TARGET DECK: MED::I::Signaling Pathways in Health and Disease::Metabolic Biochemistry::04 - Overview of Carbohydrate Metabolism
Topics Covered
- Digestion and absorption
- General scheme: role of liver and extra-hepatic tissues
- Glycogen synthesis and breakdown
- Glycolysis
- Pyruvate oxidation
- Tricarboxylic Acid (TCA) Cycle
- Gluconeogenesis
- Pentose phosphate shunt
Key Dietary Carbohydrates
| Molecule | SMILES |
|---|---|
| Glucose | OC[C@H]1OC(O)[C@H](O)[C@@H](O)[C@@H]1O |
| Fructose | OC[C@@H]1OC(O)(CO)[C@@H](O)[C@@H]1O |
| Glycogen | Branched polymer of α-D-glucose (α-1,4 and α-1,6 linkages) |
| Starch | Linear (amylose) and branched (amylopectin) α-D-glucose polymer |
franz
aggiungi come smiles o metti foto delle slide…
Digestion and Intestinal Absorption
Major dietary carbohydrates and their products:
| Carbohydrate | Type | Products |
|---|---|---|
| Starch | Polysaccharide | Glucose |
| Lactose | Disaccharide | Galactose + Glucose |
| Sucrose | Disaccharide | Fructose + Glucose |
- Digestion: Amylases from saliva and pancreas
- Absorption: Through intestinal microvilli via secondary active transport
Glucose Absorption
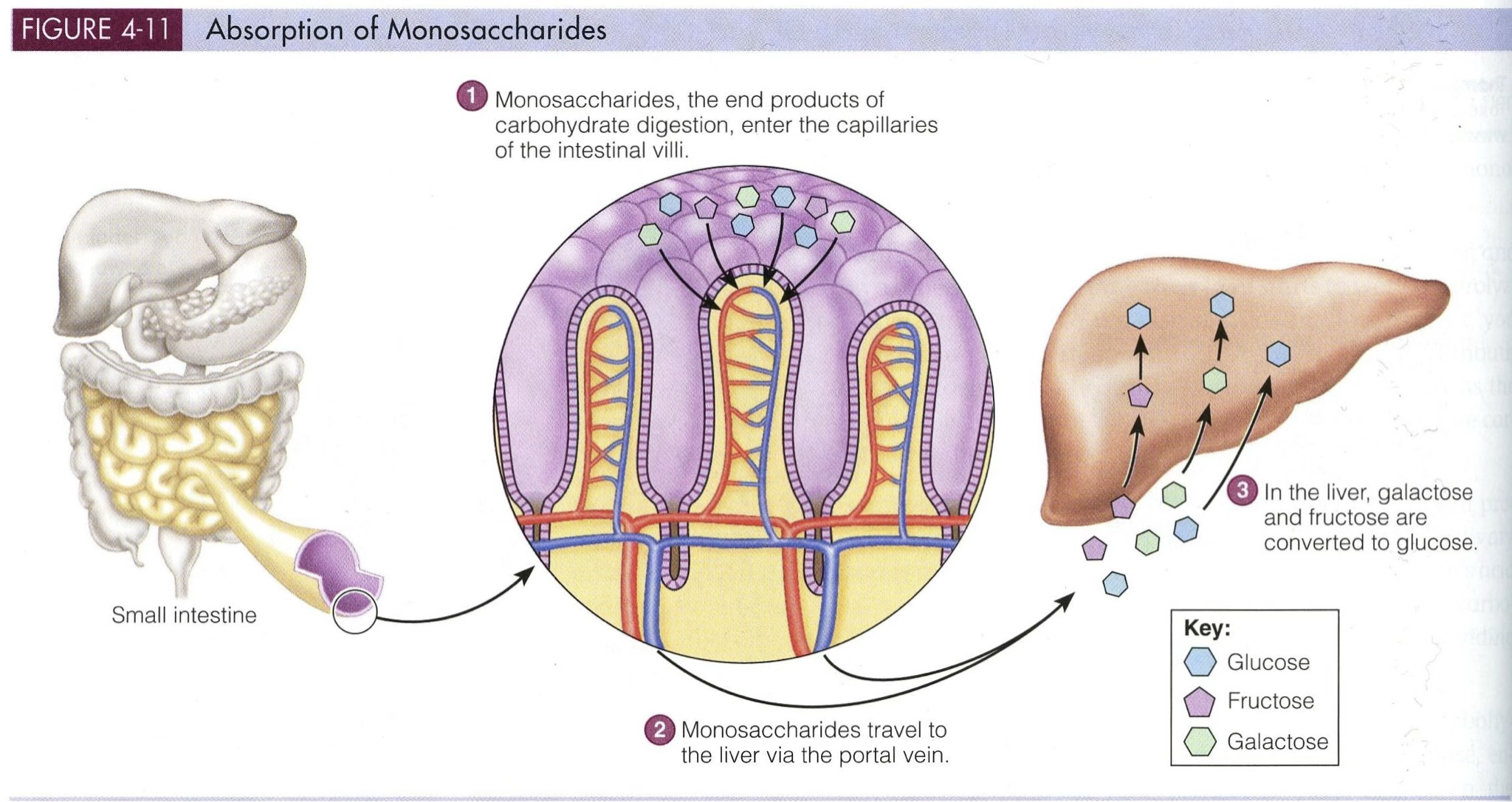
Energetics of Intestinal Co-transport
Transport Steps
- Secondary active transport → Glucose + 2 Na⁺ enter the enterocyte (SGLT1)
- Primary active transport → Na⁺/K⁺-ATPase maintains the Na⁺ gradient
- Passive transport → Glucose exits via GLUT2 into portal blood
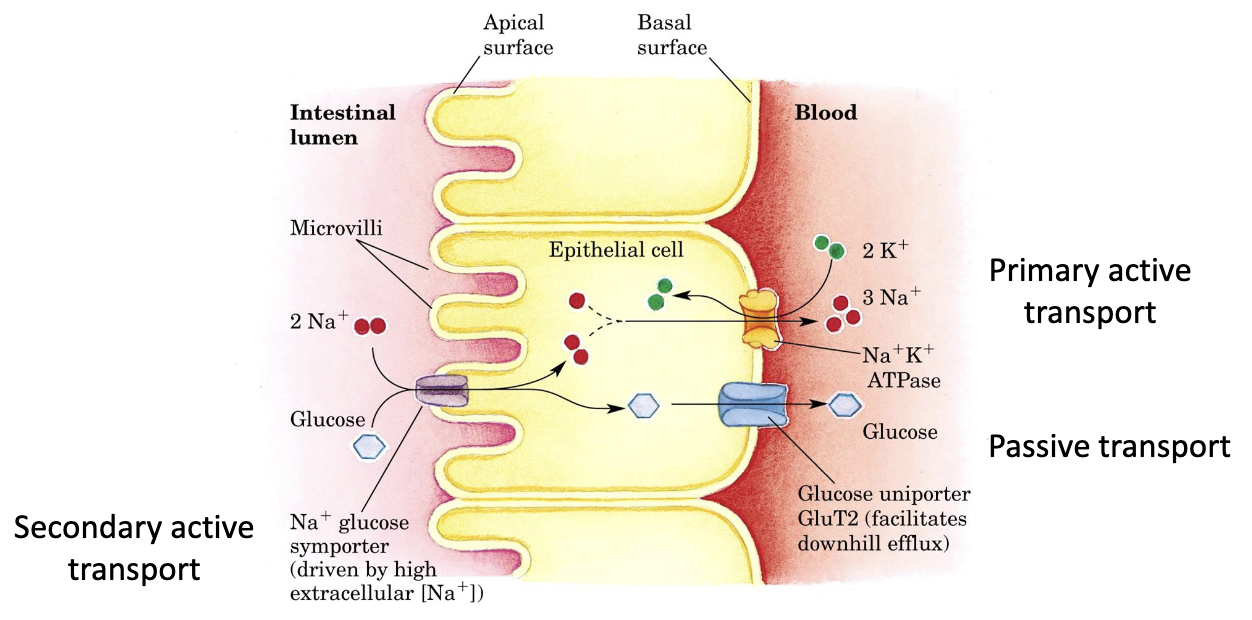
How is glucose absorbed from the intestine?
Glucose enters enterocytes by secondary active transport with Na⁺ via SGLT1, then exits to portal blood via GLUT2.
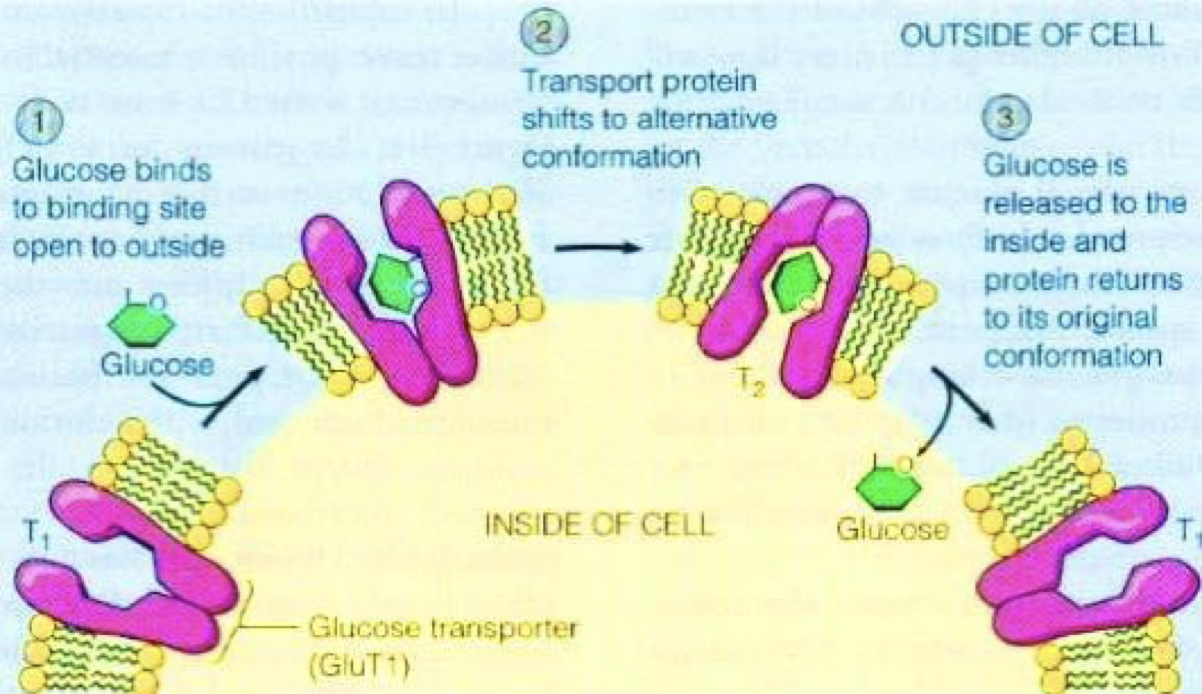
Glucose Transport in Blood (GLUT Transporters)
| GLUT | Location | Features | (substrate) mM |
|---|---|---|---|
| GLUT1 | Ubiquitous (RBCs, brain) | High affinity, basal uptake | 5 (glucose) |
| GLUT2 | Liver, pancreatic β-cells, intestine | Low affinity, high capacity | 10-15 (glucose, [galactose & fructose]) |
| GLUT3 | Neurons | Very high affinity | 1-2 (glucose) |
| GLUT4 | Muscle, adipose tissue | Insulin-dependent | 3-5 (glucose) |
| GLUT5 | 6 (fructose) | ||
 |
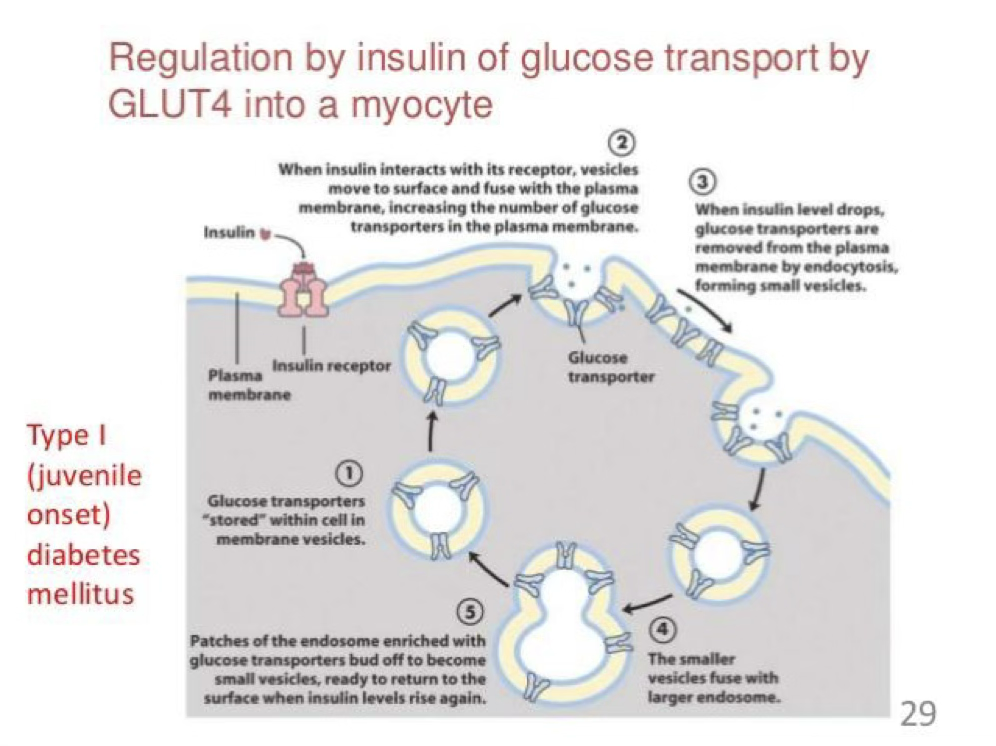
GLUT4
GLUT 4 can be regulated by insulin.
Which GLUT transporter is insulin-dependent?
GLUT4 in muscle and adipose tissue.
- Storage (The “Waiting Room”)
Normally, GLUT4 transporters aren’t on the cell’s surface. They are tucked away inside the cell in small bubbles called vesicles. They are basically “off-duty” and waiting for a signal.
- The Insulin Signal (The “Green Light”)
When you eat, your pancreas releases insulin.
- Binding: Insulin binds to an insulin receptor on the cell membrane (the pink structure in your image).
- Translocation: This sends a signal that tells the GLUT4 vesicles to move toward the surface and fuse with the plasma membrane.
- Action: Now that the “doors” are open on the surface, glucose can flood into the cell to be used for energy.
- Removal (The “Closing Time”)
Once your blood sugar levels drop, insulin levels also decrease.
- Endocytosis: The cell pinches the membrane back inward, swallowing the GLUT4 transporters.
- Recycling: These transporters are pulled back into the cell, forming new vesicles (Steps 4 and 5) where they stay until the next meal.
Anatomical Route of Absorbed Glucose
- Intestinal microvilli
- Portal circulation blood
- Hepatic sinusoids → glucose enters hepatocytes postprandially
- Centrolobular vein
- General circulation
Glycaemic Regulation
A glycaemic peak follows a carbohydrate-rich meal. Regulation is primarily mediated by insulin (↑ uptake) and glucagon (↑ production).
General Scheme of Carbohydrate Metabolism
- Metabolic tasks are distributed between the liver and peripheral tissues (muscle, brain, etc.) via the bloodstream
- The kidney plays a key role through ultrafiltration and reabsorption of glucose, governed by the renal threshold
Glucose Reabsorption in the Kidney
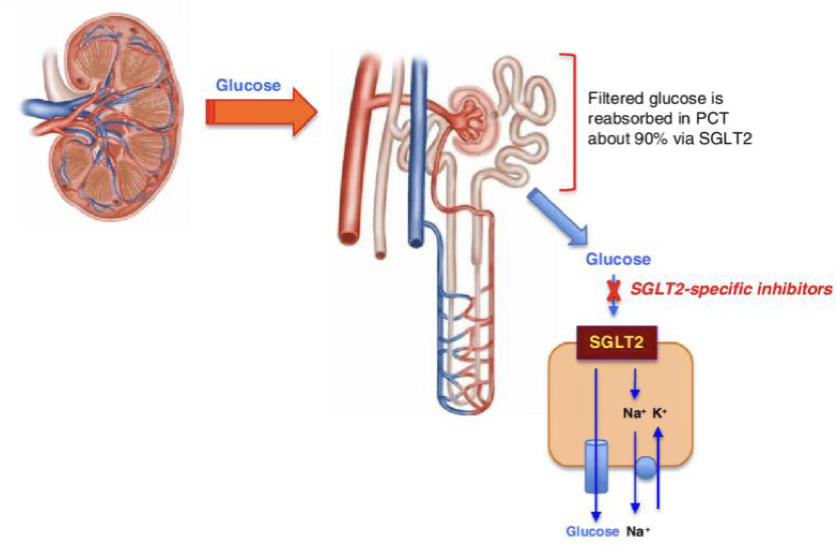
Sites and Transporters
| Segment | Transporter | Affinity | Capacity | % Glucose Reabsorbed |
|---|---|---|---|---|
| Early PCT | SGLT2 | Low | High | ~90% |
| Late PCT | SGLT1 | High | Low | ~10% |
- Basolateral exit into the bloodstream: via GLUT2 and GLUT1
- Driving force: Na⁺/K⁺-ATPase maintains the electrochemical gradient required for SGLT activity
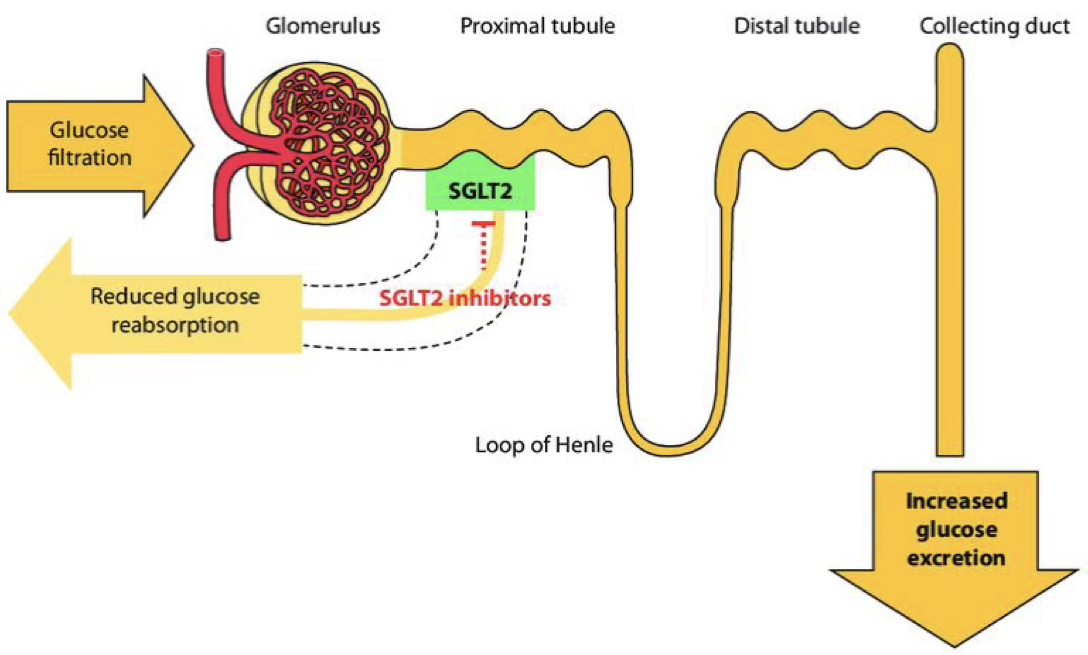
Renal Threshold for Glucose (RTG)
Renal Glucose Threshold
In healthy individuals, the RTG is approximately 180–200 mg/dL. Below this concentration, virtually all filtered glucose is reabsorbed. Above it, glucose appears in the urine (glucosuria).
What is the renal threshold for glucose in healthy individuals?
About 180–200 mg/dL; above this, glucose appears in urine.
Transport Maximum (Tm) for glucose reabsorption:
RTG variability:
| Condition | RTG |
|---|---|
| Healthy adult | 180–200 mg/dL |
| Pregnancy / Children | < 126 mg/dL |
| Type 2 Diabetes | 200–250 mg/dL |
Effects of Insulin and Glucagon
Summary Table
| Hormone | Pathways Activated | Net Effect |
|---|---|---|
| Insulin | Glycogen synthesis, Glycolysis, Pentose phosphate pathway, Lipid synthesis | ↓ Blood glucose |
| Glucagon | Glycogenolysis, Gluconeogenesis | ↑ Blood glucose |
What is the main metabolic effect of insulin versus glucagon?
Insulin promotes glycogen synthesis, glycolysis, PPP, and lipid synthesis; glucagon promotes glycogenolysis and gluconeogenesis.
Postprandial State (Insulin Active)
Glucose → Glucose-6-P → Glycogen (liver & muscle)
→ Glycolysis → Pyruvate → CO₂ + H₂O (+ ATP)
→ Lipid synthesis
Fasting State (Glucagon Active – Liver)
Glycogen → Glycogenolysis → Glucose-6-P → Glucose (→ blood)
Amino acids → Gluconeogenesis → Glucose-6-P → Glucose (→ blood)
Skeletal Muscle (No Glucagon Receptors)
Blood Glucose → (Insulin ↑) → Glucose-6-P
→ Glycogen
→ 2 Pyruvate → CO₂ + H₂O (25 ATP)
→ Lactate (→ blood)
Net: 2 ATP (substrate level) + 25 ATP (oxidative) per glucose
Kinases and Phosphatases
Kinase = phosphotransferase:
Note
In protein kinases, X is a Ser, Thr, or Tyr residue. Many kinase reactions are irreversible; the reverse is catalysed by a phosphatase:
Glucose Phosphorylation
Key Reactions
Futile Cycle
Running both reactions simultaneously results in:
This is energetically wasteful and is largely prevented by hormonal regulation.
Why is the glucose/glucose-6-phosphatase pair considered a futile cycle?
Because running both reactions at once wastes ATP without changing the glucose pool.
Hormonal Transcriptional Control
| Enzyme | Induced by | Inhibited by | Effect on Glycaemia |
|---|---|---|---|
| Glucokinase | Insulin | Glucagon | ↓ |
| Glucose-6-Phosphatase | Glucagon | Insulin | ↑ |
Hexokinase vs. Glucokinase
| Property | Glucokinase (GK) | Hexokinase (HK) |
|---|---|---|
| Location | Liver, pancreatic β-cells | All other tissues |
| Affinity | Low (high Km) | High (low Km) |
| Substrate specificity | Glucose only | Glucose, fructose, mannose |
| Product inhibition | Not inhibited by G6P | Inhibited by G6P |
| Insulin induction | Yes | No |
| Kinetics | Sigmoidal (cooperative) | Hyperbolic (Michaelis-Menten) |
Glucokinase Regulatory Protein (GKRP)
GKRP Regulation
- Fasting: GKRP sequesters GCK in the nucleus, creating a reserve pool
- Postprandial (high glucose): GCK is released into the cytoplasm → phosphorylates glucose → supports glycogen synthesis
- F6P stabilises the GCK–GKRP complex → enhanced inhibition
- F1P disrupts the complex → releases active GCK into the cytosol
Downstream Fates of Glucose-6-Phosphate
(All stimulated by insulin, inhibited by glucagon)
Glucose-6-P ──→ Glycogen synthesis
──→ Glycolysis
──→ Pentose phosphate pathway
TLDR - 04 - Overview of Carbohydrate Metabolism
TLDR – Overview of Carbohydrate Metabolism
Digestion & Absorption:
Dietary carbohydrates (starch, lactose, sucrose) are broken down by salivary and pancreatic amylases into monosaccharides (glucose, fructose, galactose). These are absorbed in the intestine via secondary active transport (SGLT1, driven by the Na⁺ gradient maintained by Na⁺/K⁺-ATPase) and exit into the portal blood via GLUT2.Glucose Transport:
GLUT transporters mediate tissue-specific glucose uptake. GLUT4 in muscle and adipose tissue is insulin-dependent. GLUT2 in the liver acts as a glucose sensor (low affinity, high capacity).Renal Handling:
The kidney reabsorbs ~90% of filtered glucose via SGLT2 (early PCT) and ~10% via SGLT1 (late PCT). The renal threshold is ~180–200 mg/dL; above this, glucosuria occurs. Tm is 375 mg/min (men) and 300 mg/min (women).Insulin vs. Glucagon:
- Insulin (postprandial): activates glycogen synthesis, glycolysis, pentose phosphate pathway, and lipid synthesis → lowers blood glucose
- Glucagon (fasting): activates glycogenolysis and gluconeogenesis → raises blood glucose
- Skeletal muscle has no glucagon receptors; glucose metabolism there is primarily insulin-driven
Glucose Phosphorylation:
Glucose is trapped in cells as Glucose-6-Phosphate by hexokinase (all tissues, high affinity, inhibited by G6P) or glucokinase (liver/pancreas, low affinity, not inhibited by G6P, insulin-induced). G6P can be released back to glucose only in liver and kidney (glucose-6-phosphatase). Running both enzymes simultaneously creates a futile cycle, prevented hormonally.GKRP sequesters glucokinase in the nucleus during fasting; high glucose and F1P release it into the cytosol, while F6P enhances its nuclear retention.
G6P fates (all insulin-stimulated, glucagon-inhibited): glycogen synthesis, glycolysis, pentose phosphate pathway.