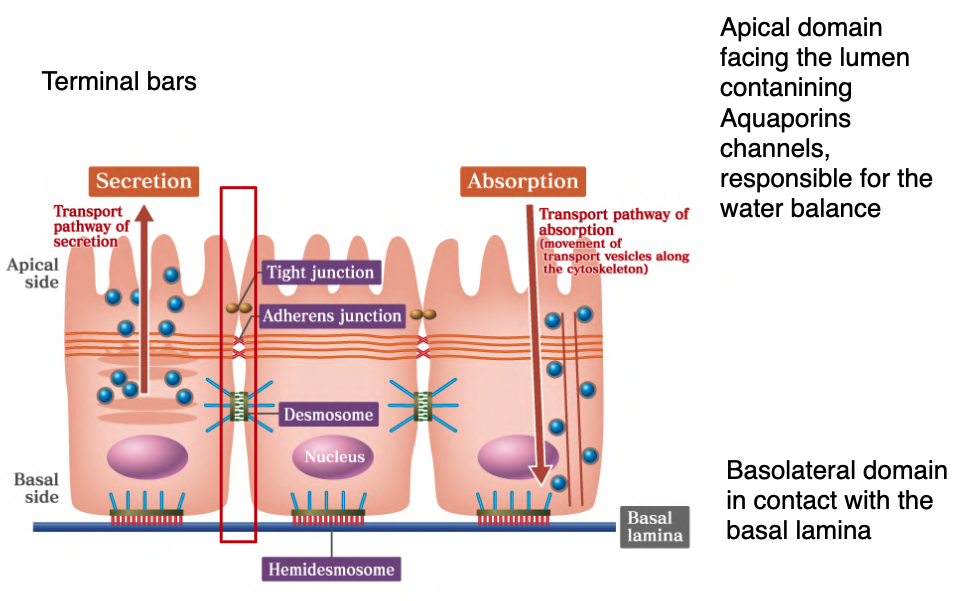
Cell-to-Cell Junctions (Terminal Bars)
Junctional complexes are specialized regions of the plasma membrane that categorize into three functional types:
- Occluding junctions: Form impermeable barriers.
- Anchoring junctions: Maintain cell-to-cell and cell-to-lamina structural integrity.
- Communicating junctions: Permit movement of signaling molecules between cells.
1. Occluding Junctions (Tight Junctions / Zonulae Occludentes)
These are the most apically located junctions. They form a “belt-like” seal that encircles the entire circumference of the cell, fusing adjacent plasma membranes.
Key Functions
- Prevents material from passing from the lumen into the connective tissues (paracellular barrier).
- Maintains cell polarity by preventing membrane proteins from migrating between apical and basolateral domains.
Molecular Components
- Claudins: The primary proteins (calcium-dependent).
- Occludins, Nectins, and JAMs: Supporting transmembrane proteins.
- ZO-1, ZO-2, ZO-3: Cytoplasmic complexes that link claudins to the cytoskeleton.
2. Anchoring Junctions
These junctions provide mechanical stability by linking the cytoskeletons of adjacent cells or the cell to the extracellular matrix.
Zonulae Adherentes
Zonulae adherentes are anchoring junctions of epithelial cells are located just basal to the zonulae occludentes and also encircle the cell.
The intercellular space of 15 to 20 nm between the two adjacent cell membranes is occupied by cadherins.
These Ca+-dependent proteins of the cell membrane are transmembrane linker proteins.
Their intracytoplasmic aspect binds to a web of actin filaments that are attached to each other and to the cell membrane by vinculin, catenin and α**-actinin.**
Desmosomes (Maculae Adherentes)
Desmosomes are the last of the three components of the junctional complex.
Two (Hemidesmosomes) disk-shaped forming the attachment plaques are located opposite each other on the cytoplasmic side of the plasma membranes of adjacent epithelial cells - Each plaque is composed of a series of attachment proteins.
The intercellular space is of 30 nm and it is occupied with the extracellular domains of:
- Desmocollins and desmogleins, are both cadherins (Calcium-dependent adhesion)
The outer dense plaque is adhering to the cytoplasm. It’s composed of glycoproteins (plakoglobins and plakophilins held together by desmoplakins).
Desmoplakins contact keratins (IF)
Hemidesmosomes - Type I
Hemidesmosomes resemble half desmosomes and serve to attach the basal cell membrane to the basal lamina.
Type I hemidesmosome is more complex than II and is present in the basal layer of cells of the stratified squamous epithelia and pseudostratified epithelia.
- α6β4 integrin molecules
- Tonofilaments of K5 and K14 intermediate filaments
- Plakin proteins that bind to tonofilaments and α6β4 integrin
- Erbin facilitates the binding of integrin to plakins
- CD151 that recruits integrins to ensure the formation of hemidesmosome
Attachment plaques, composed of desmoplakins and other associated proteins, are present on the cytoplasmic aspect of the plasma membrane.
Keratin tonofilaments insert into these plaques, unlike those in the desmosome, where the filaments enter the plaque and then make a sharp turn to exit it. The cytoplasmic aspects of transmembrane linker proteins are attached to the plaque, whereas their extracellular moieties bind to laminin and type IV collagen of the basal lamina.
Attachment plaques, composed of desmoplakins and other associated proteins, are present on the cytoplasmic aspect of the plasma membrane.
Keratin tonofilaments insert into these plaques, unlike those in the desmosome, where the filaments enter the plaque and then make a sharp turn to exit it.
The cytoplasmic aspects of transmembrane linker proteins are attached to the plaque, whereas their extracellular domains bind to laminin and type IV collagen of the basal lamina.
Basement Membrane
The lamina reticularis possesses fibronectin.
The lamina reticularis, a region of varying thickness, is manufactured by fibroblasts and is composed of type I and type III collagen. It is the interface between the basal lamina and the underlying connective tissue, and its thickness varies with the amount of frictional force on the overlying epithelium.
53Hemidesmosomes - Type II
Hemidesmosomes Type II are present in the basal plasma membrane of simple columnar epithelial cells. They have large concentration of integrin molecules, which form bonds with keratin-8 and 18.
Both require the presence of calcium ions to maintain the attachment to the basal lamina.
Junctional complexes, gap junctions, and hemidesmosomes.
54• Where do we expect to have a problem in presence of a mutation on desmosomal proteins?
Clinical Correlations & Pathology
Autoantibodies against desmosomal proteins are responsible for a skin disease:
Pemphigus vulgaris
Treatments: Systemic steroids and immunosuppressive agents
56
Copyright © 2017 by Elsevier, Inc. All rights reserved.Naxos Syndrome
• Middle East and in the Greek Island: Naxos
• Mutations in desmoplakins and plakoglobins
Keratoderma of the palm of the hands and of the feet
Cardiomiopathy involving right ventricular arrhytmia
57
_Copyright © 2017 by Elsevier, Inc. All rights reserved._Generalized Junctional Epidermolysis Bullosa (JEB)
• Skin and mucosal blisters and erosions occur within the lamina lucida of the basement membrane upon minor trauma
• JEB is caused by mutations in LAMA3, LAMB3 or LAMC2 genes
Clinical picture of the patient showing
At the first surgery, the patient had complete epidermal loss on ~80% massive epidermal loss.
https://www.ncbi.nlm.nih.gov/pubmed/29144448
Copyright © 2017 by Elsevier, Inc. All rights reserved.
58Experimental plan
4-cm2 biopsy, taken from a currently non-blistering area of patient’s left inguinal region, was used to establish primary keratinocyte cultures, which were then transduced with a retroviral vector (RV) expressing the full-length LAMB3 cDNA under the control of the
Moloney leukaemia virus (strong promoter)
Center for Regenerative Medicine “Stefano Ferrari”, Department of Life Sciences,
University of Modena and Reggio Emilia, Modena, Italy
Copyright © 2017 by Elsevier, Inc. All rights reserved. 59Experimental plan
Copyright © 2017 by Elsevier, Inc. All rights reserved. 60_Copyright © 2017 by Elsevier, Inc. All rights reserved._ 61Complete recovery after 21 months
Copyright © 2017 by Elsevier, Inc. All rights reserved. 62# Communicating Junctions (Gap Junctions)
Gap junctions are widespread in epithelial tissues, neurons, muscle cells and cardiac cells, but NO skeletal muscle cells.
The GJs mediate intercellular communication by permitting the passage of small molecules.
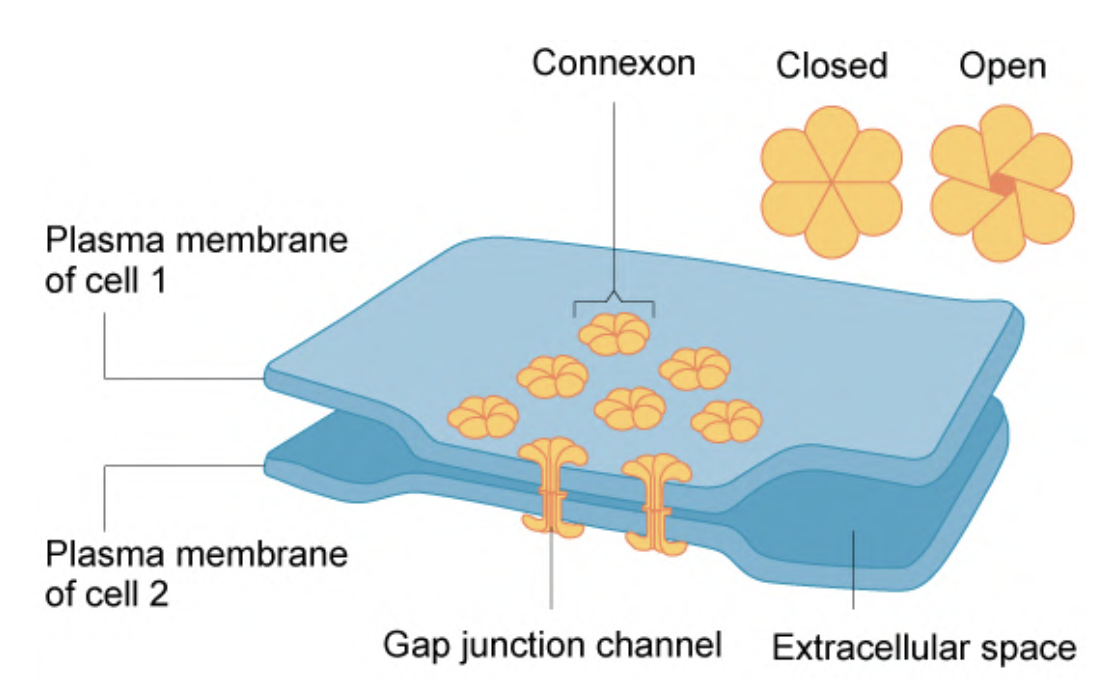
They are built by six closely packed transmembrane proteins (connexins) that assemble to form structures called connexons, aqueous pores through the plasma membrane extending into the intercellular space.
Two connexons in adjacent cells are aligned, forming a Gap Junction.
Junctional complexes, gap junctions, and hemidesmosomes.
Copyright © 2017 by Elsevier, Inc. All rights reserved.
3. Gap junctions or communicating junctions
Two connexons in adjacent cells are aligned, forming a Gap Junction.
The two connexons fuse, forming the functional intercellular communication channel.
Gap junctions are regulated, so they may be opened or closed.
Although the opening and closing mechanism is not understood, it has been shown experimentally that a decrease in cytosolic pH or an increase in cytosolic Ca2+ concentrations closes channels.
Conversely, high pH or low Ca2+ concentration opens the channels.
Gap junctions functions for sharing molecules for coordinating physiological continuity within a particular tissue
For example, when glucose is needed in the bloodstream, the nervous system stimulates hepatocytes to initiate glycogen breakdown.
Because not all the hepatocytes are individually stimulated, the signal is propagated to other hepatocytes by gap-junctions.
• Heart cells are also coordinated by gap-junctions
• Also gut muscle during peristalsis are coordinated by gap-junction
Copyright © 2017 by Elsevier, Inc. All rights reserved.
65Clinical Correlations
A number of cardiac arrhythmias have been linked to gap junction anomalies. These are due to wrong number of gap junctions plaques or to the wrong location, in the lateral membrane instead of being at the end of the cells, compared to the healthy ventricular myocardial cells.
66
_Copyright © 2017 by Elsevier, Inc. All rights reserved._Renewal of epithelial cells
• Epithelial tissues exhibit a high turnover rate, which is related to their location and function.
• Epidermis takes approximately 28 days
• Cells lining the intestine are replaced every 4 to 6 days.
Copyright © 2017 by Elsevier, Inc. All rights reserved.
67Clinical correlation
• Cells in an epithelium may transform into another epithelial type: metaplasia.
• Pseudostratified ciliated epithelium in heavy smokers undergo squamous metaplasia (transform into stratified squamous epithelium)
• Tumors that arise from epithelial cells are known as carcinoma
• Tumors that arise from glandular epithelium are known as adenocarcinoma
The Integument (Skin)
The integument, composed of skin sweat glands, sebaceous glands, hair, and nails, is the largest organ, constituting 16% of the body weight.
Comparison of thick skin and thin skin.
Besides providing a cover for the underlying soft tissues, skin performs many additional functions, including
- protection against injury, bacterial invasion, and desiccation;
- regulation of body temperature;
- reception of sensations from the environment (e.g., touch, temperature, and pain);
- excretion from sweat glands;
- absorption of ultraviolet (UV) radiation from the sun for the synthesis of vitamin D.
Integument
Skin consists of two layers: an outer epidermis and a deeper connective tissue layer, the dermis.
Comparison of thick skin and thin skin.
The epidermis is composed of stratified squamous keratinized epithelium. Lying directly below and interdigitating with the epidermis is the dermis, composed of dense, irregular collagenous connective tissue.
The interface between the epidermis and dermis is formed b y t h e d e r m a l r i d g e s (papillae), which interdigitate with invaginations of the epidermis called epidermal ridges**.**
Epidermis
Comparison of thick skin and thin skin.
The epidermis is 0.07 to 0.12 mm in thickness over most of the body, with localized thickening on the palms of the hands and the soles of the feet (where it may be as much as 0.8 mm and 1.4 mm in thickness, respectively).
Keratinocytes, which form the largest population of cells, are arranged in five recognizable layers; the remaining three cell types:
Langerhans cells (antigen presenting cells derived from precursor in the bone marrow, modified macrophages),
Merkel cells (have mechanoreceptors and secrete neurocrine like substances, similar to
Diffuse Neuro Endocrine System),
Melanocytes derive from the neural crest have processes known as dendrites, produce melanin responsible for pigmentation
Because keratinocytes are being continually sloughed from the surface of the epidermis, this cell population must continually be renewed. Renewal is accomplished through mitotic activity of the keratinocytes in the basal layers of the epidermis and as the new cells are forming, the cells above continue to be pushed toward the surface. Along their way to the surface, the cells differentiate and begin to accumulate keratin filaments in their cytoplasm. Eventually, as they near the surface, the cells die and are sloughed off, a process that takes 20 to 30 days.
Comparison of thick skin and thin skin.
Layers of the Epidermis
Because of the cytomorphosis of keratinocytes during their migration from the basal layer of the epidermis to its surface, five morphologically distinct zones of the epidermis can be identified.
From the inner to the outer layer, these are the
- stratum basale (germinativum)
- **stratum spinosum
- stratum granulosum (due to keratohyalin granules)
- stratum lucidum, and
- stratum corneum.
Comparison of thick skin and thin skin.
Skin is classified as thick or thin according to the thickness of the epidermis. However, these two types also are distinguished by the presence or absence of certain epidermal layers and the presence or absence of hair.
Dermis
The region of the skin lying directly beneath the epidermis, called the dermis is divided into two layers: the superficial, loosely woven papillary layer and the deeper, much denser reticular layer.
The dermis is composed of dense, irregular collagenous connective tissue, containing mostly type I collagen fibers and networks of elastic fibers, which support the epidermis and bind the skin to the underlying hypodermis (superficial fascia).
Comparison of thick skin and thin skin.
Comparison of thick skin and thin skin.
The superficial papillary layer of the dermis is uneven where it interdigitates with the epidermis, forming the dermal ridges (papillae).
It is composed of a loose connective tissue whose thin type III collagen fibers and elastic fibers are arranged in loose networks.
The interface between the papillary layer and reticular layer of the dermis is indistinguishable. Characteristically, the reticular layer is composed of dense, irregular collagenous connective tissue, displaying thick type I collagen fibers, which are closely packed into large bundles lying mostly parallel to the skin surface. Sweat glands, sebaceous glands, and hair follicles, all derived from the epidermis, invade the dermis and hypodermis during embryogenesis, and remain there permanently.
Renewal & Epigenetic Regulation
Epigenetic events controlling proliferative potential in the basal layer, as well as lineage commitment and differentiation,
Stratified epithelium in which proliferation occurs exclusively in the basal layer (stratum basale). Post-mitotic cells migrate and differentiate through the different layers of the epidermis until they are ultimately shed from the stratum corneum.
CBX, chromobox; DNMT, DNA methyltransferase; EDC, epidermal differentiation complex; HDAC, histone deacetylase;
_Epigenetic regulation of epidermal stem cell homeostasis
• Histone acetylation leads to loosening of the chromatin and therefore greater accessibility for the transcriptional machinery.
• DNMT1 (DNA methyltransferase) DNA (de)methylases levels in the epidermis are highest in undifferentiated basal epidermal progenitor cells and decrease with cellular differentiation
The chromatin state is dynamic during epidermal differentiation.
Histone H3 Lys27 trimethylation (H3K27me3) marking is highly locus specific, whereas histone acetylation and DNA methylation generally decrease during differentiation.
Take Home Message
- Cilia/Microvilli/Stereocilia composition and function
- Junctional Complexes
- Epidermal Receptor Homeostasis
- Methylation and Acetylation differentiation markers
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1777/i7776/
Squamous stratified.
TARGET DECK: MED::I::Morphology and Development::Histology::03 - Epithelium
What are the four basic tissue types and their functions?
- Connective → Support
- Muscle → Movement
- Nervous → Control and communication
- Epithelial → Cover and protect
What embryonic germ layer gives rise to the liver, pancreas, and GI tract?
Endoderm
What embryonic germ layer gives rise to skin, oral mucosa, and mammary glands?
Ectoderm
What embryonic germ layer gives rise to serous membranes and kidney?
Mesoderm
What determines epithelial cell polarity?
Distribution of plasma membrane proteins and lipids and rearrangement of the cytoskeleton
What is the basement membrane composed of?
- Basal lamina (produced by epithelial cells): lamina lucida + lamina densa
- Lamina reticularis (produced by fibroblasts): type I and III collagen + fibronectin
What are the three main functions of the basement membrane?
- Cell adhesion (interface between epithelial cells and ECM)
- Permeability barrier (pore size depends on GAG charge/arrangement)
- Regulation of cell organization and differentiation
What is the molecular composition of the lamina lucida?
Laminin, entactin, integrins, and dystroglycans (transmembrane laminin receptors)
What is the lamina densa composed of?
A meshwork of type IV collagen
How is stratified epithelium classified?
By the morphology of the cells in the superficial (outermost) layer only
Where is simple squamous epithelium found?
- Pulmonary alveoli
- Bowman’s capsule
- Endothelial lining of blood vessels
Where is simple cuboidal epithelium found?
- Ducts of many glands
- Covering of the ovary
- Kidney tubules
Where is simple columnar epithelium found?
- Digestive tract
- Gallbladder
- Large ducts of glands
What characterizes stratified squamous keratinized epithelium?
Outermost cells are dead, non-nucleated, filled with keratin; resists friction and is impermeable to water
What is transitional epithelium (urothelium)?
Several layers of cells with dome/umbrella-shaped superficial cells; located in the urinary system; superficial cells can flatten and stretch when the bladder fills
What is the axoneme and how is it arranged?
The core microtubule complex of a cilium; arranged as 9 doublets surrounding 2 central singlets (“9 + 2” pattern)
What is the function of microvilli and what is their cytoskeletal core?
Increase surface area for absorption; core of 25–30 actin filaments cross-linked by villin, embedded in the terminal web
What are the three functional types of junctional complexes?
- Occluding junctions – impermeable barriers
- Anchoring junctions – structural integrity
- Communicating junctions – passage of signaling molecules
What are the key molecular components of tight junctions (zonulae occludentes)?
- Claudins (primary proteins, Ca²⁺-dependent)
- Occludins, Nectins, JAMs
- ZO-1, ZO-2, ZO-3 (link claudins to cytoskeleton)
What proteins occupy the intercellular space of zonulae adherentes?
Cadherins (Ca²⁺-dependent transmembrane linker proteins); intracytoplasmic aspect binds actin via vinculin, catenin, and α-actinin
What proteins occupy the intercellular space of desmosomes?
Desmocollins and desmogleins (both cadherins, Ca²⁺-dependent)
What connects desmoplakins to intermediate filaments in desmosomes?
Plakoglobins and plakophilins held together by desmoplakins, which contact keratin intermediate filaments
What is pemphigus vulgaris and what causes it?
A skin disease caused by autoantibodies against desmosomal proteins; treated with systemic steroids and immunosuppressive agents
What is Naxos Syndrome?
A condition caused by mutations in desmoplakins and plakoglobins, presenting with keratoderma of palms/feet and right ventricular arrhythmia (cardiomyopathy)
What causes Generalized Junctional Epidermolysis Bullosa (JEB)?
Mutations in LAMA3, LAMB3, or LAMC2 genes → skin/mucosal blisters within the lamina lucida of the basement membrane upon minor trauma
What are connexons and how do they form gap junctions?
Six connexin proteins assemble into a connexon (aqueous pore); two connexons from adjacent cells align and fuse to form a gap junction channel
What regulates the opening/closing of gap junctions?
- Decreased pH or increased Ca²⁺ → closes channels
- High pH or low Ca²⁺ → opens channels
What are the five layers of the epidermis (inner to outer)?
- Stratum basale (germinativum)
- Stratum spinosum
- Stratum granulosum
- Stratum lucidum
- Stratum corneum
What are the four cell types of the epidermis?
- Keratinocytes (largest population)
- Langerhans cells (antigen-presenting, bone marrow–derived)
- Merkel cells (mechanoreceptors, neurocrine secretion)
- Melanocytes (neural crest–derived, produce melanin)
How long does epidermal turnover take?
Approximately 20–30 days (epidermis ~28 days; intestinal lining every 4–6 days)
What is metaplasia? Give a clinical example.
Transformation of one epithelial type into another; e.g., pseudostratified ciliated epithelium → stratified squamous epithelium in heavy smokers (squamous metaplasia)
What is the epigenetic significance of DNMT1 in the epidermis?
DNMT1 levels are highest in undifferentiated basal progenitor cells and decrease with differentiation; DNA methylation generally decreases during differentiation
Anki cloze
The basement membrane consists of the {1:basal lamina} produced by epithelial cells and the {1:lamina reticularis} produced by fibroblasts.
Anki cloze
Tight junctions prevent membrane proteins from migrating between the {1:apical} and {1:basolateral} domains, thereby maintaining cell polarity.
Anki cloze
The axoneme of a cilium follows a {1:9 + 2} microtubule arrangement: nine doublets surrounding two central singlets.
Anki cloze
Desmosomes use {1:desmocollins} and {1:desmogleins} in the intercellular space and anchor to {1:keratin} intermediate filaments via desmoplakins.
Anki cloze
Gap junctions are closed by {1:decreased pH} or {1:increased cytosolic Ca²⁺} and opened by high pH or low Ca²⁺.
Anki cloze
In pemphigus vulgaris, {1:autoantibodies against desmosomal proteins} disrupt cell adhesion, causing skin blistering.
Anki cloze
Transitional epithelium is distinguished by {1:dome/umbrella-shaped} superficial cells that flatten when the {1:bladder} is distended.
Anki cloze
Stratified squamous keratinized epithelium is found in tissues exposed to friction such as the {1:palm of the hand}, where the outermost cells are {1:dead and filled with keratin}.
Anki cloze
Type I hemidesmosome is found in {1:stratified squamous} and {1:pseudostratified} epithelia; type II is found in {1:simple columnar} epithelial cells.
Anki cloze
JEB is caused by mutations in {1:LAMA3}, {1:LAMB3}, or {1:LAMC2} genes, leading to blisters within the {1:lamina lucida}.