General Principles
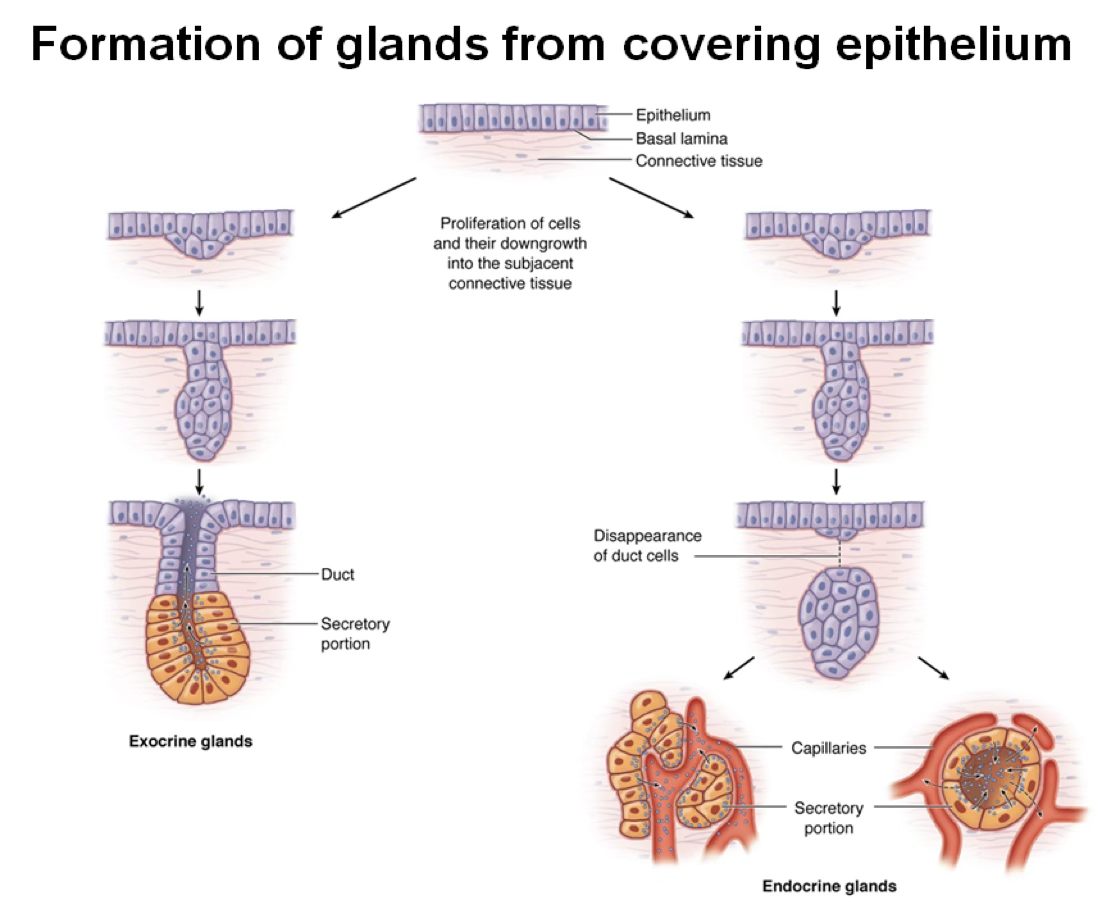
Endocrine glands release their secretions — hormones — directly into blood or lymphatic vessels for distribution to target organs. They are characterized by:
- No connection with the covering epithelium that generated them
- No ducts (ductless glands)
- High vascularization with fenestrated capillaries
Definition
The endocrine system consists of ductless glands, distinct clusters of cells within certain organs, and diffuse neuroendocrine cells.
It regulates metabolic activities to maintain homeostasis via chemical messengers (hormones) released into the bloodstream.
Secretory Organization
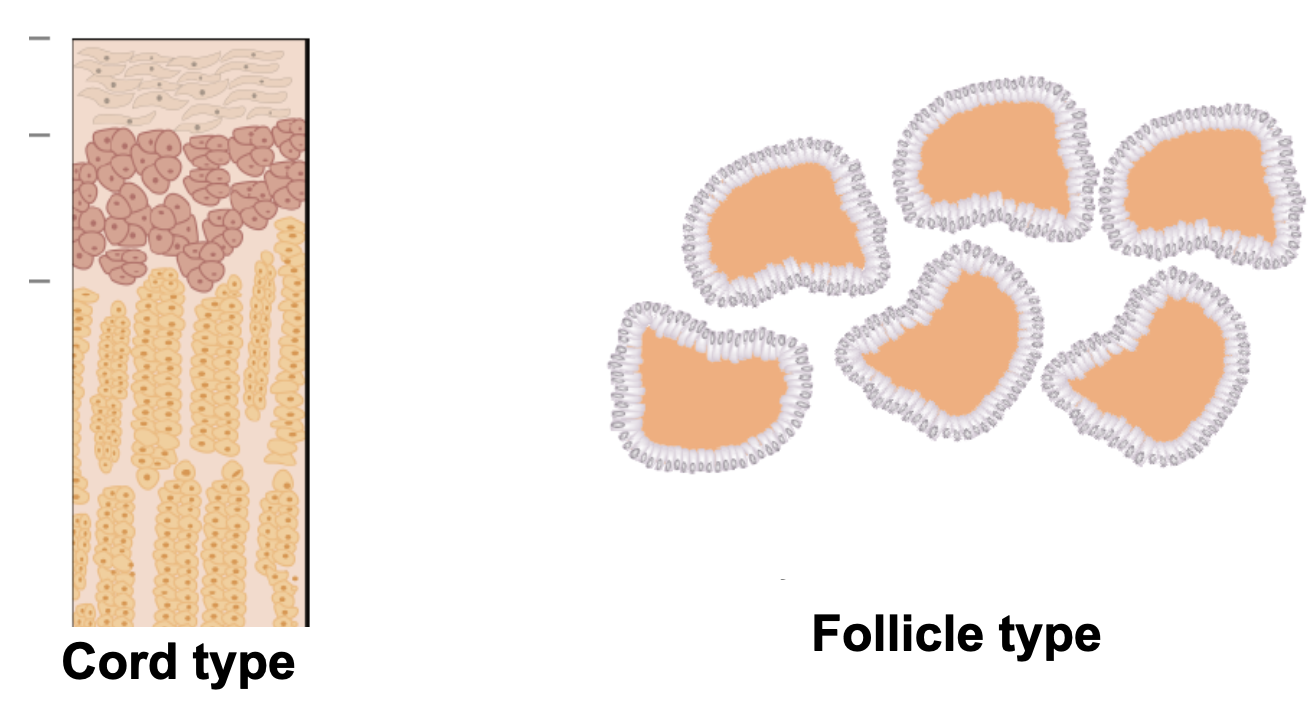
Secretory cells are arranged in one of two ways (classification of the parenchyma → the secreting portion):
Cord type (most common): cells form anastomosing cords around capillaries. Hormone is stored intracellularly and released upon signaling.
Follicle type: cells form follicles surrounding a central cavity (lumen) that stores secreted hormones (e.g., thyroid gland). Usually made by cuboidal/columnar.
Hormone Classification
Protein/Polypeptide Hormones (water-soluble)
Examples: thyroxine, epinephrine
- Cannot pass through the plasma membrane
- Bind receptors on the external cell surface
- Use a second messenger to trigger signal transduction (mediator of the signaling)
- Receptor couples with protein kinases → phosphorylation cascade → nuclear transcription factor activation
- Some exhibit intracrine activity (interact with intracellular receptors)
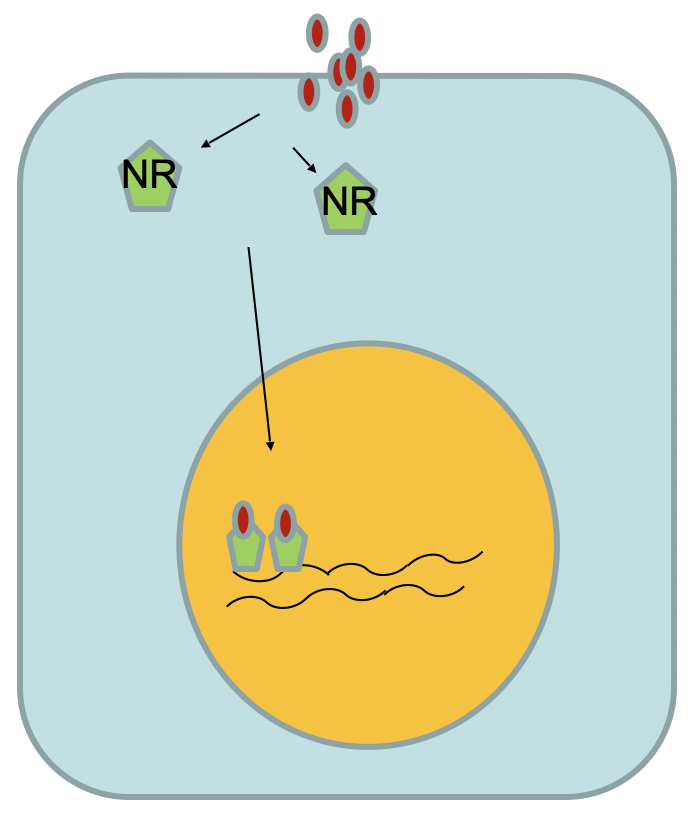
Steroid Hormones (lipid-soluble)
Examples: estrogen, progesterone, glucocorticoids
- Penetrate the cell membrane freely
- Bind cytoplasmic receptors
- Hormone–receptor complex (nuclear receptor) translocates to nucleus → stimulates gene transcription
Key Distinction
Steroids act via nuclear receptors (intracellular). Polypeptides act via membrane receptors + second messengers. This difference determines onset speed and duration of hormone action.
Feedback Mechanisms
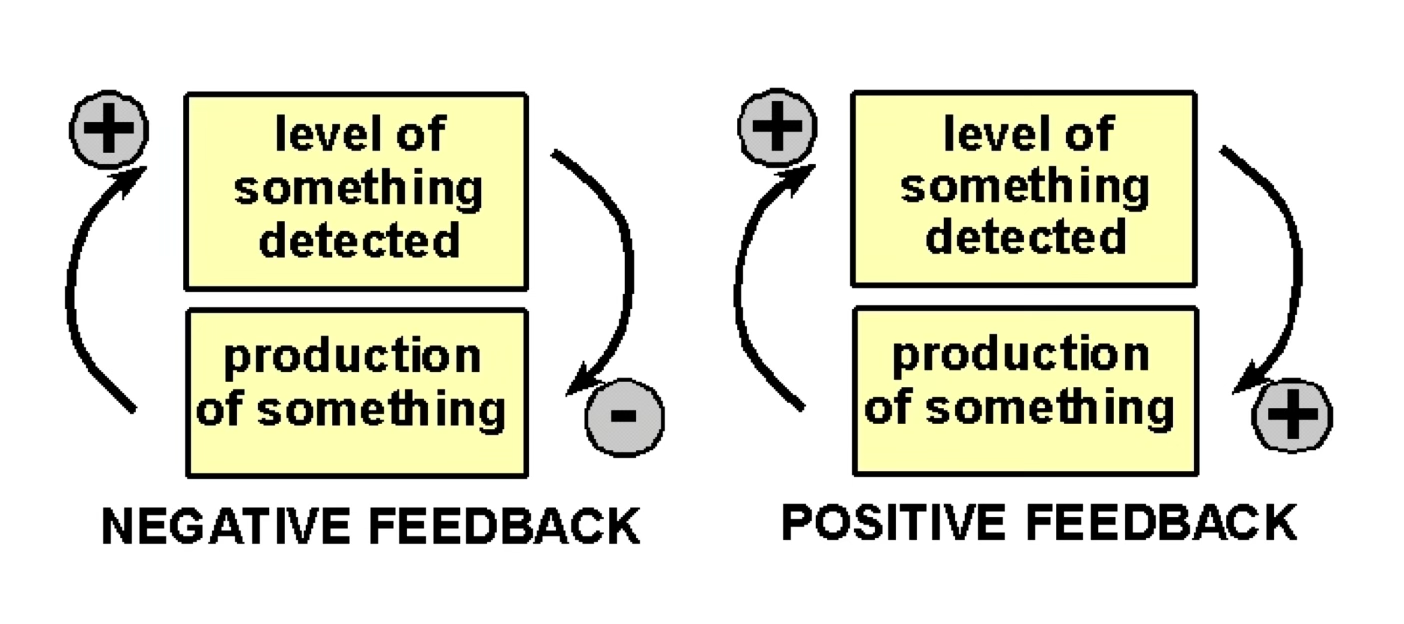
Most endocrine axes operate via negative feedback: the product of a target gland inhibits upstream hormone secretion (its own production), maintaining homeostasis.
Inversely, with positive feedback / feed-forward feedback, the absence/low level of the secrete induces upstream hormone secretion.
For example,
breath rate control during meditation → your body is mimicking “resting time” hormones when you manually lower your breath rate, leading to less anxiety.
Pituitary Gland (Hypophysis)
Master Gland
The pituitary is the master endocrine gland, secreting many types of hormones regulating growth, reproduction, and metabolism.
It weighs ~0.6 g and is 1cm (never-pregnant woman) and increases to ~1.2 cm after 2+ pregnancies.
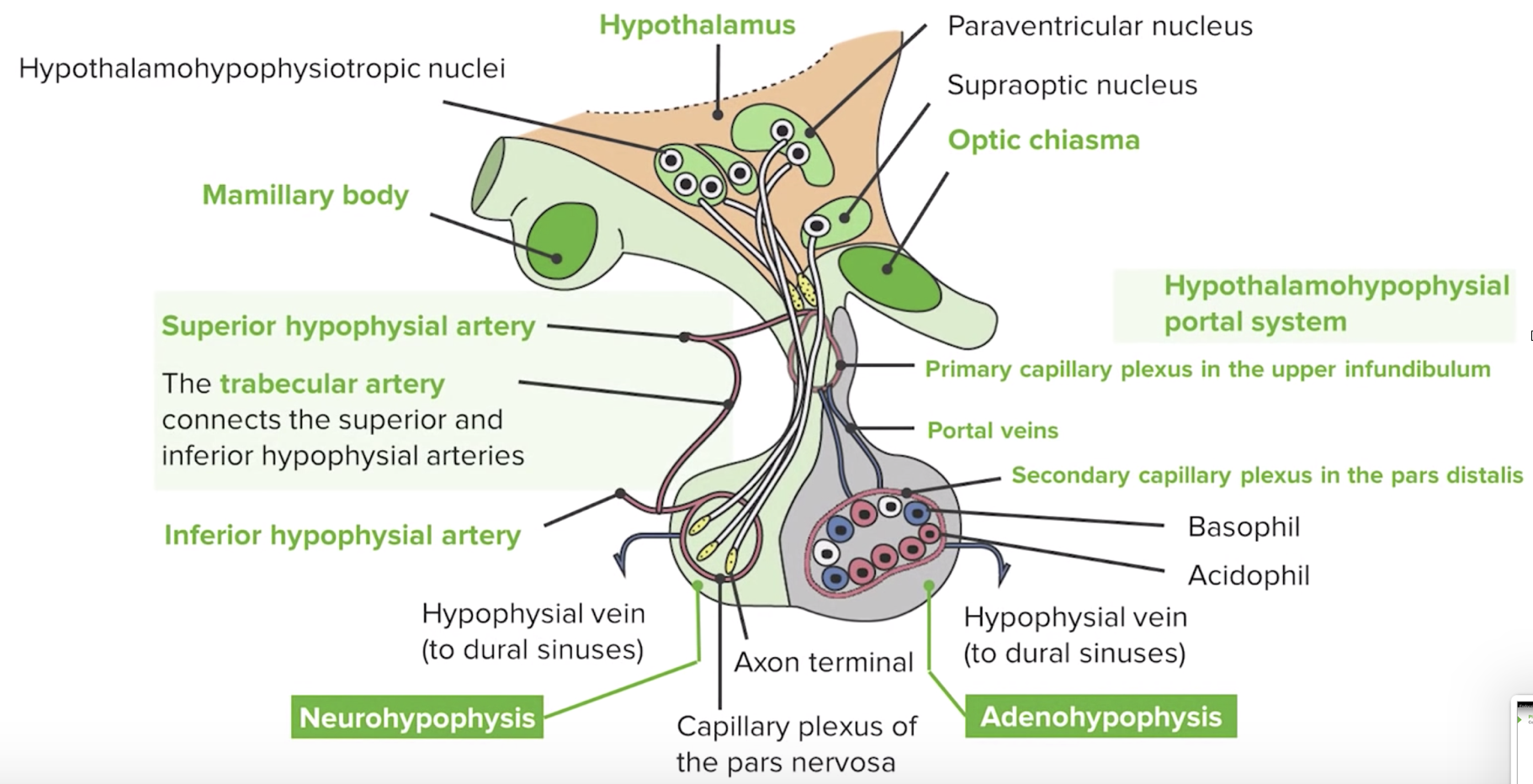
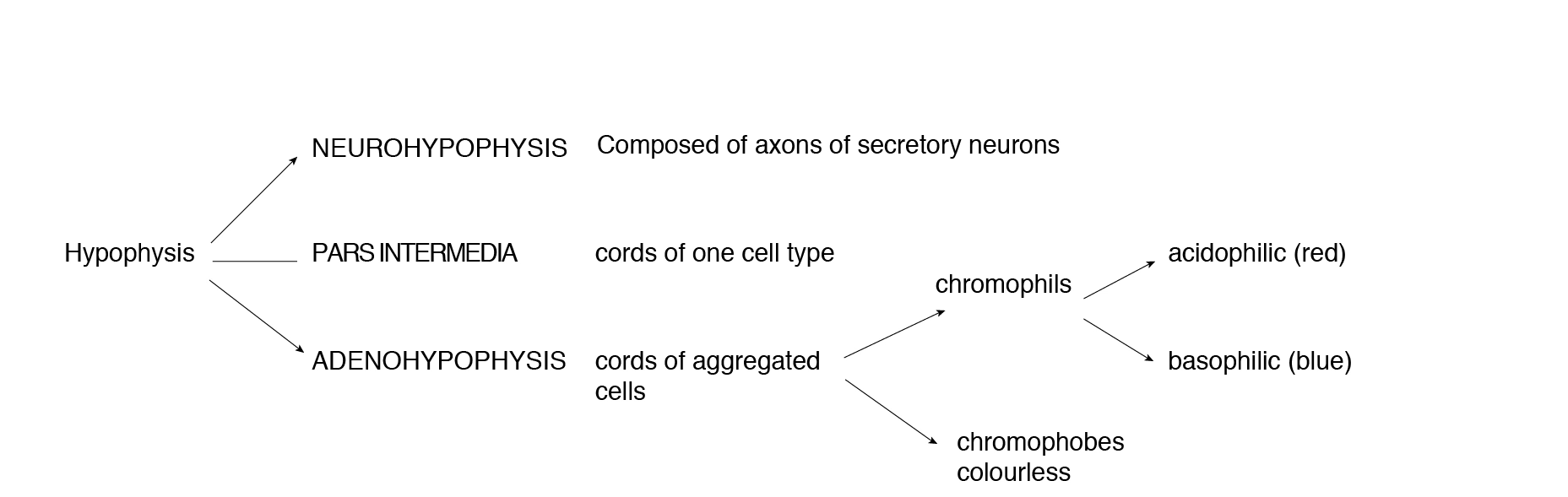
Divided into:
- Adenohypophysis (anterior pituitary) — derived from oral ectoderm (Rathke’s pouch); controlled by BMP4, FGF8, WNT5
- Neurohypophysis (posterior pituitary) — derived from neural ectoderm (completely different embryonic origin); contains pituicytes (glial cells) and Herring bodies
- Third area: intermediate hypophysis, composed of cords of only one cell type, not believed to be involved in hormone secretion.

The neurohypophysis is made by the axons of the secretory neurons, located at the level of the hypothalamus. They will release the hormones at the neurohypophysis.
There are no hormones produced in/by the neurohypophysis, they are only secreted there.
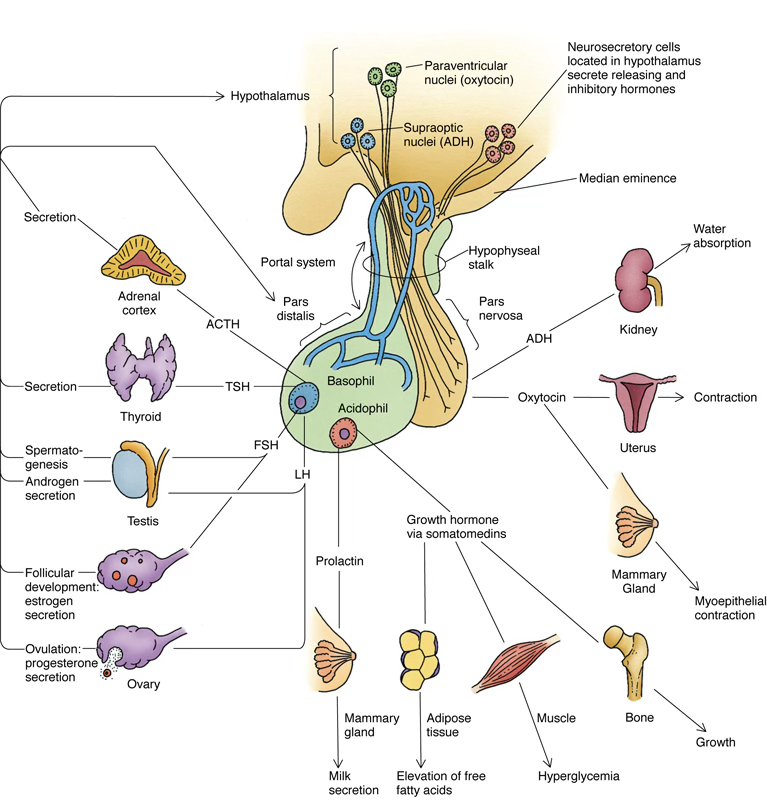
Hypothalamo-Pituitary Axis
The pituitary is under neural control of the hypothalamus.
Neurons with soma in the paraventricular and supraoptic nuclei project axons into the neurohypophysis, and release hypothalamic hormones into the capillary beds of the anterior pituitary.
Feed-Forward Signals from Hypothalamus
| Hypothalamic Hormone | Action | |
|---|---|---|
| TRH | Stimulates TSH release | Thyroid |
| CRH | Stimulates ACTH release | Corticotropin |
| SRH (GHRH) | Stimulates GH release | Somatotropin |
| GnRH | Stimulates LH and FSH | Gonadotropin |
| PRH | Stimulates prolactin | Prolactin |
| PIF (dopamine) | Inhibits prolactin | Prolactin |
Cells of the Adenohypophysis (Pars Distalis)
Three major cell types:
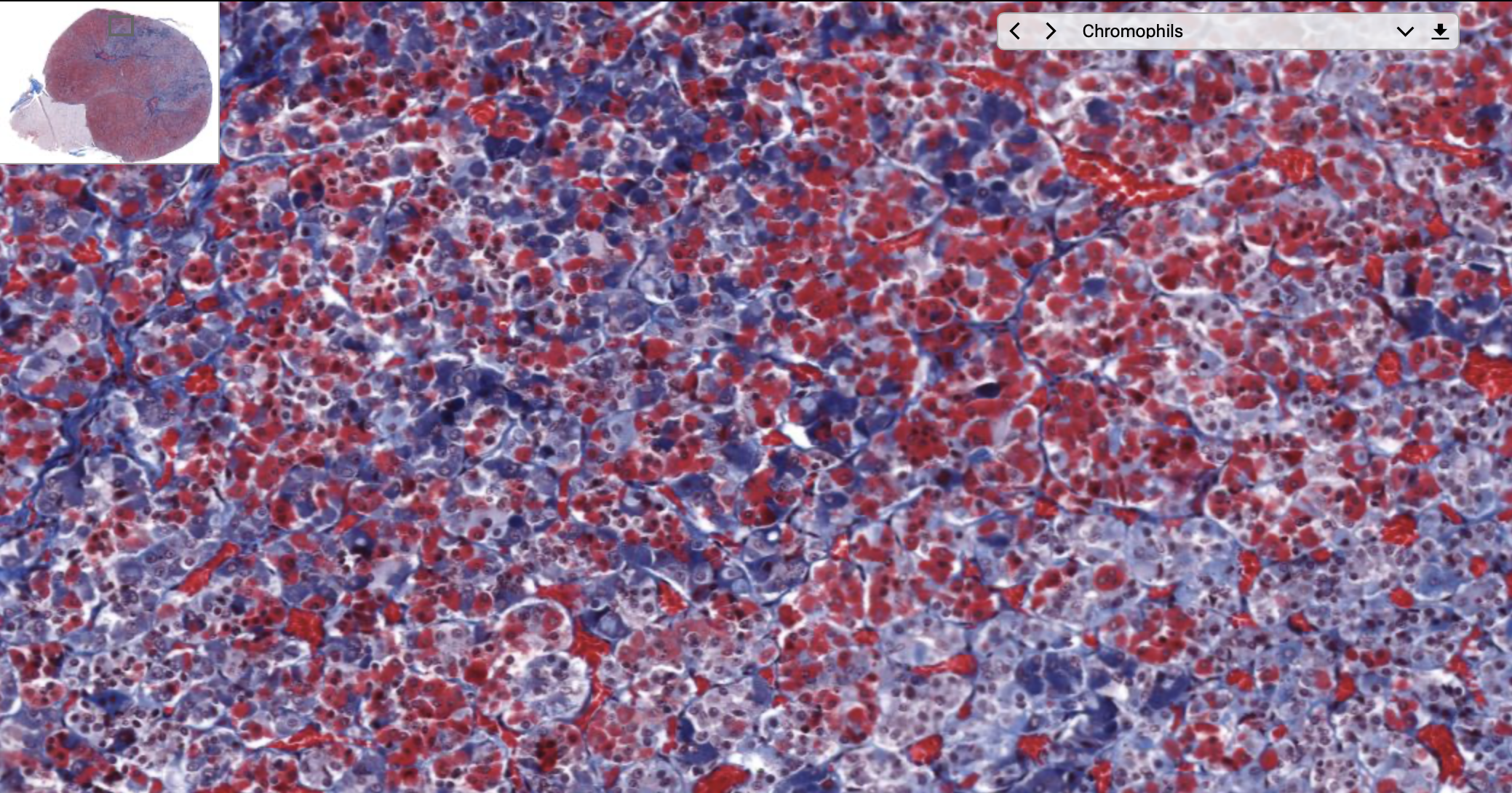
- (chromophils):
- acidophils,
- basophils,
- and chromophobes (probably lost their function / are in senescence, so they’re resistant to the staining).
Acidophils
Somatotrophs (~most abundant)
- Secrete somatotropin (GH / growth hormone)
- Stimulated by SRH; inhibited by somatostatin
- GH → liver produces IGF-I and IGF-II → stimulate epiphyseal plate chondrocyte mitosis → long bone elongation
Mammotrophs
- Release prolactin
- Promotes mammary gland development during pregnancy and lactation post-birth
Basophils
Basophil Location
Basophils stain blue with basic dyes and are typically located at the periphery of the pars distalis.
Corticotrophs (scattered, round–ovoid cells; eccentric nucleus; granules 250–400 nm)
- Secrete POMC (proopiomelanocortin) → cleaved to produce:
- ACTH → acts on adrenal cortex zona fasciculata → glucocorticoid release
- LPH (lipotropic hormone) → induces lipolysis, steroid synthesis, melanin production
- Further cleavage of ACTH → MSH → melanocytes → melanin
- Further cleavage of LPH → β-endorphin
Thyrotrophs (~5% of chromophils; anteromedial region; granules 150 nm)
- Secrete TSH (thyrotropin)
- Stimulated by TRH; inhibited by and
- TSH acts on thyroid follicular cells → releases and
Gonadotrophs (~10% of chromophils; distributed homogeneously; granules 300–400 nm)
- Secrete FSH and LH
- LH stimulates steroid production in testicular interstitial cells
- Stimulated by GnRH and leptin; inhibited by ovarian/testicular hormones
- Uncertain whether two subpopulations exist (one per hormone) or one cell produces both
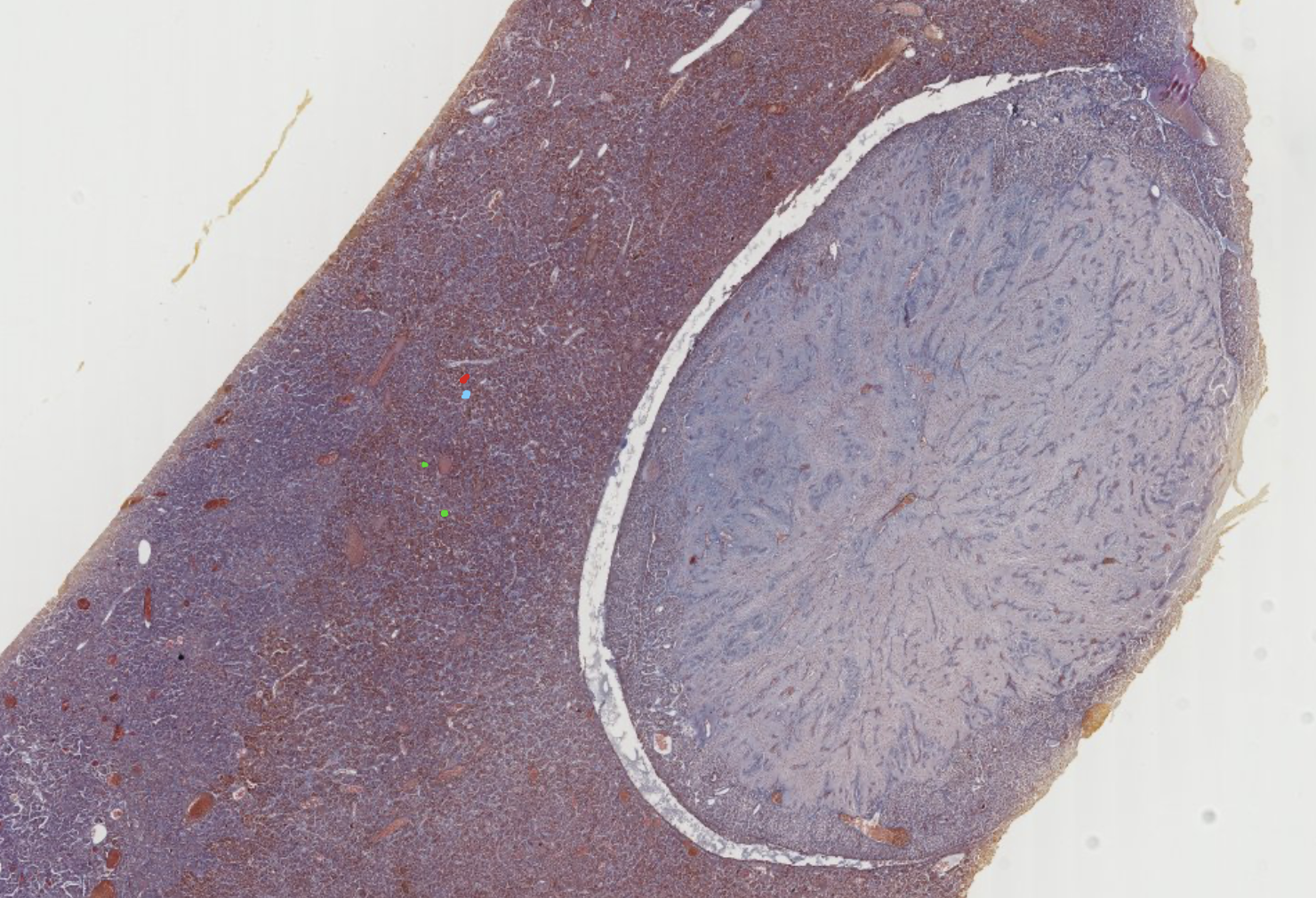
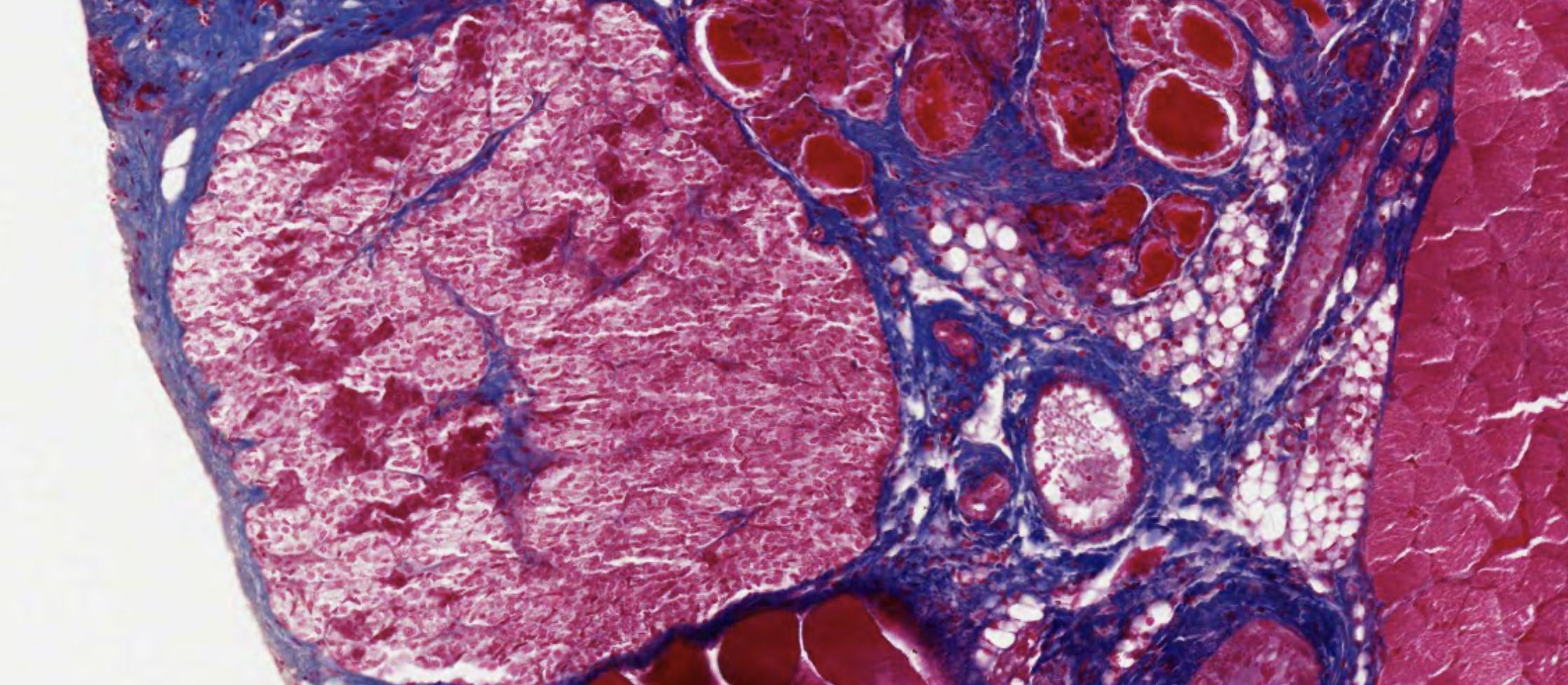
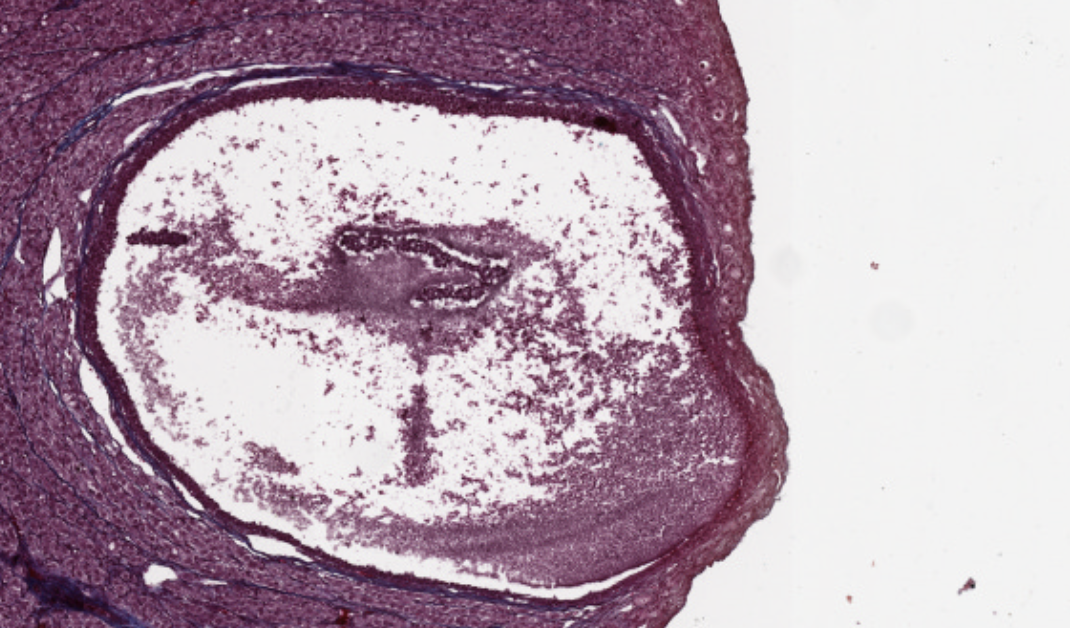
Start with the lowest power, to classify the gland.
The staining is always gonna have an important artifact: the two parts of the hypophysis will physically separate, and you will find a free space between the two. It’s the result of the detachment of the adenohypophsis from the neurohypophysis, due to their different nature of composition (epithelial vs neuronal).
The blue lines are reticular fibers, connective tissue keeping the glands together (?).
In this specimen, the colorphobes lack any staining, appearing transparent.
In the non secreting portion, you can see the neurofilaments of the axon bla bla. Several blood vessels huge amount of capillaries in both cut sections.
It might be harder here to find the Herring Bodies.
These vesicles no idea what they do, but they contribute to this separation.
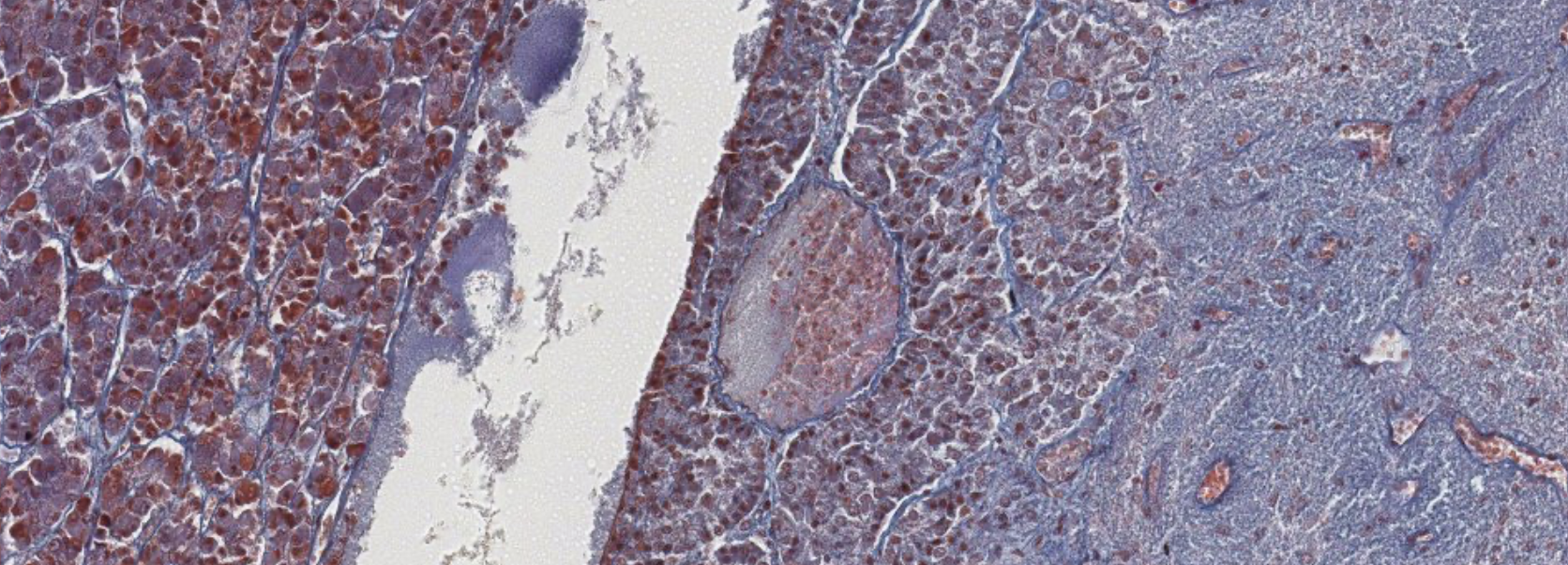
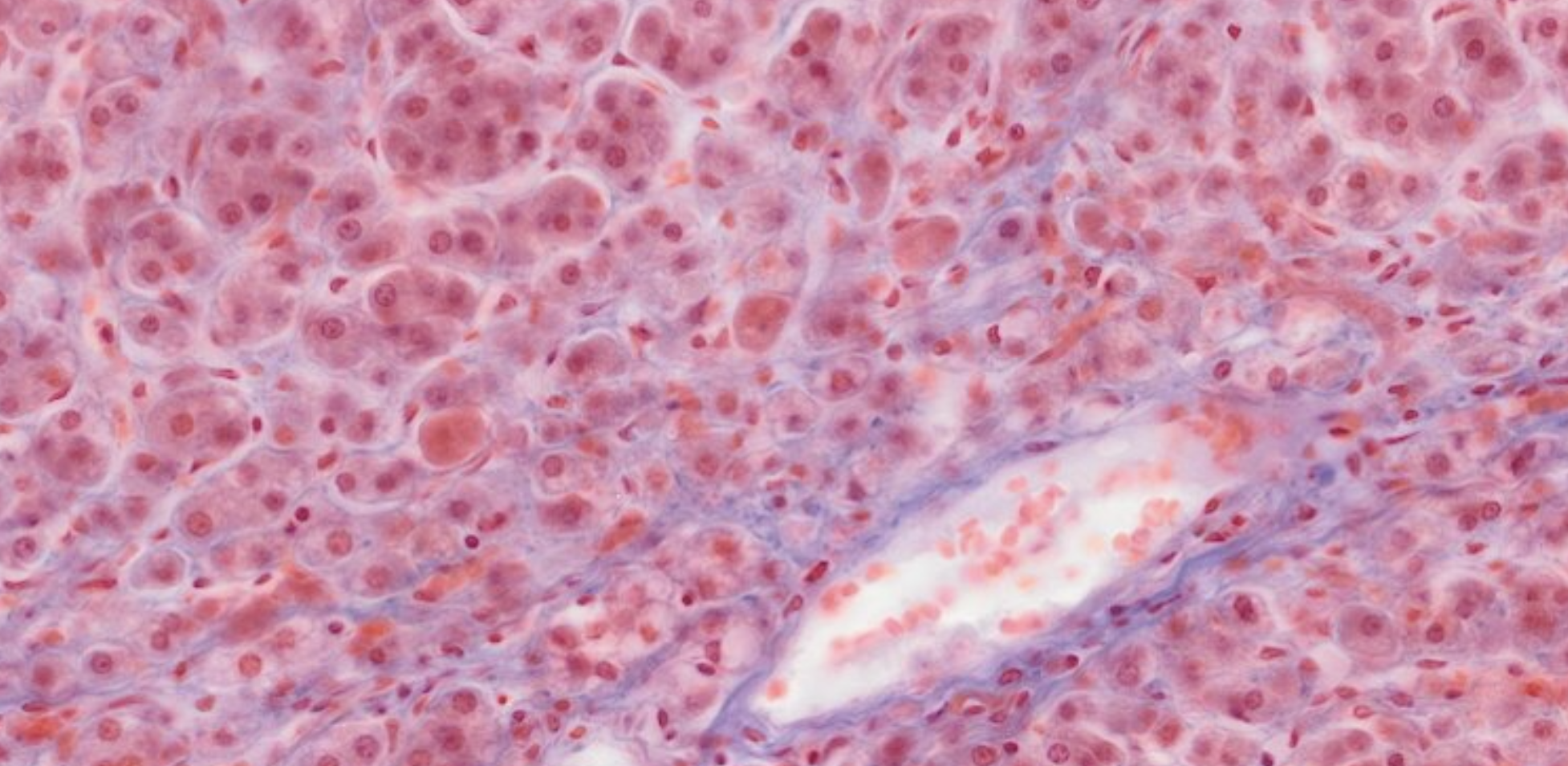
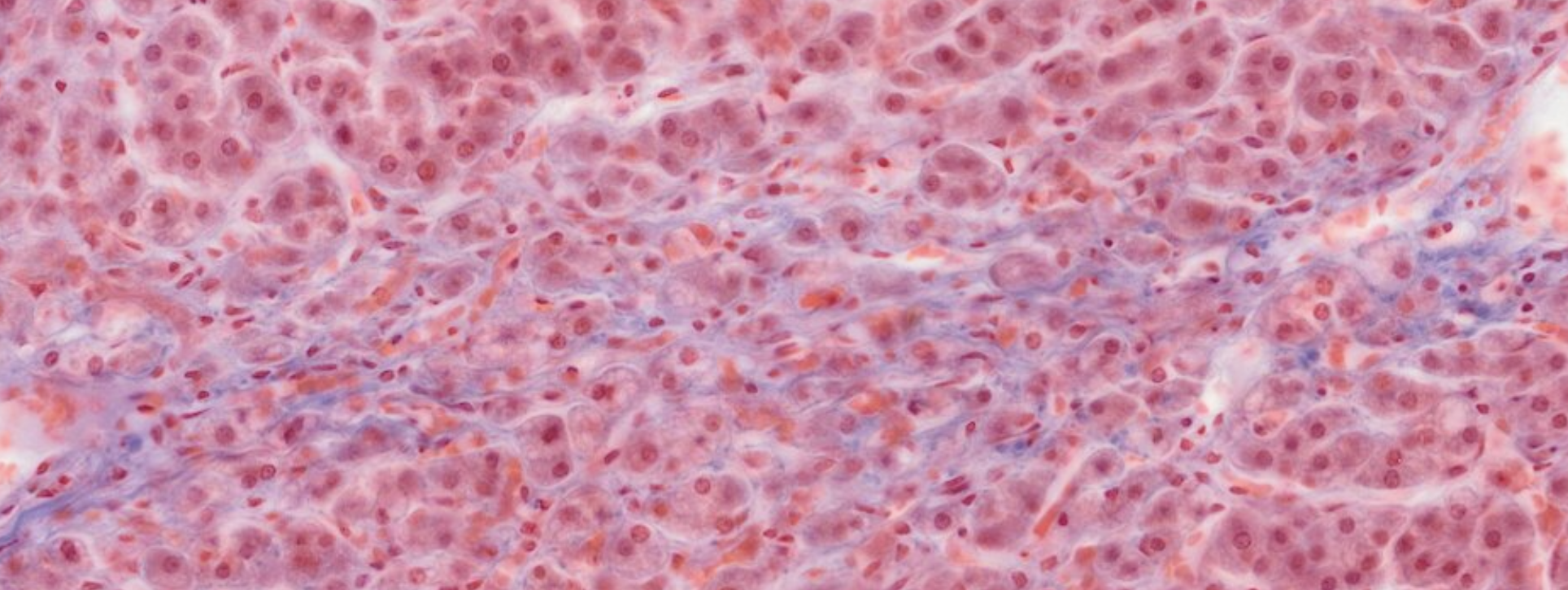
You can clearly see the cord structure of the endocrine glands, and the red/blue staining of the different types of cells.
We also see a large amount of blood vessels, usual for endocrine glands.
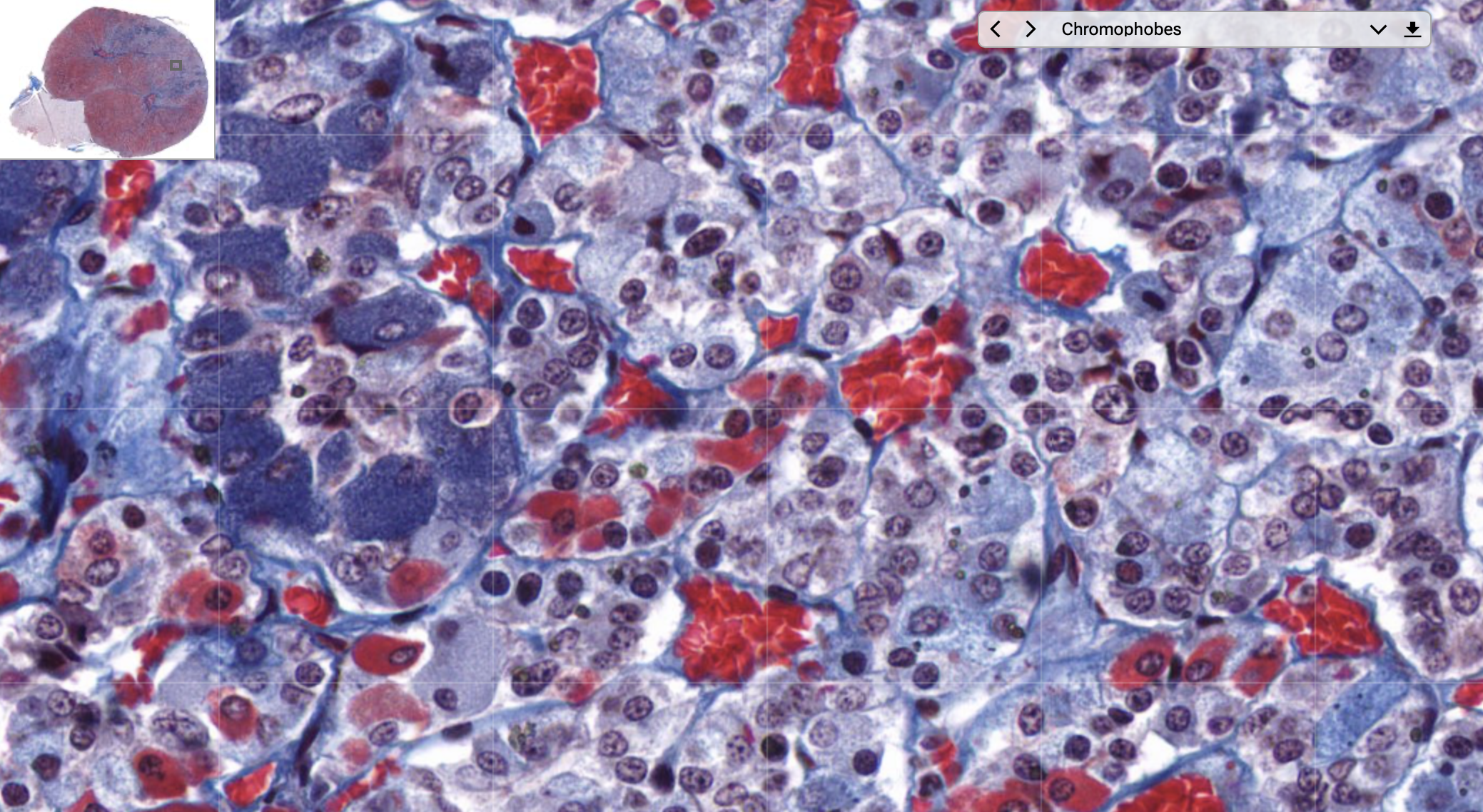
The chromophobes stain light blue.
Due to the good practice of the staining, we can also see the granules, inside the cells, representing the stored secrete.
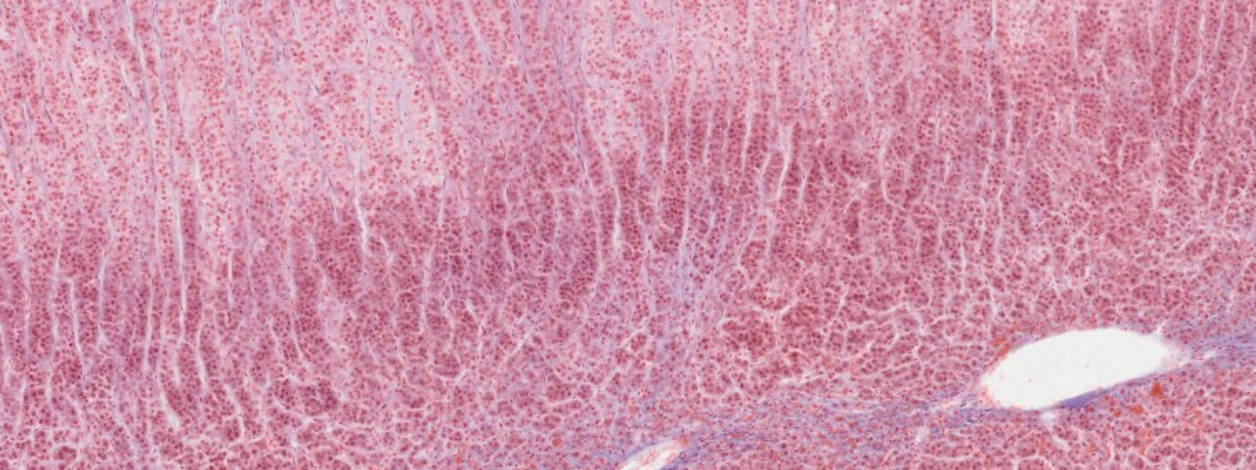
In the posterior of the cell there are very little cells, and the few nucleus that we see are part of glial cells. You can also identify small structures known as herring bodies, representing the ends of terminal axons filled with neurosecretion vescicles.
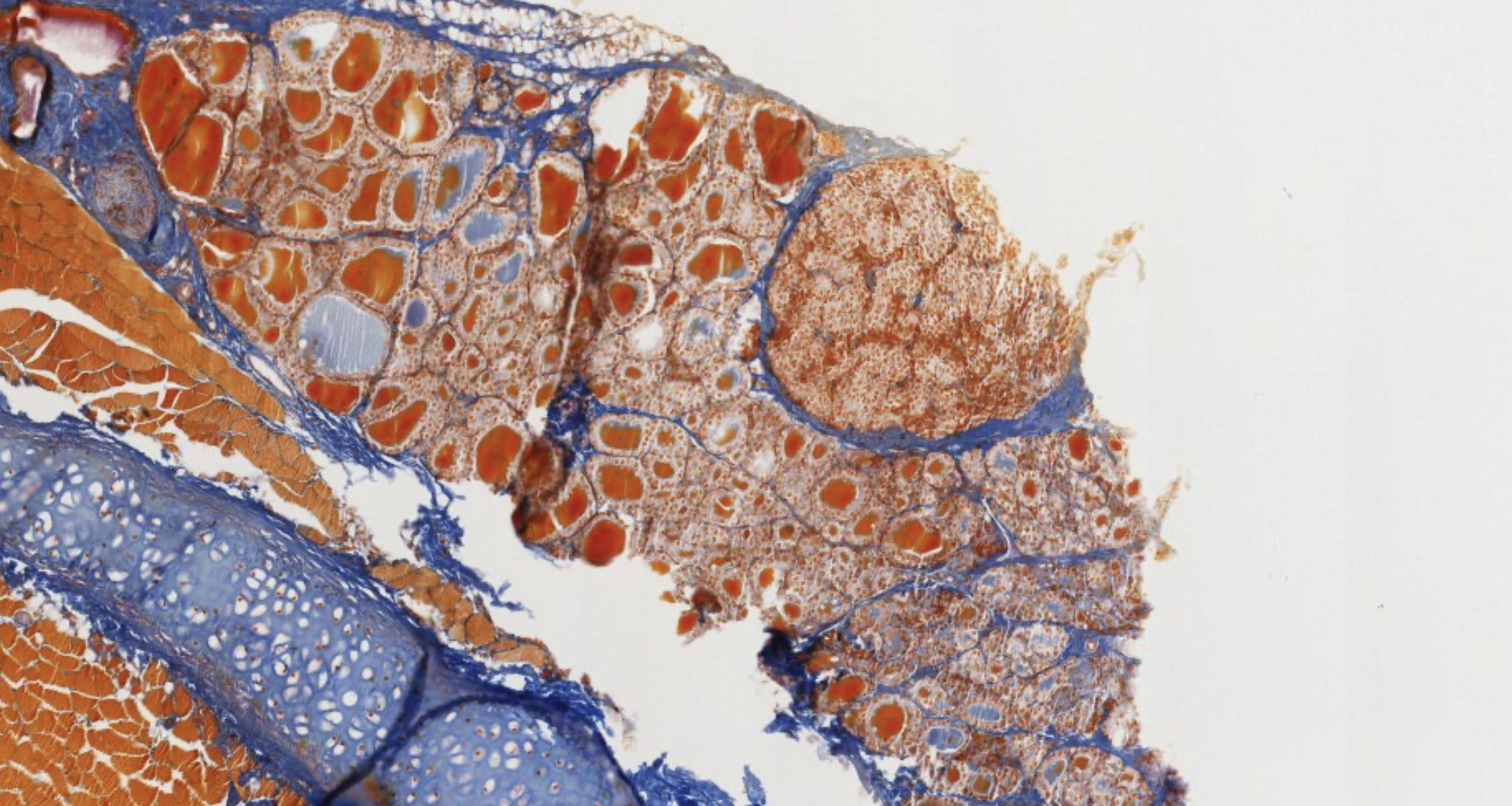
Thyroid Gland
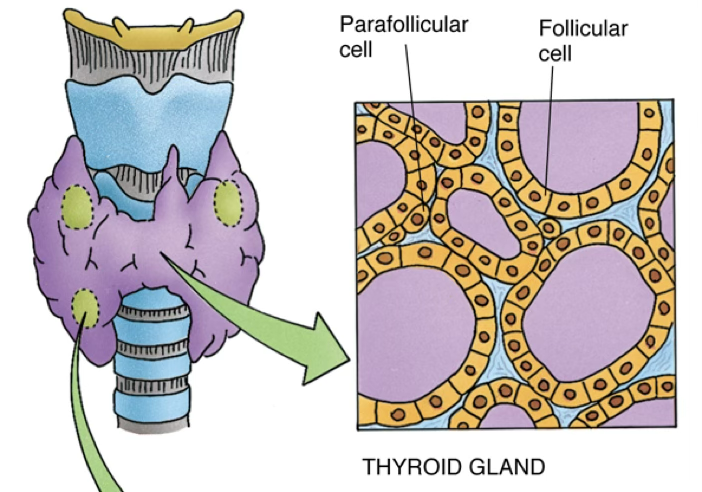
Composed of right and left lobes connected by an isthmus.
Surrounded by a collagenous (connective) capsule; parathyroid glands are embedded posteriorly.
Hormones Produced
- (triiodothyronine) — high affinity, 1-day half-life
- (thyroxine) — 90% of released hormone, 6-day half-life
- Calcitonin — produced by C-cells (parafollicular); decreases blood
and stimulate the rate of metabolism and are controlled by TSH from the adenohypophysis (basophil thyrotrophs).
TSH
The TSH attaches to the membrane receptors in the basal layer.
All the inactive and hormones reside and form the colloid, the lumen of these follicular cells.
and Activation
When the pituitary gland are stimulating the thyroid to secrete the T3 and T4, the follicular cells will re-uptake the hormone, activate it, and from them it will be sent to the bloodstream to reach the target organ.
(Explained in better detail later.)
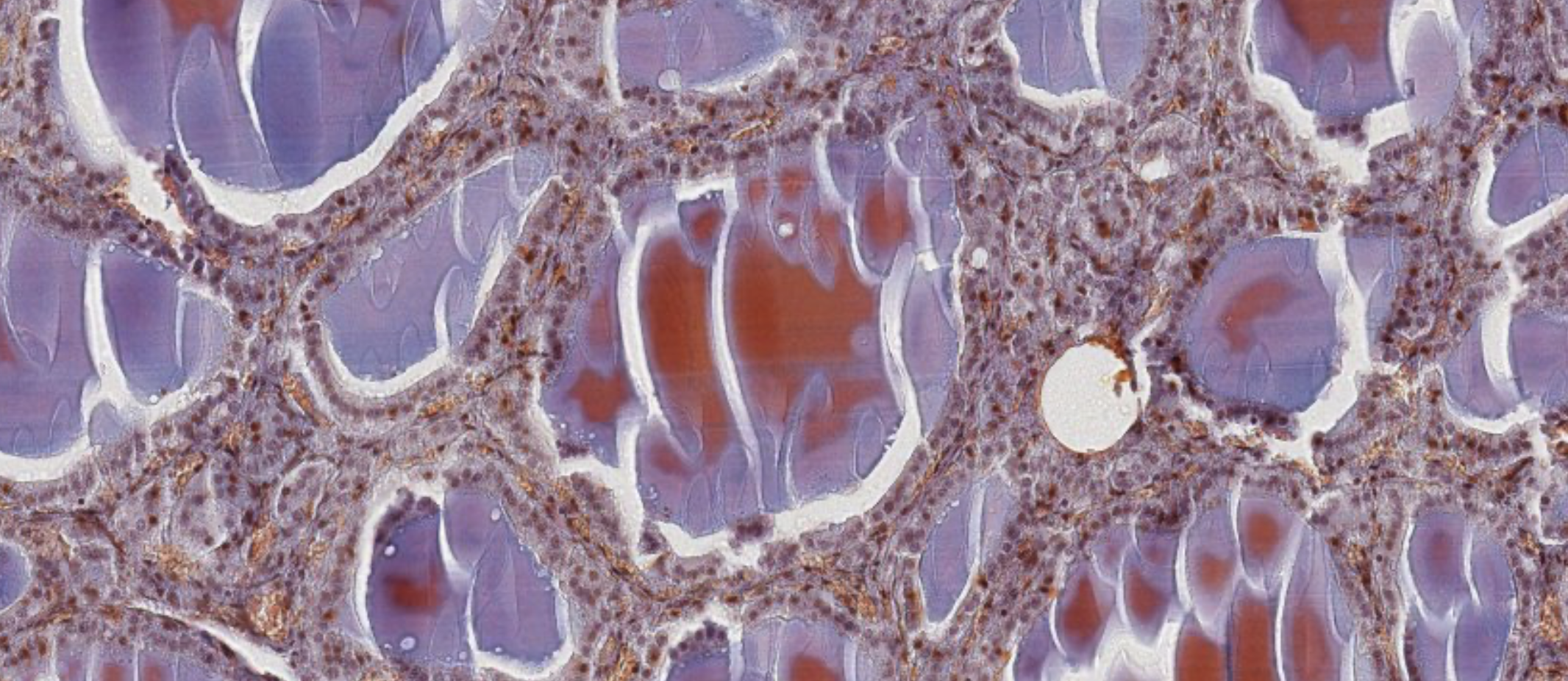
Active / Resting Thyroid.
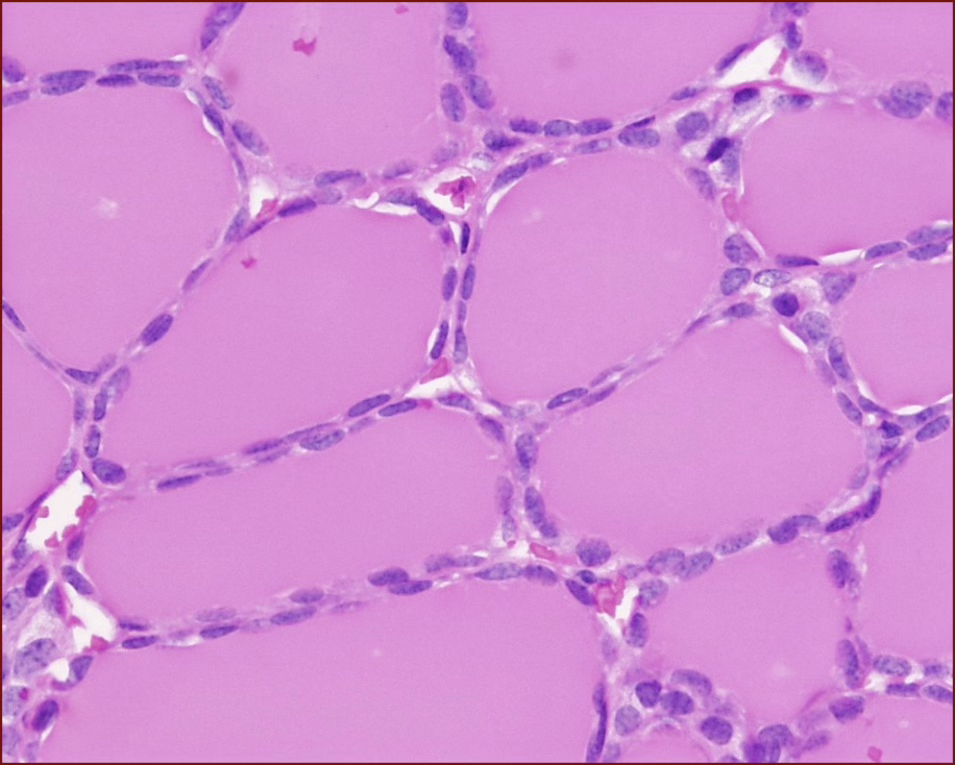
When we don’t have the presence of vesicles inside the colloid, that is a resting thyroid.
Resting Thyroid ↑
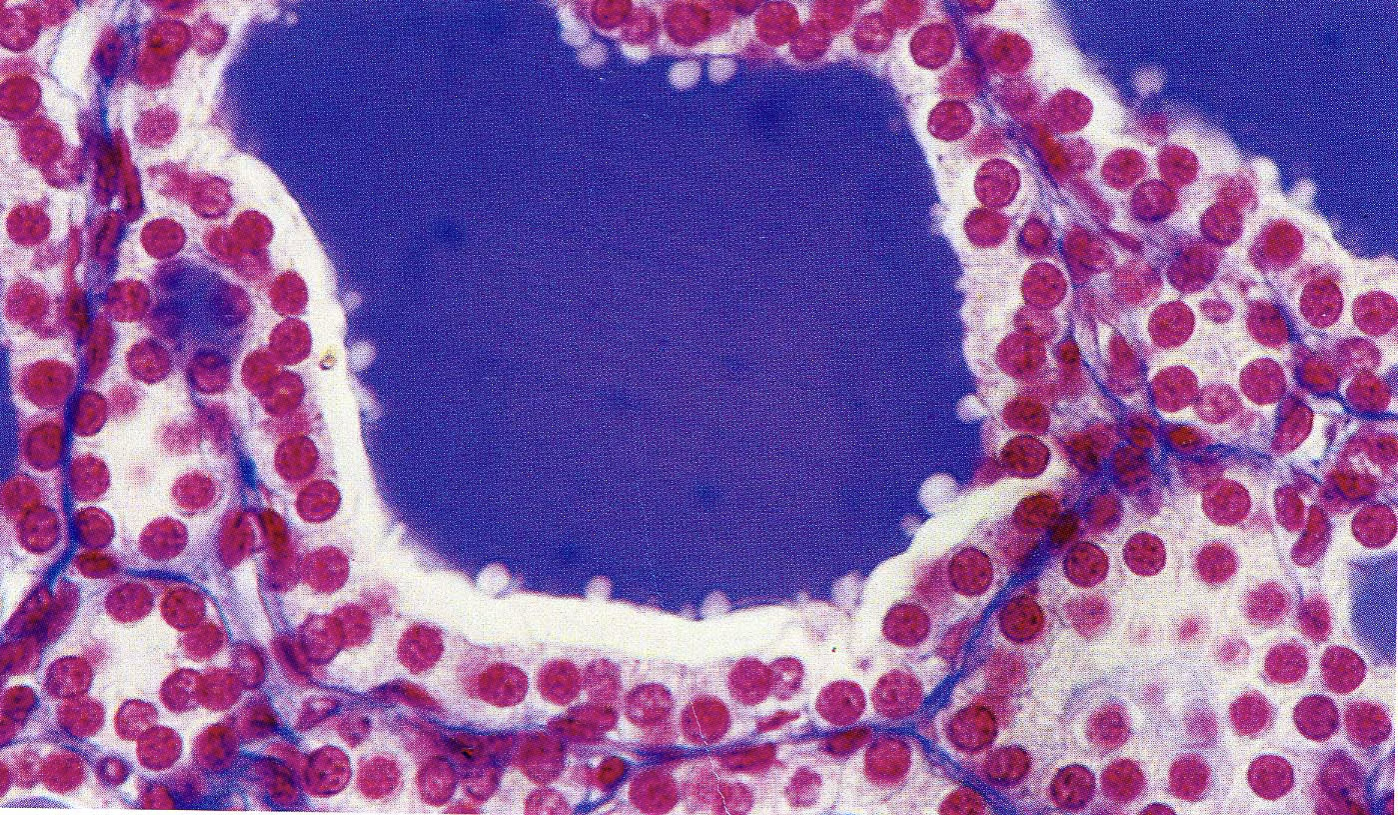
Activated Thyroid ↑
Vescicles inside the Lumen
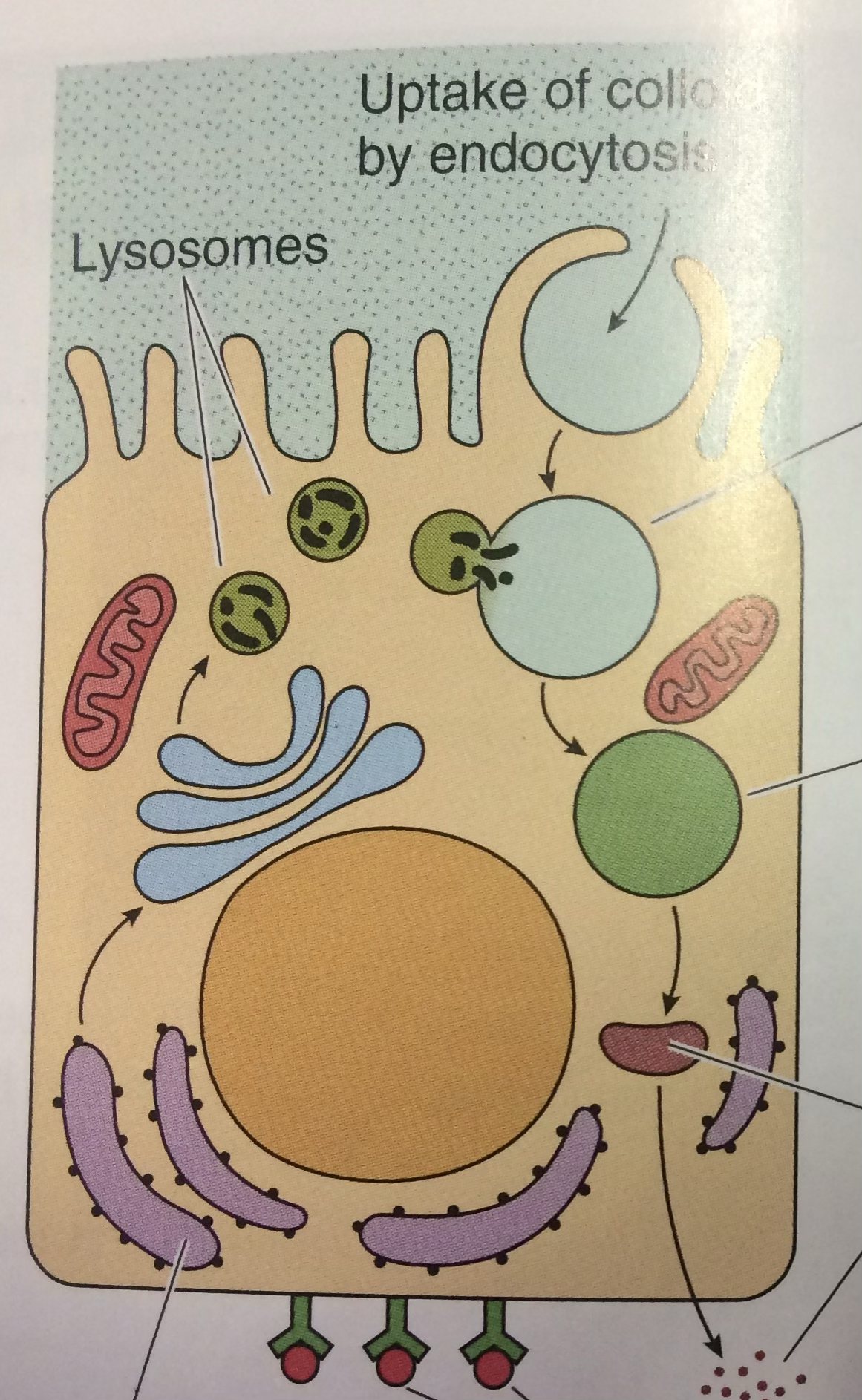
Vesicles are the proof that the follicular cells are performing endocytosis, re-uptaking the colloid for activation.
Cellular Organization
Follicles (0.2–0.9 mm diameter) composed of:
- Simple cuboidal epithelium (follicular cells + rare parafollicular cells)
- Central colloid-filled lumen — stores several weeks’ supply of hormone
and are bound to thyroglobulin (large secretory glycoprotein) within the colloid. Upon stimulation, hormone-bound thyroglobulin is endocytosed by follicular cells; hormones are cleaved by lysosomal proteases and released at the basal membrane into blood vessels.
Connective tissue septa from the capsule carry blood vessels, lymphatics, and nerves. Each follicle is surrounded by reticular fibers and a rich capillary plexus, separated by a thin basal lamina.
Iodide
Iodide () is essential for / synthesis. Iodination of tyrosine residues occurs at the colloid–follicular cell interface.
Follicular Cells (Principal Cells)
- Normally cuboidal with round nuclei and basophilic cytoplasm
- Apically located lysosomes; microvilli extending into colloid
- Upon TSH binding to membrane receptor: cells develop apical filopodia → endocytose colloid aliquots → / released basally into blood vessels
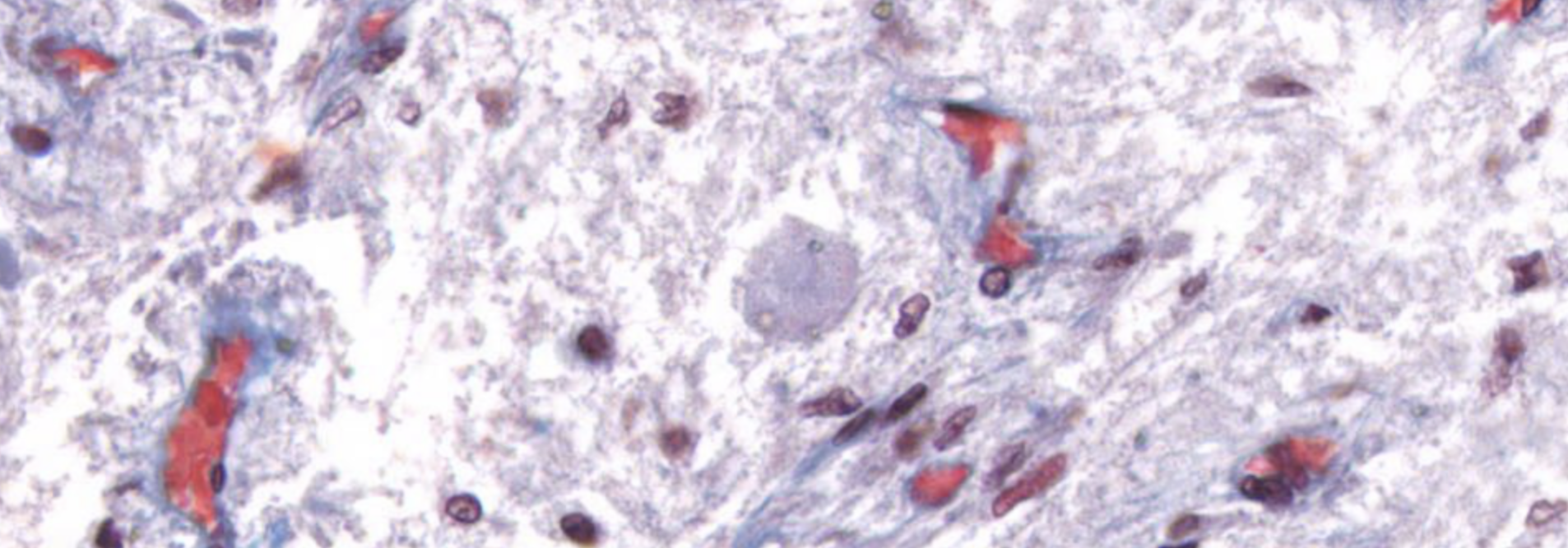
Parafollicular Cells (C-cells / Clear cells)
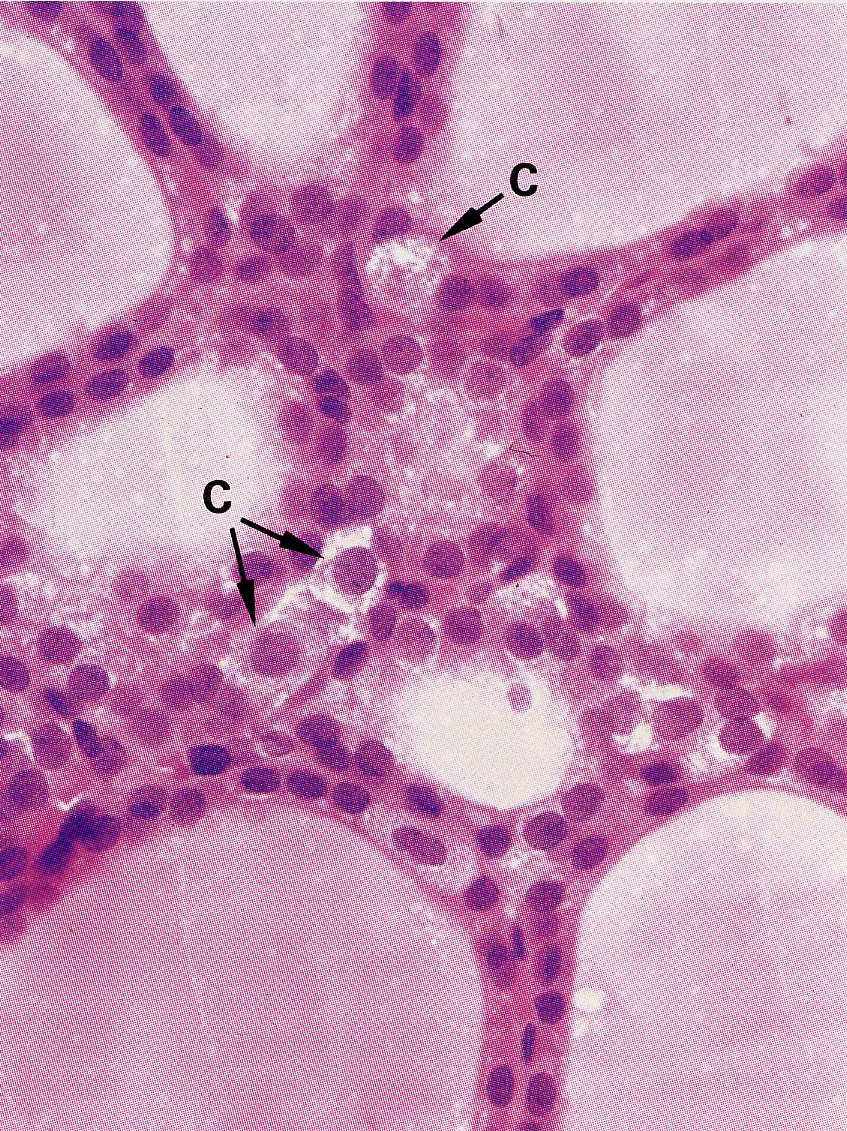
- 2–3× larger than follicular cells; only 0.1% of thyroid epithelium
- Produce calcitonin — peptide hormone that inhibits osteoclast bone resorption → lowers blood
Marker of an active thyroid.
Don’t be confused by the color of the colloid, but focus on the cuboidal shape of the follicular cells. The staining can be a weird reaction with the staining.The colloid needs to help you not mistake this gland with an exocrine alveolar gland.
Negative Feedback Control (Thyroid Axis)
Parathyroid Gland
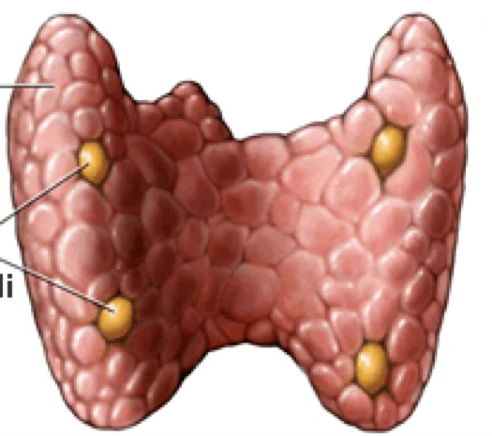
Usually four glands, located on the posterior surface of the thyroid, each in its own collagenous capsule.
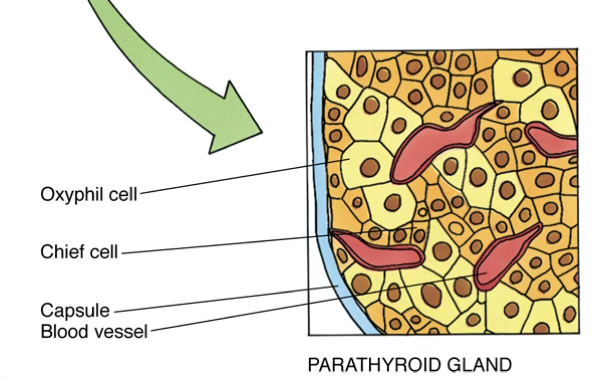
PTH and Calcium
Homeostasis PTH maintains blood at 8.5–10.5 mg/dL by acting on bone, kidney, and intestine to increase calcium concentration.
Cell Types
Chief cells (major parenchymal cells; slightly eosinophilic → lightly stained)
- Contain PTH-secretory granules
- Stimulated by low → release PTH
Oxyphil cells (deeply eosin-stained)
- Function unknown; thought to represent inactive phases of chief cells
- A third “intermediate cell” type also described
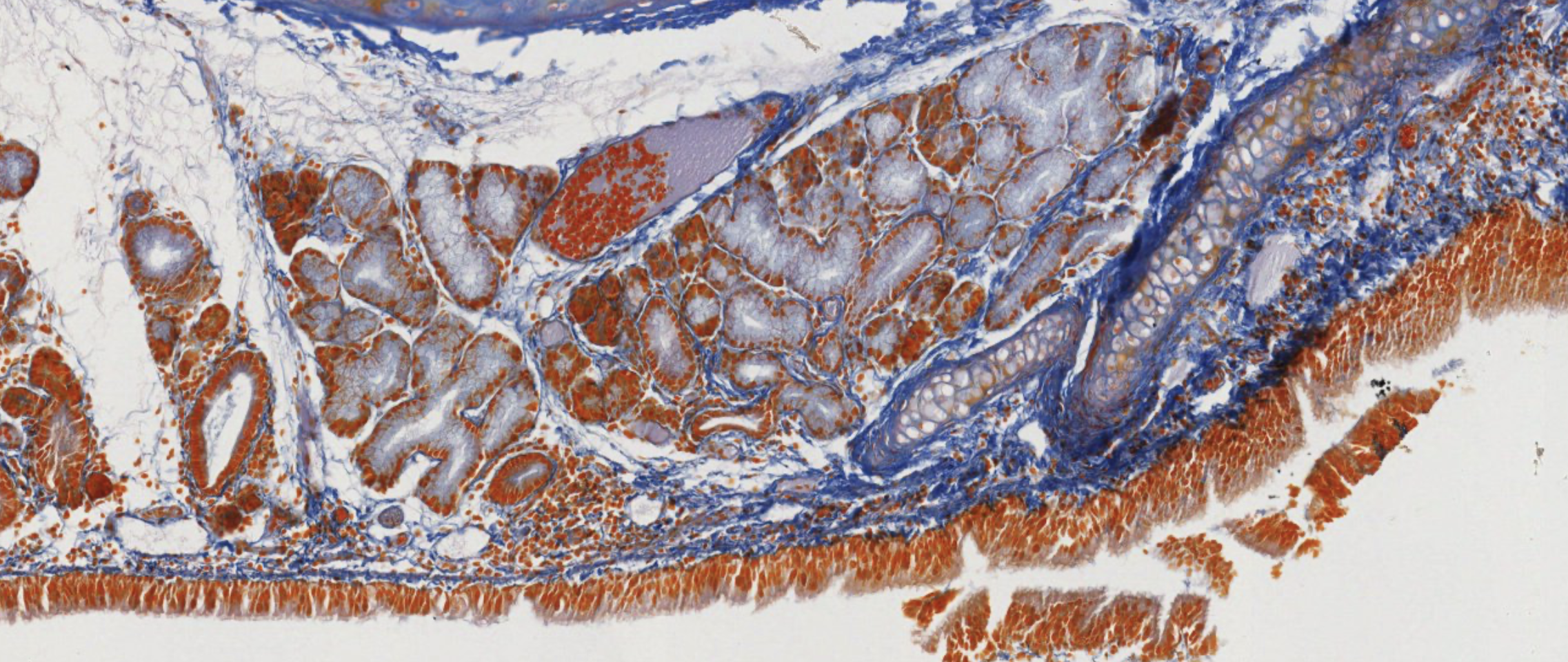
There are exocrine glands here, the secretory units… not alveoli because they’re much wider… it’s tubular. Tubular mucous gland in long wide tubes. Ducts everywhere non si capisce un cazzo.
This is an acinar part, classic pyramid shape. Now, WHERE IS THE THYDROID.
When you find the thyroid, look next to it, and find the capsule covered by connective tissue next to the thyroid.
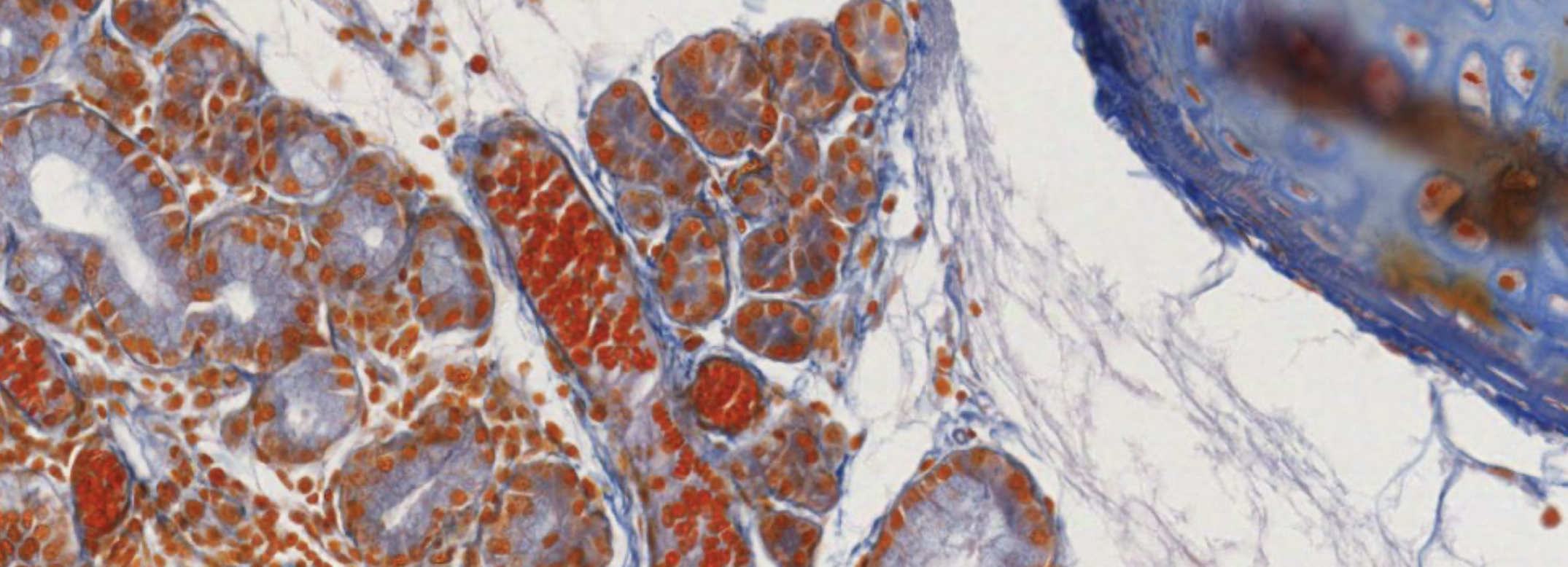
Here it is! We see oxyphil cells very clearly. These are cords of cells… surrounded by the blue strands of connective tissue.
Here it is… Different staining. Oxyphil probably resting or intermediate in the periphery, we don’t know if they’re gonna ever become chief again.
Without the thyroid its hard to find the parathyroid.
PTH Mechanism of Action
non lha spiegato in classe ma non ha detto chiaramente che non ci sarà
Bone: PTH binds osteoblast receptors → secretion of osteoclast-stimulating factor → osteoclast activation → released into blood
Kidney: PTH prevents urinary calcium loss; proximal tubule cells produce calcitriol (active )
Intestine: Calcitriol (active ) is necessary for intestinal absorption from mucosa
Calcitonin vs PTH
These two hormones are antagonists:
- PTH raises blood calcium;
- calcitonin (from thyroid C-cells) lowers it by inhibiting osteoclasts.
Adrenal (Suprarenal) Glands
Divided into two functionally and embryologically distinct regions:
| Region | Origin | Zones / Cells | Hormones |
|---|---|---|---|
| Cortex (outer, yellowish) | Mesoderm (Oral) | Three concentric zones (see below) | Steroids |
| Medulla (inner, dark) | Neural crest | Chromaffin cells | Catecholamines |

The Adrenal Glands are surrounded by a capsule of dense collagenous connective tissue.
Both parts are endocrine glands.
Slides
The Adrenal Medulla has neurons that control the release of adrenaline.
The Adrenal Cortex, the most abundant portion, is composed of epithelial tissue and divided into three zones.
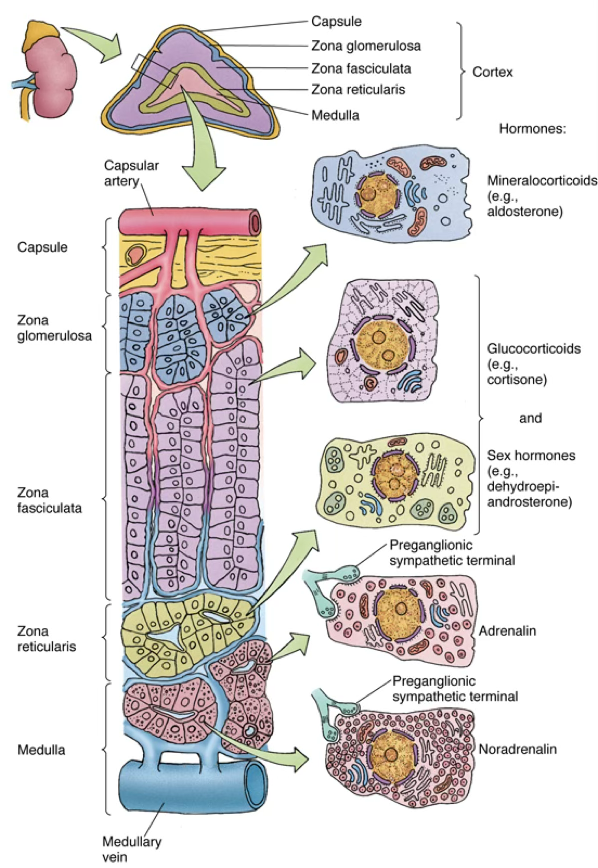
Adrenal Cortex
Mnemonic:
GFR → Salt, Sugar, Sex Zona Glomerulosa → Salt (mineralocorticoids); Zona Fasciculata → Sugar (glucocorticoids); Zona Reticularis → Sex (androgens)
Zona glomerulosa (outermost)
- Closely packed columnar cells.
- Stimulated by angiotensin II and ACTH (secreted by the pituitary gland)
- Produces aldosterone and deoxycorticosterone (mineralocorticoids)
Zona fasciculata (middle, largest)
- Elongated fascicular orientation of cords of cells, usually two-cell thick layers.
- Cells called spongiocytes
- Stimulated by ACTH
- Produces cortisol and corticosterone (glucocorticoids)
Zona reticularis (innermost, tiny, next to the medulla)
- Irregular cords of cells, anastomosing network.
- Stimulated by ACTH
- Produces dehydroepiandrosterone (DHEA), androstenedione, and some glucocorticoids
Adrenal Medulla
- Functionally related to the sympathetic nervous system
- Parenchymal cells = chromaffin cells (modified postganglionic sympathetic neurons)
- Stimulated by preganglionic sympathetic splanchnic nerves
- Produce and release epinephrine and norepinephrine
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1815/i7789/
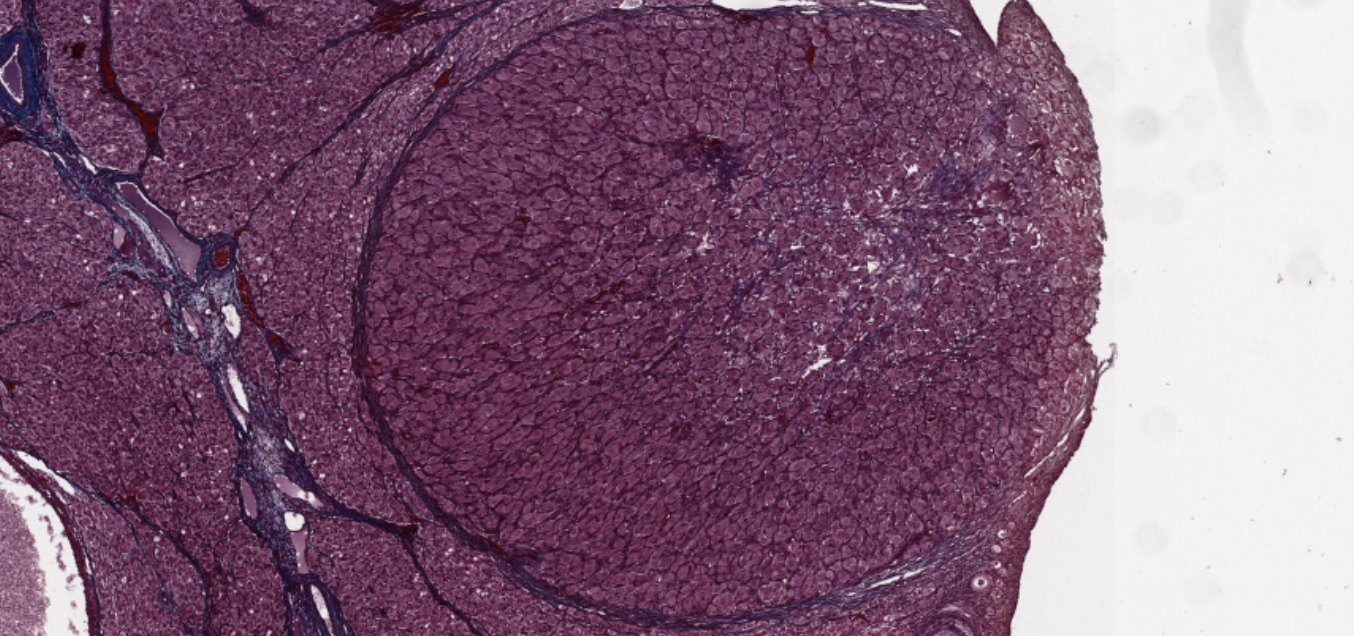
Cords of cells that produce glucocorticoids, followed by (connective tissue?)
The small, few, darker red stained cells… are the somas of the neurons in the medulla.
How do you identify the medulla? By the presence of a loose tissue with many blood vessels, and only in the medulla you see those darker staining.
Lighter blue… These are neurofilaments.
From then the darker staining start, the zona reticularis starts and then fuses into the medulla…
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1815/i1822/
These darker stained figures, that look like Herring Bodies, are the somas of the neurons of the medulla. (They look like Herring bcuz theyre both neurons.)
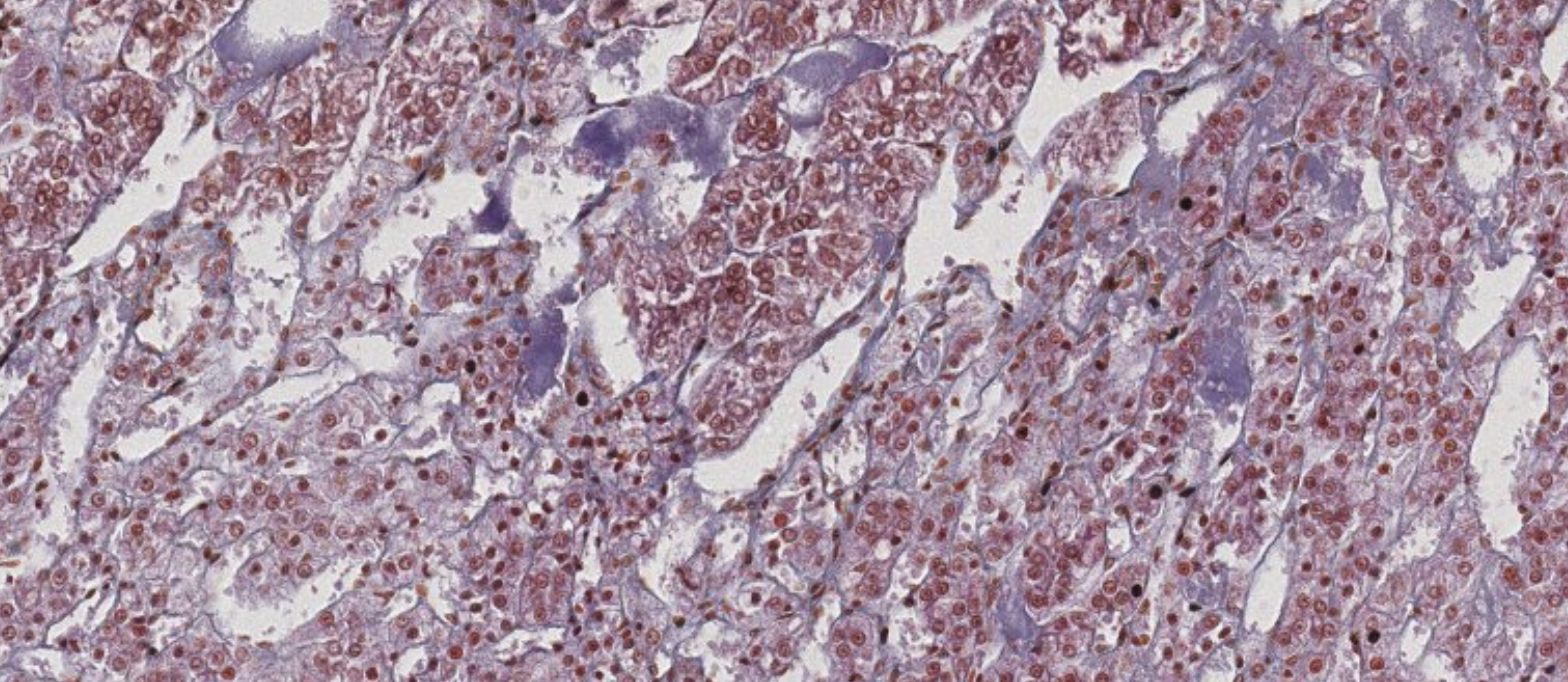
Pineal Gland
Covered by a capsule with septa creating incomplete lobules. Parenchymal cells:
- Pinealocytes (primary secretory cells)
- Interstitial cells (neuroglial)
Function
Produces melatonin and serotonin. Secretion is regulated by light/dark cycles — it is the biological clock interface between environment and endocrine system.
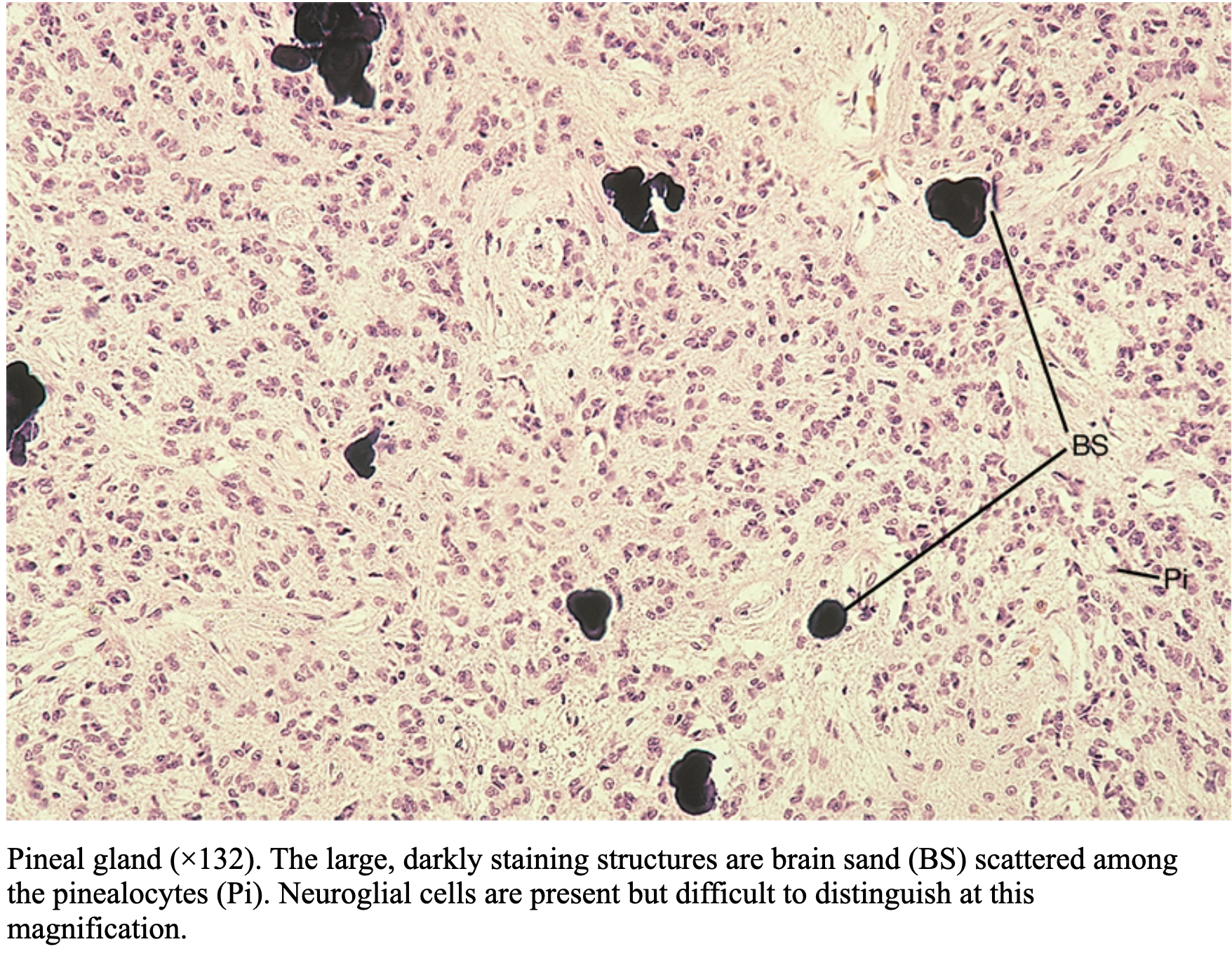
Characteristic finding:
brain sand (corpora arenacea) — darkly staining calcified concretions scattered among pinealocytes.
These are essential to identify the pineal gland.
Circadian Rhythm
Nobel Prize 2017
Jeffrey C. Hall, Michael Rosbash, and Michael W. Young received the Nobel Prize in Medicine (2017) for identifying the genetic basis of circadian rhythms through screening for mutants with altered behavioral rhythms.
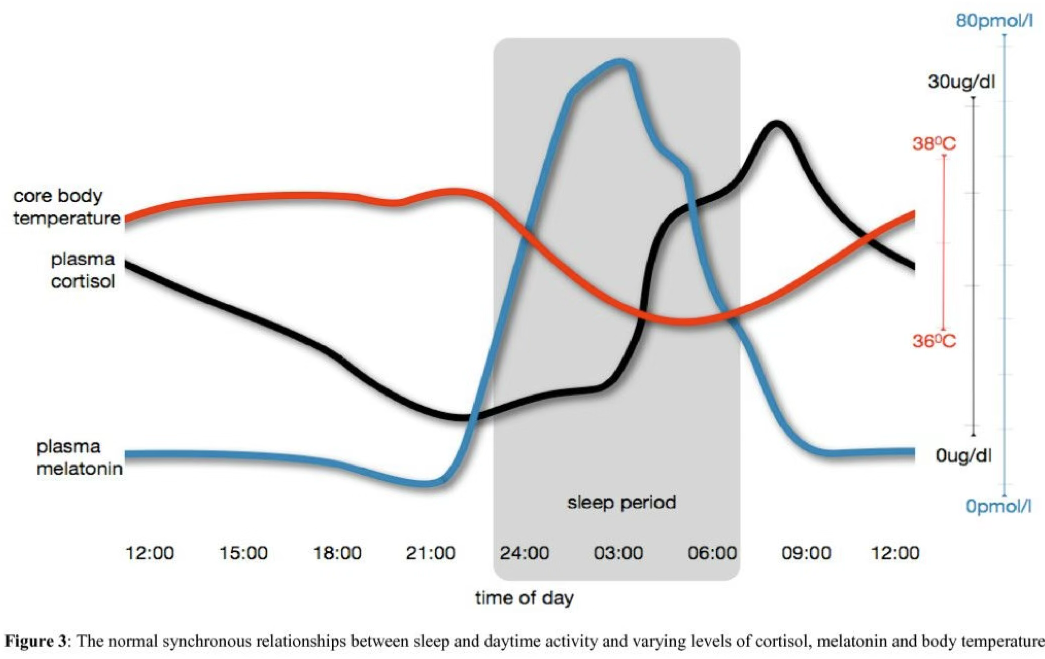
Key findings:
- Circadian rhythm is preserved in the absence of light (Aschoff, 1969)
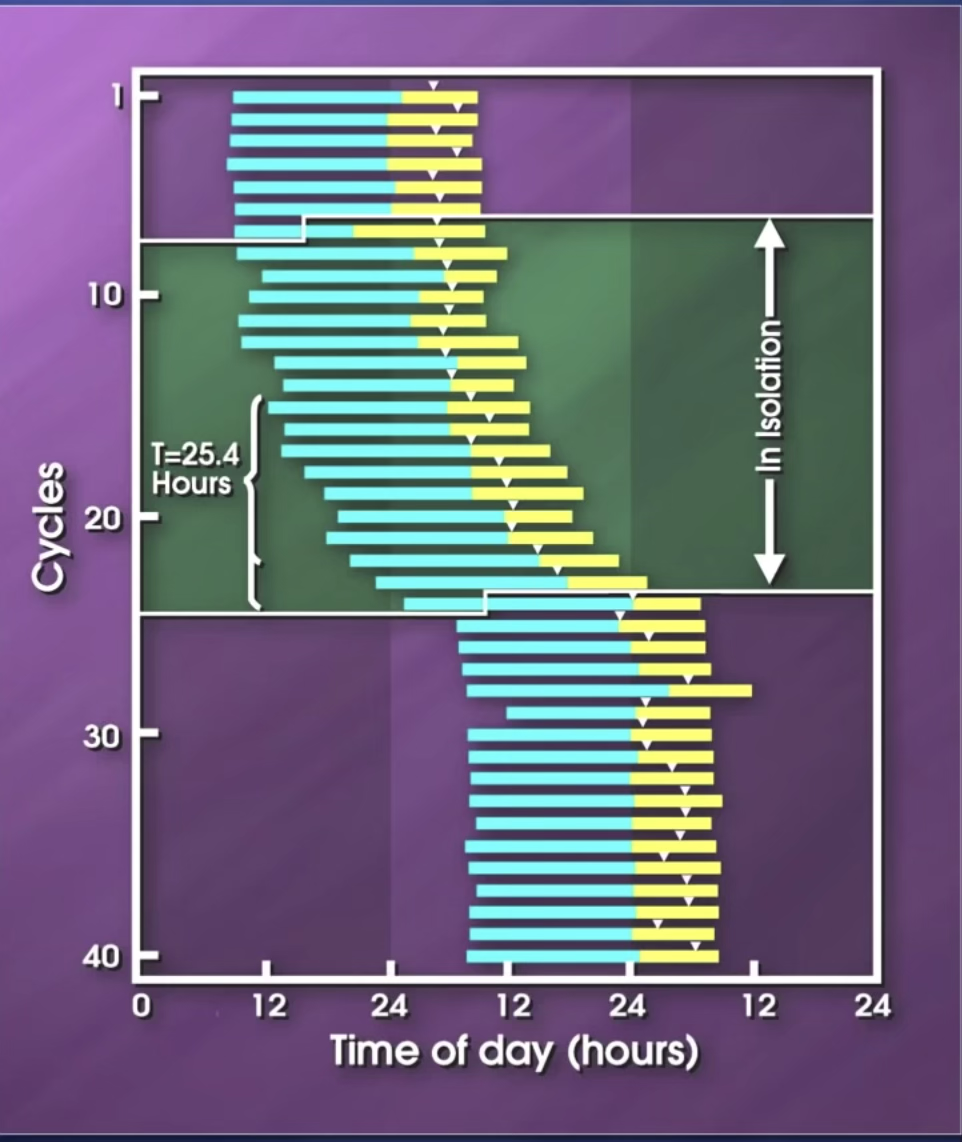
Historical Note
This experiment started in 1969 with Max Planck.
40 Day experiment with students having checks day and night.
(Yellow in the graph → resting time)
At some point, the same student agreed to move to the basement, completely separated from the external environment.
His circadian rhythm was maintained but shifted from 24 to 25.5h.
When he went back to his normal life, he came back to his normal cycle.
- Clock gene oscillations are maintained in vitro in isolated fibroblasts from healthy tissue
- 10–60% of the transcriptome is circadian-regulated
- Circulating glucocorticoids show circadian rhythmicity, peaking at onset of activity — a true clock-regulated process
- Our feeding time also represent a type of internal clock control then diffused to all the tissues in the body.
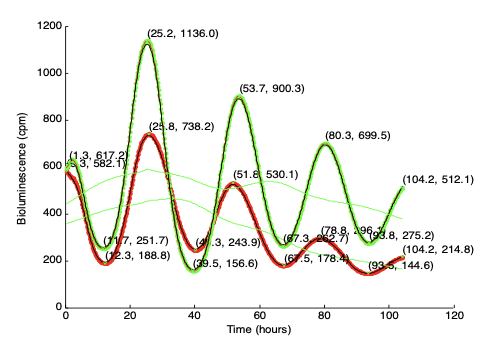
An important application: Chronotherapy
These glucocorticoids are survival hormones (indicators of resting/feeding).
They are able to control the activity of membrane receptors responsible for the proliferation of our cells. Regeneration works better during “resting time”.We can use this knowledge to suppress tumor progression with better timing, attacking the cell when the receptor is more active.
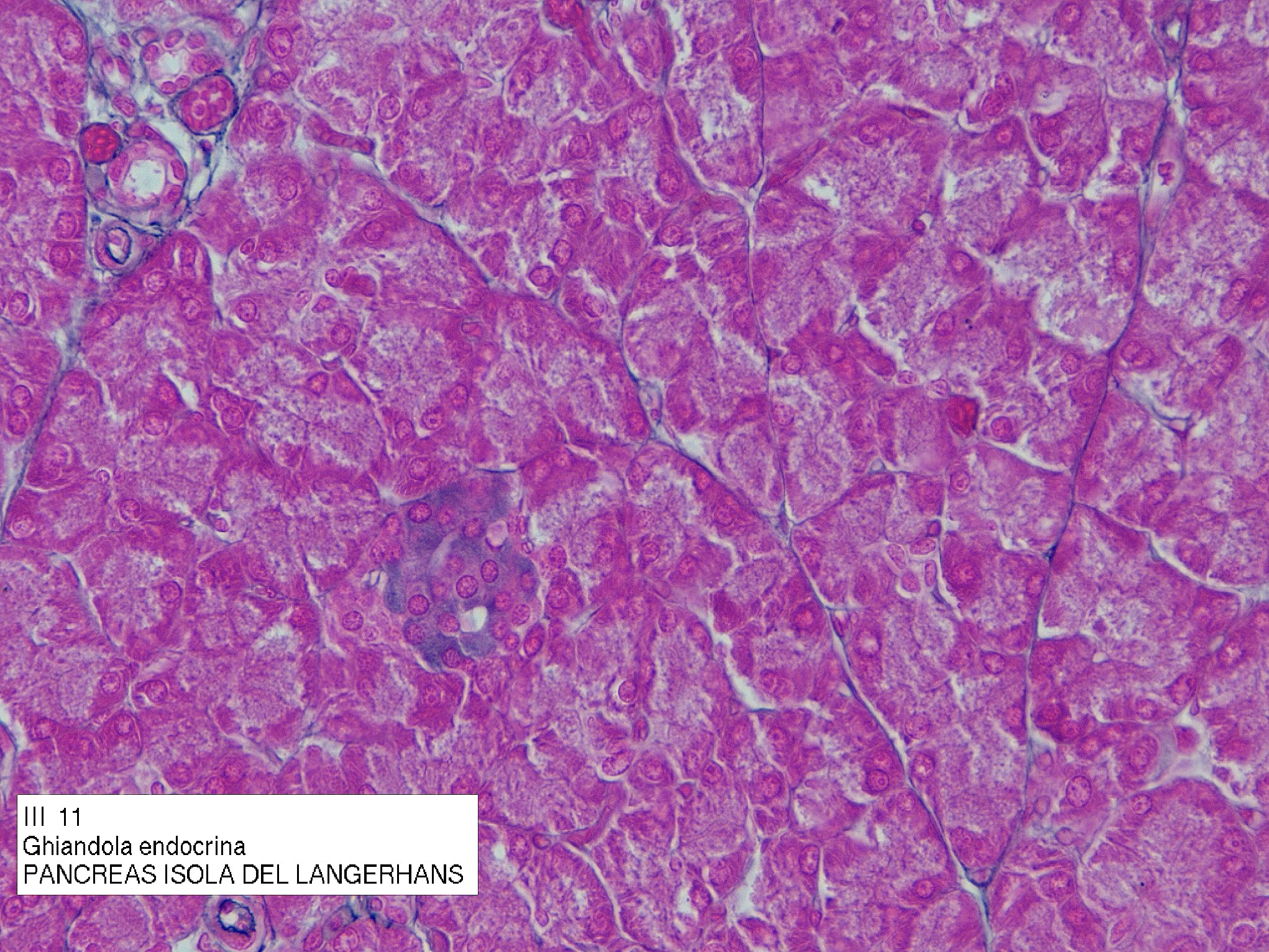
Islets of Langerhans (Pancreatic Endocrine Tissue)
Rounded clusters of ~3,000 cells embedded within exocrine pancreatic tissue.
Each islet is ~0.3 mm in diameter, surrounded by reticular fibers, and highly vascularized. There are 1–2 million islets in the human pancreas.
Five Cell Types
| Cell | Hormone(s) | Function |
|---|---|---|
| β-cells | Insulin, Amylin | Insulin ↓ blood glucose; Amylin inhibits gastric emptying and α-cells |
| α-cells | Glucagon | ↑ blood glucose |
| δ-cells | Somatostatin, VIP | Inhibits endocrine hormone release and exocrine enzyme secretion; VIP regulates smooth muscle tone and glycogenolysis |
| PP cells | Pancreatic polypeptide | Regulates exocrine secretion |
| G cells | Gastrin | Stimulates HCl production in stomach |
Clusters of Cells Within Organs
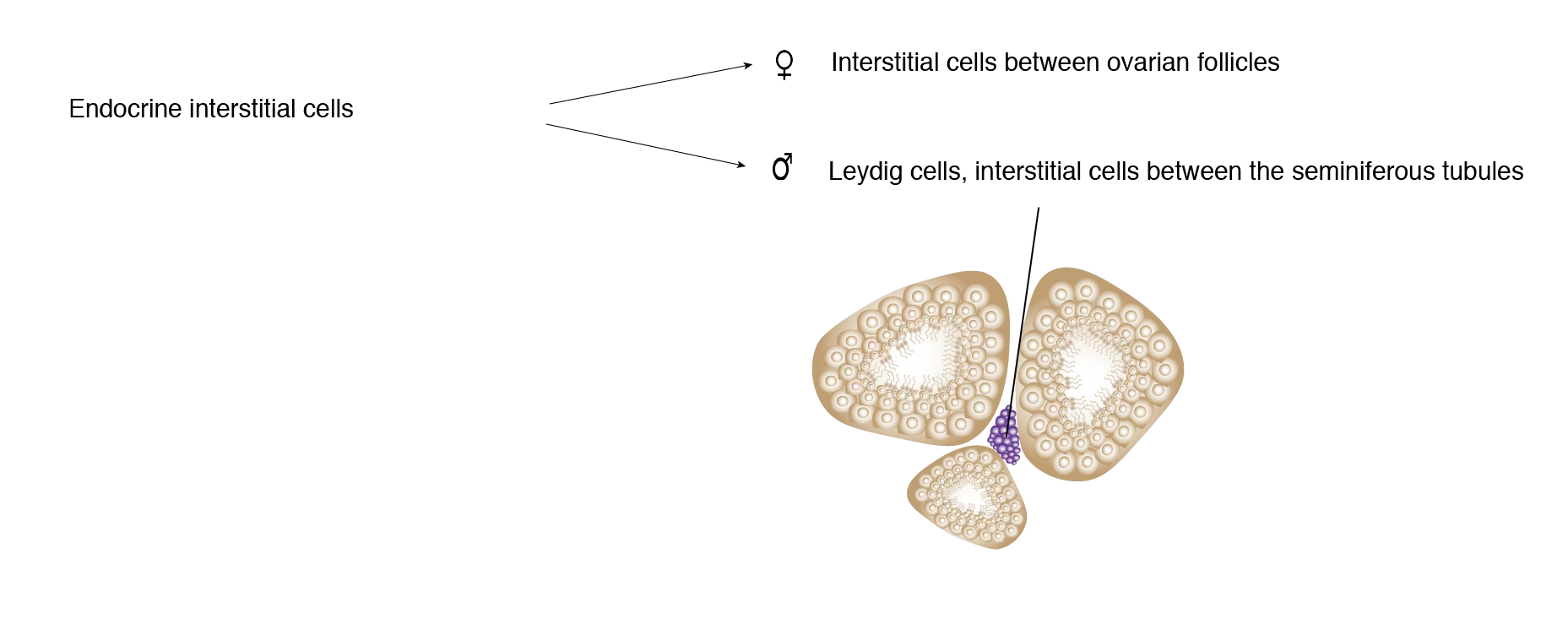
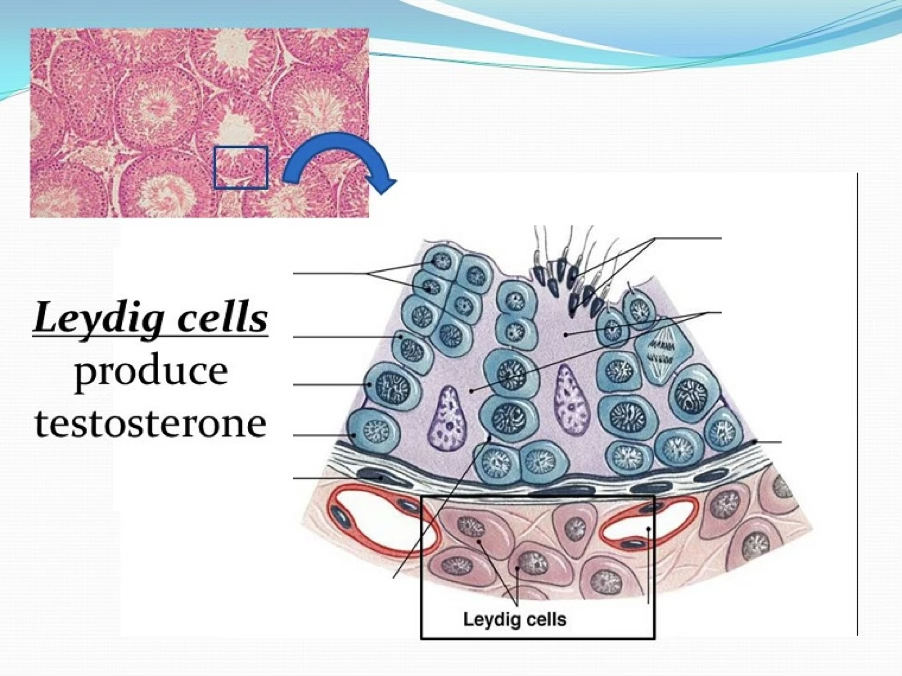
Leydig Cells (Testes)
- Interstitial cells dispersed in loose connective tissue containing fibroblasts and mast cells
- Possess receptors for LH (from anterior pituitary) → stimulates testosterone synthesis pathway
Products
- Testosterone → responsible for spermatogenesis
- INSL3 (insulin-like factor 3) → responsible for testicular descent into scrotum during fetal life
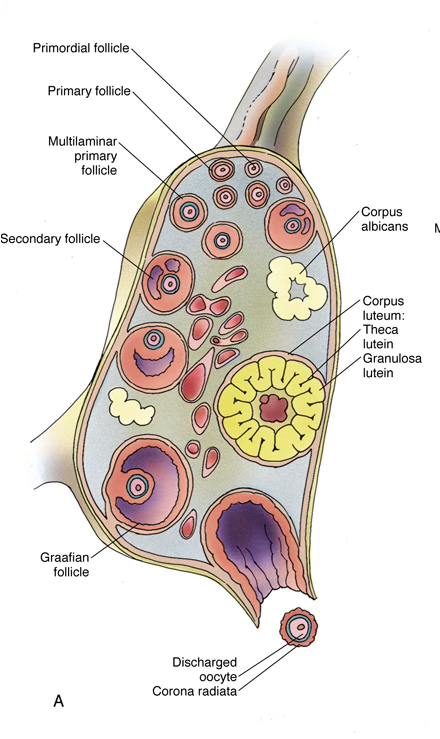
Ovarian Follicles
 | direction of maturation. |
|---|
The paired ovaries (3 × 1.5–2 × 1 cm) are subdivided into:
- Cortex: connective tissue stroma with fibroblast-like stromal cells and follicles at various development stages
- Medulla: large blood vessels, lymph vessels, nerve fibers in connective stroma
Surface covered by germinal epithelium.
Follicular Development Stages
FSH Dependence
Primordial and primary follicle development is FSH-independent (driven by local ovarian factors). Secondary and Graafian follicles require FSH.
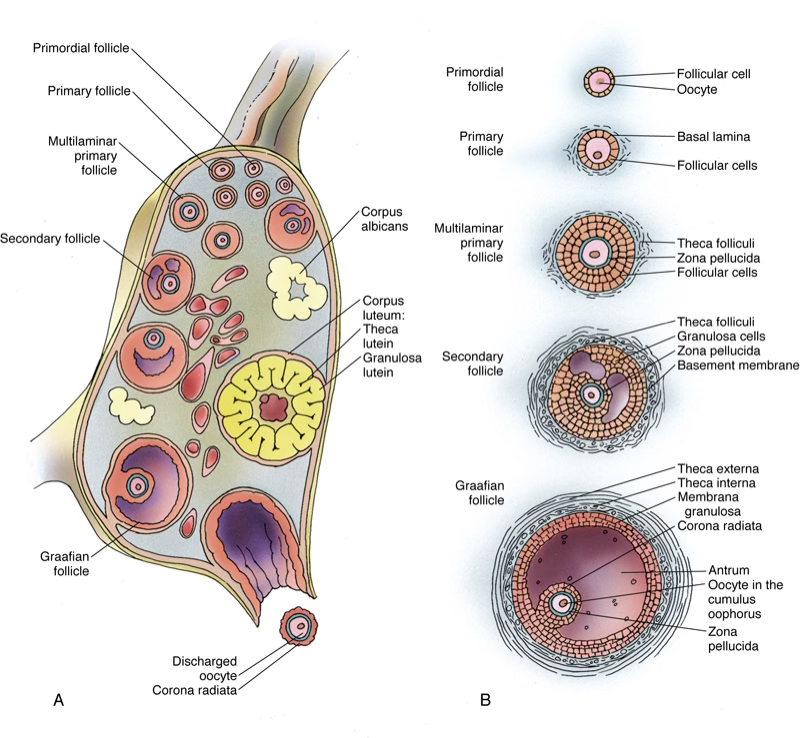
1. Primordial follicles — present before puberty; GnRH (pulsatile) → FSH + LH
Missing notes: associated cells.
2. Unilaminar primary follicle — oocyte grows to 100–150 µm; follicular cells become cuboidal
3. Multilaminar primary follicle — follicular cells proliferate → granulosa cells; zona pellucida appears; stromal cells form:
- Theca interna (richly vascularized) → produces androstenedione → enters granulosa cells → converted by aromatase to estradiol ()
- Theca externa (fibrous connective tissue)
4. Secondary (antral) follicle — liquor folliculi accumulates among granulosa cells; growth depends on FSH from pituitary basophils
5. Graafian (mature) follicle — LH surge from pituitary basophils → ovulation (discharge of mature oocyte)
Post-ovulation: follicle undergoes atresia → granulosa cells → granulosa lutein cells + theca lutein cells → corpus luteum → produces progesterone
If no fertilization, degeneration of the follicle: corpus luteum (progesterone-secreting gland) regresses → corpus albicans (fibrous scar)
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1815/i7793/
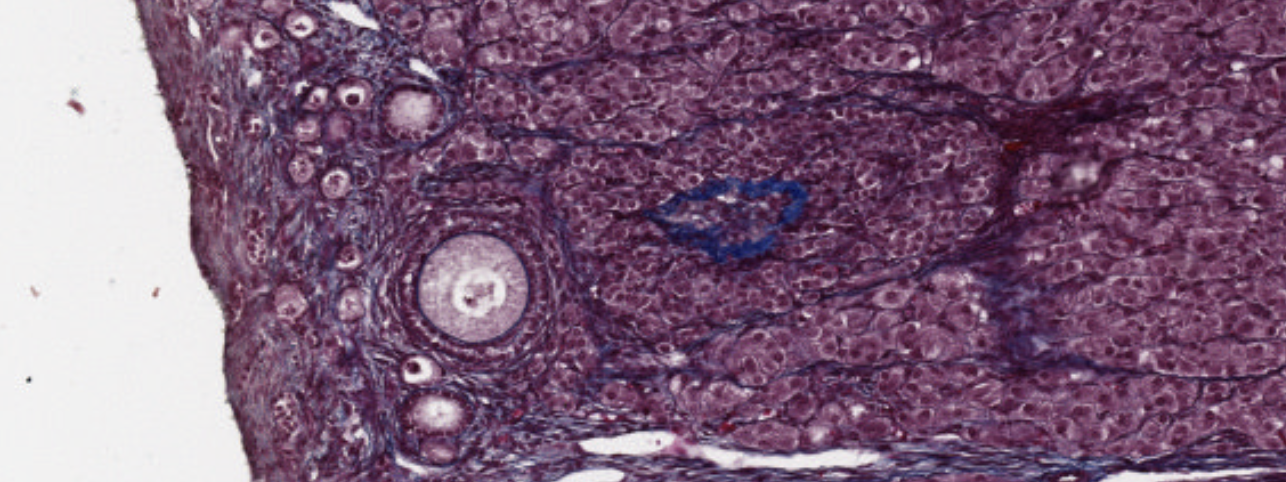
Simple cuboidal epithelium covering the ovary.
Follicular cells maturating over the initial two weeks of the female cycle.
Interstitial cells present in between the follicules, in between the cords, able to secrete estrogen.
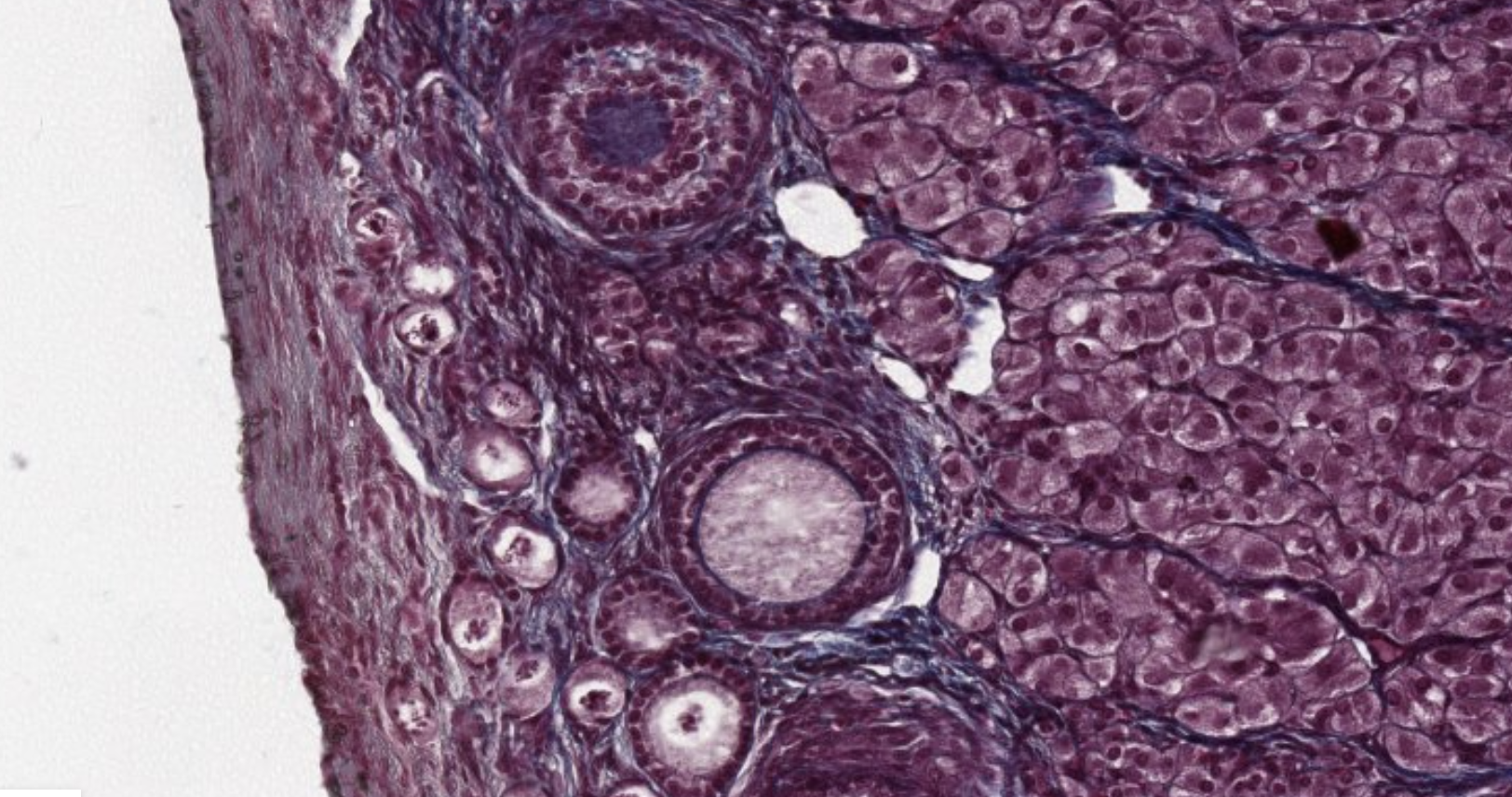
The big ball on the bottom is an oocyte maturating (primordial follicule) with a cuboidal epithelium starting to cover it.
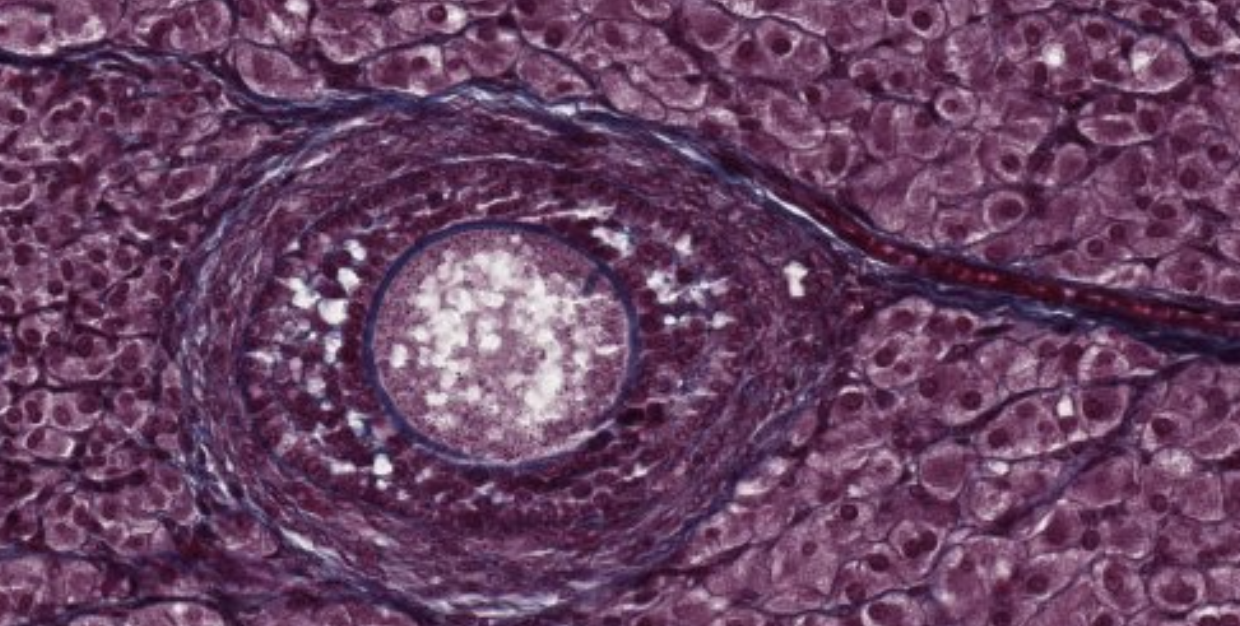
This is a mature follicule. They will continue growing and become…
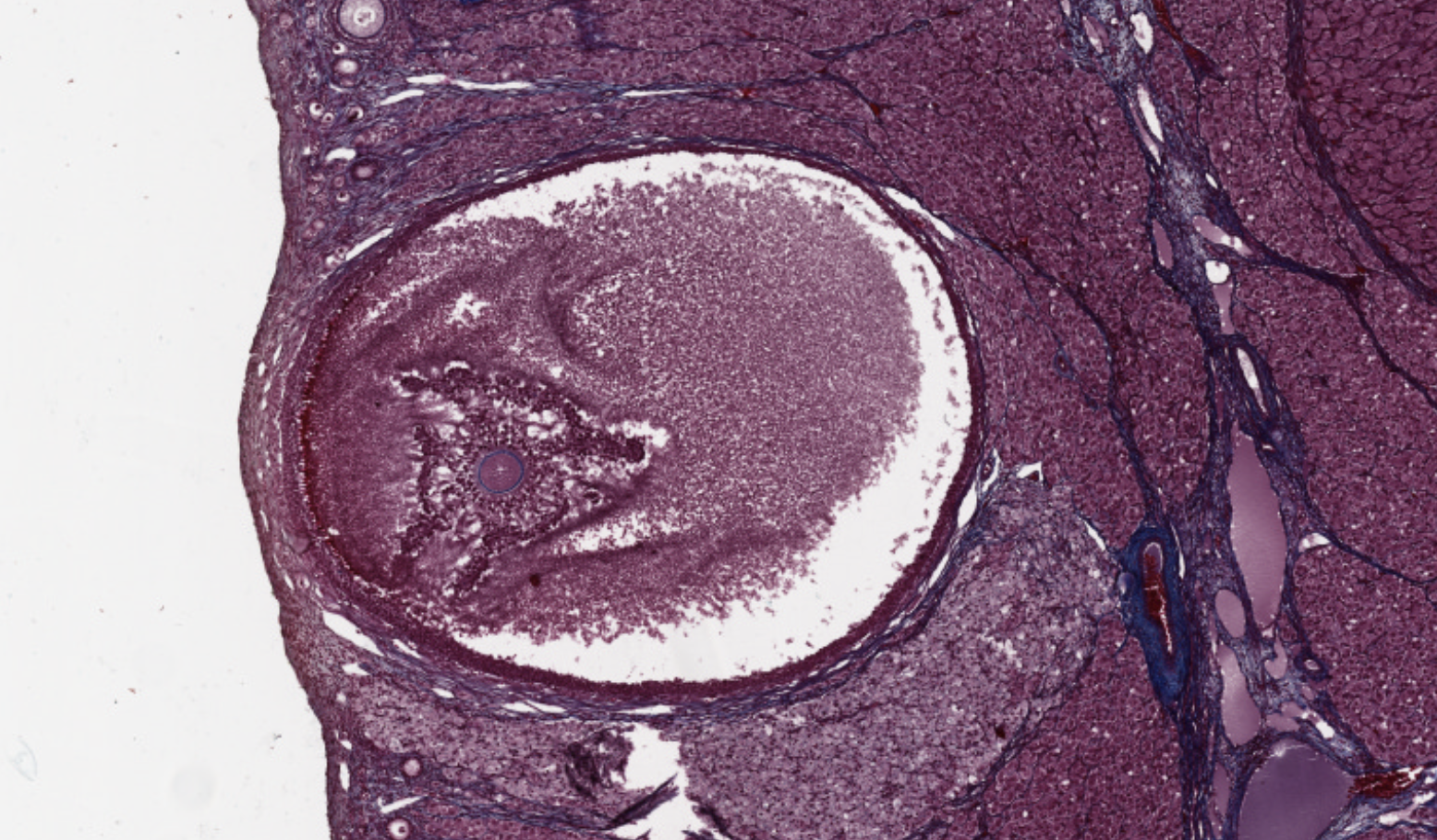
This is giant! It is sustaining the oocyte (blue borders) at the center-sx. It will explode after creating the bulge we can see on the wall of the ovary, then it will release the oocyte.
Bam here ovulation already occurred and they’re still producing estrogen.
Vascular epithelia growth factor is being used to help this structure become a corpus luteum:
This corpus luteum, endocrine organ, will last two weeks and the degenerate. Likely, a new follicule will start a new process of maturation again.
If there is fertilization… the corpus luteum will not disintegrate, but it will stay there and secrete progesterone, being the main source for three months, after which its function will be replaced by the placenta, and the pregnancy wont need the corpus luteum anymore.
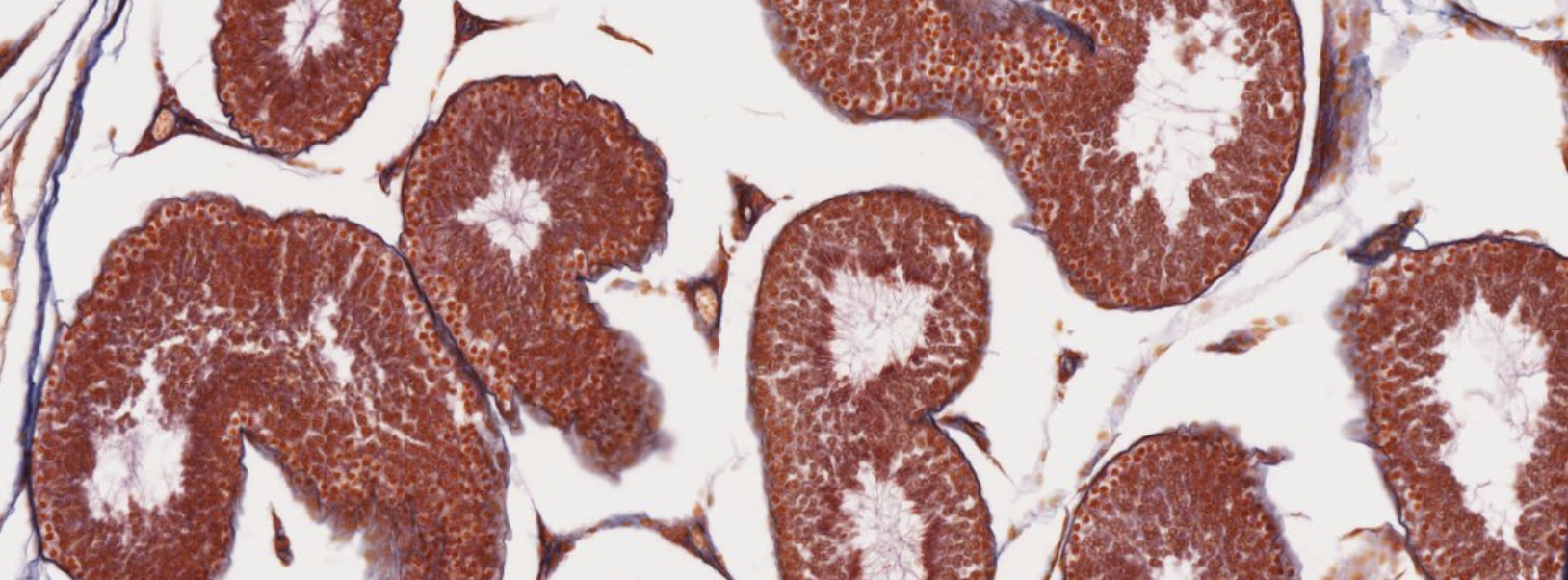
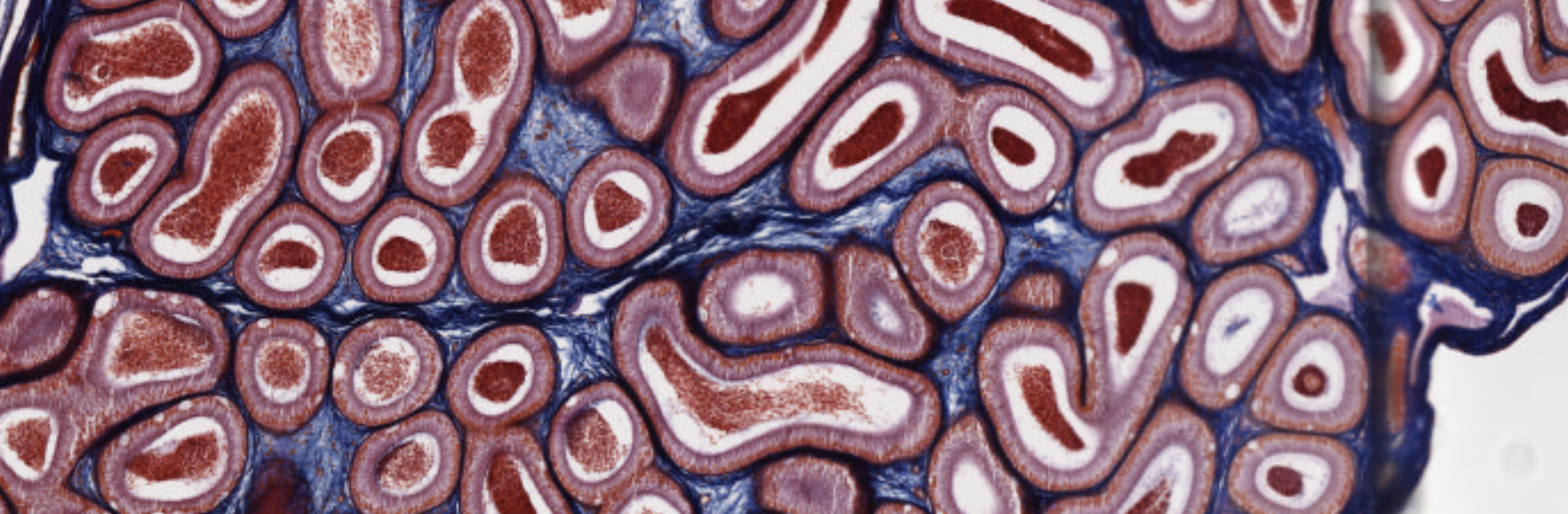
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1815/i7795/
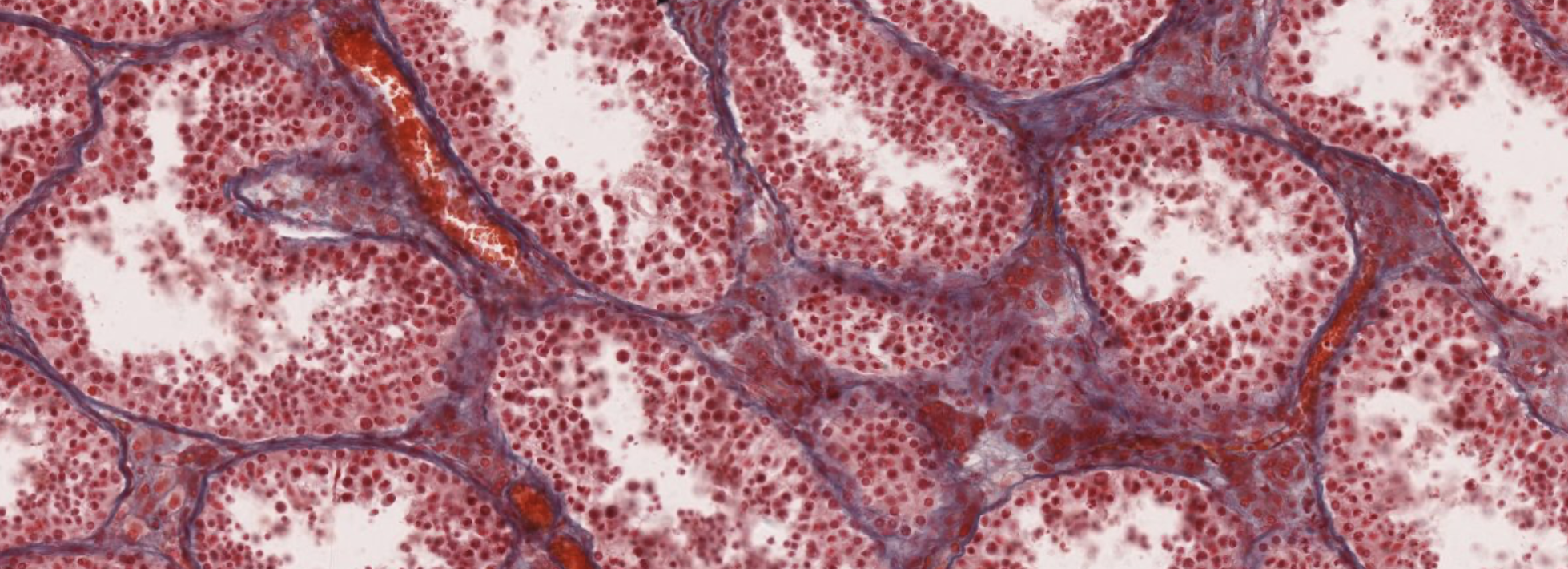
The little triangle structures in between the (?) are the Leydig cells, that produce testosterone.
These are seminiferous tubules.
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1815/i1821/
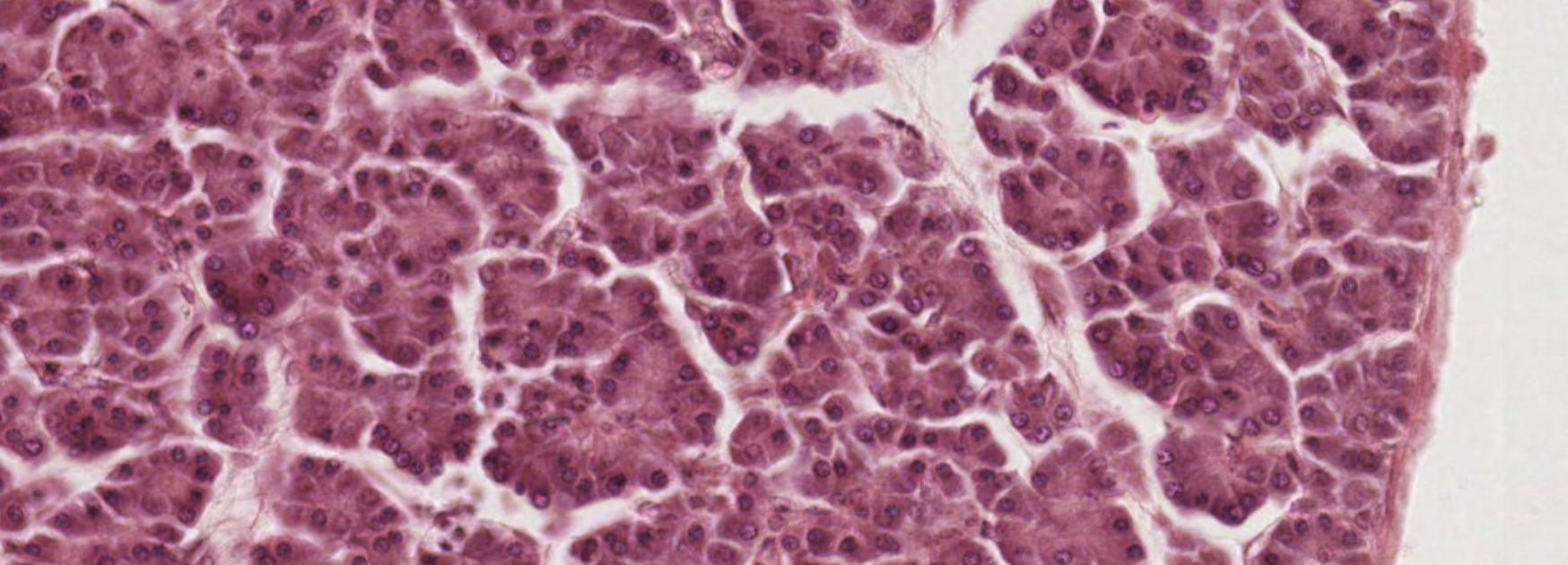
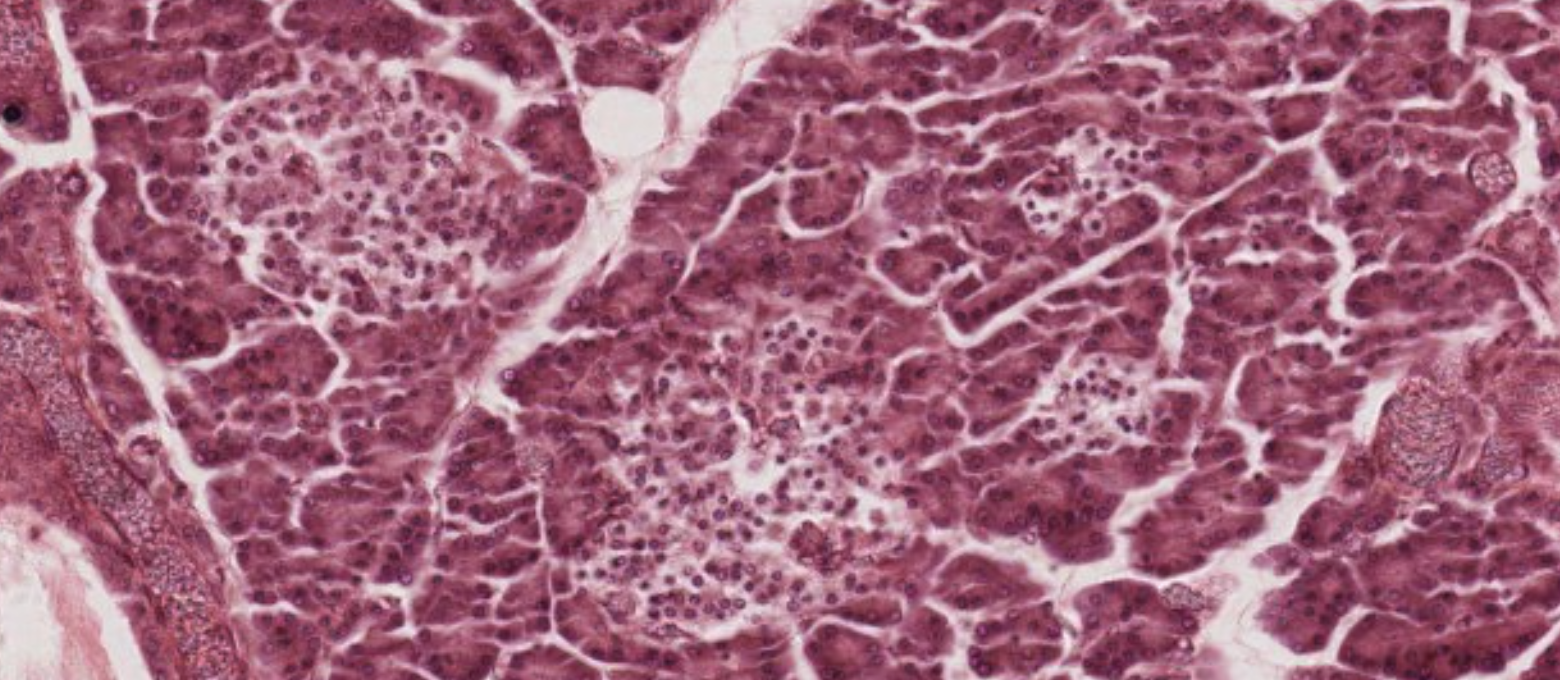
These are compound acinar exocrine glands with a serous secretion.
These clusters of cells are the endocrine glands: Islets of Langerhans. You expect to see blood vessels near them.
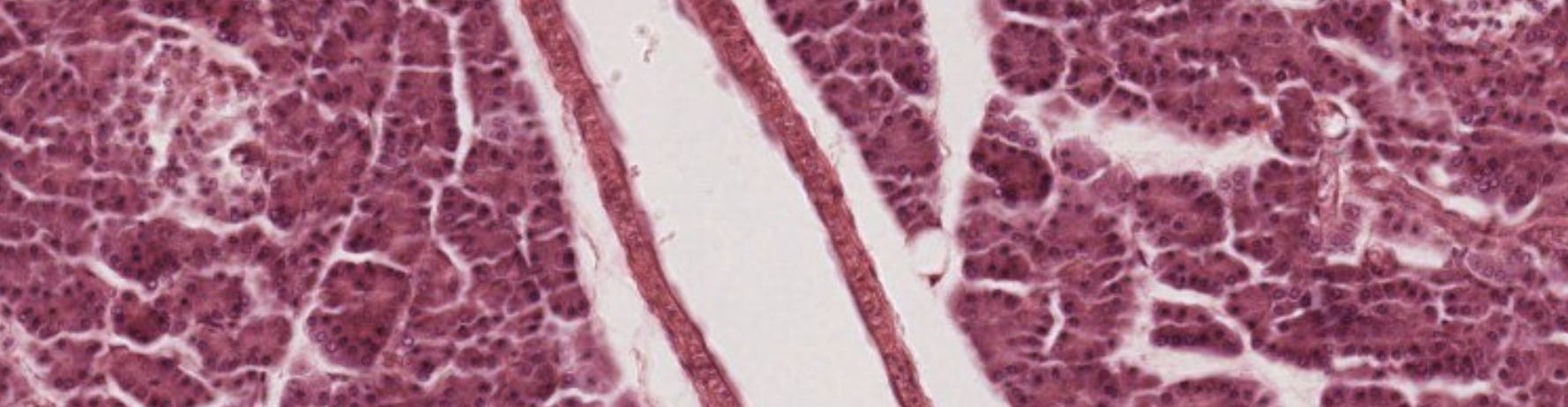
What is this? It’s the main duct, with striation.
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1815/i1816/
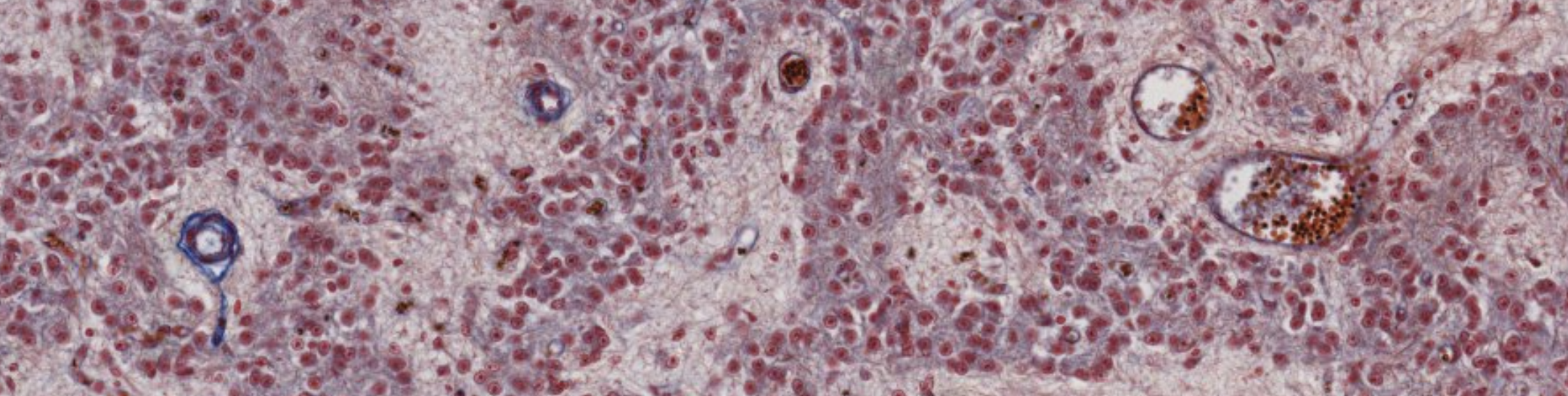
This is pretty anonymous. This is cords of cells, endocrine..
We can see these blue structures… Brain sand! Mineral precipitations.
This is the only specimen of the pineal gland we have.
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1815/i7796/
Triangle parts… Leydig!
TLDR
Endocrine glands are ductless, highly vascularized glands that secrete hormones directly into the blood. Hormones are either water-soluble (polypeptides — act via membrane receptors and second messengers) or lipid-soluble (steroids — cross membranes and act via nuclear receptors to directly influence gene transcription).
The pituitary is the master gland, controlled by the hypothalamus via releasing/inhibiting hormones. Its anterior lobe (adenohypophysis) contains acidophils (somatotrophs → GH; mammotrophs → prolactin) and basophils (corticotrophs → ACTH; thyrotrophs → TSH; gonadotrophs → FSH/LH). The posterior lobe stores hypothalamic hormones.
The thyroid is a follicle-type gland storing / bound to thyroglobulin in colloid. It is activated by TSH, and / exert negative feedback on the hypothalamus and pituitary. C-cells produce calcitonin (lowers ). The parathyroid (chief cells) secretes PTH, which raises via bone resorption, renal reabsorption, and intestinal absorption (via calcitriol/Vit. D). PTH and calcitonin are functional antagonists.
The adrenal cortex has three zones (GFR mnemonic): glomerulosa (aldosterone/mineralocorticoids), fasciculata (cortisol/glucocorticoids), reticularis (DHEA/androgens). The adrenal medulla is derived from neural crest and functions as modified sympathetic neurons secreting epinephrine and norepinephrine.
The pineal gland produces melatonin and serotonin under circadian control. Clock genes drive 10–60% of the transcriptome in a rhythmic fashion; glucocorticoid levels are a key clock-regulated output.
The islets of Langerhans contain five cell types: β-cells (insulin — lowers glucose), α-cells (glucagon — raises glucose), δ-cells (somatostatin — inhibits both endocrine and exocrine secretion), PP cells (pancreatic polypeptide), and G cells (gastrin).
Gonadal endocrine clusters: Leydig cells in the testes produce testosterone (spermatogenesis) and INSL3 (testicular descent) under LH stimulation. In the ovary, follicular development progresses from primordial → primary → secondary → Graafian follicle. Theca interna cells produce androstenedione, which granulosa cell aromatase converts to estradiol. An LH surge triggers ovulation; the ruptured follicle becomes the corpus luteum, which secretes progesterone.
TARGET DECK: MED::I::Morphology and Development::Histology::05 - Endocrine Glands
What are the three structural characteristics of endocrine glands?
- No connection with covering epithelium
- No ducts (ductless)
- High vascularization with fenestrated capillaries
What are the two secretory organizational patterns of endocrine gland parenchyma?
- Cord type: anastomosing cords of cells around capillaries; hormone stored intracellularly
- Follicle type: cells form follicles around a colloid-filled lumen (e.g., thyroid)
Anki cloze
Protein/polypeptide hormones are {1:water-soluble} and bind receptors on the {1:external cell surface}, using a {1:second messenger} system for signal transduction.
Anki cloze
Steroid hormones are {1:lipid-soluble}, penetrate the cell membrane freely, and bind {1:cytoplasmic receptors}. The hormone–receptor complex translocates to the {1:nucleus} to stimulate gene transcription.
What is negative feedback in endocrine axes?
The product of a target gland inhibits upstream hormone secretion, maintaining homeostasis.
What are the embryonic origins of the adenohypophysis and neurohypophysis?
- Adenohypophysis: oral ectoderm (Rathke’s pouch); controlled by BMP4, FGF8, WNT5
- Neurohypophysis: neural ectoderm; contains pituicytes (glial cells) and Herring bodies
Anki cloze
The neurohypophysis does not {1:produce} hormones — it only {1:secretes} them. Hormones are produced by neurons in the {1:hypothalamus}.
Which hypothalamic nuclei project axons into the neurohypophysis?
Paraventricular and supraoptic nuclei.
Match each hypothalamic hormone to its action:
Hormone Action TRH Stimulates TSH release CRH Stimulates ACTH release GHRH (SRH) Stimulates GH release GnRH Stimulates LH and FSH PRH Stimulates prolactin PIF (dopamine) Inhibits prolactin
What are the three major cell categories of the adenohypophysis?
- Acidophils (chromophils)
- Basophils (chromophils)
- Chromophobes (likely senescent/non-secreting cells)
Which cells of the adenohypophysis are acidophils and what do they secrete?
- Somatotrophs → somatotropin (GH)
- Mammotrophs → prolactin
Anki cloze
GH acts on the liver to produce {1:IGF-I and IGF-II}, which stimulate {1:epiphyseal plate chondrocyte mitosis} → long bone elongation.
What does POMC get cleaved into (corticotrophs)?
- ACTH → adrenal cortex zona fasciculata → glucocorticoid release
- LPH → lipolysis, steroid synthesis, melanin production
- ACTH further → MSH → melanin
- LPH further → β-endorphin
What are the three basophil cell types of the adenohypophysis and their secretions?
- Corticotrophs → ACTH (via POMC cleavage)
- Thyrotrophs (~) → TSH
- Gonadotrophs (~) → FSH and LH
Anki cloze
TSH is stimulated by {1:TRH} and inhibited by {1: and }. It acts on thyroid follicular cells to release {1: and }.
What hormones does the thyroid gland produce and what are their half-lives?
- (triiodothyronine): high affinity, 1-day half-life
- (thyroxine): of released hormone, 6-day half-life
- Calcitonin: produced by C-cells (parafollicular); decreases blood
What is the colloid of the thyroid follicle?
The central lumen of thyroid follicles storing inactive and bound to thyroglobulin (a large secretory glycoprotein). It provides several weeks’ hormone supply.
Anki cloze
Upon TSH stimulation, thyroid follicular cells develop apical {1:filopodia}, {1:endocytose} colloid aliquots, and / are cleaved by {1:lysosomal proteases} and released basally into blood vessels.
Anki cloze
Iodide () is essential for / synthesis. Iodination of {1:tyrosine residues} occurs at the {1:colloid–follicular cell interface}.
What are parafollicular (C) cells and what do they produce?
- – larger than follicular cells; only of thyroid epithelium
- Produce calcitonin → inhibits osteoclast bone resorption → lowers blood
What is the thyroid axis negative feedback loop?
What are the two cell types of the parathyroid gland and their functions?
- Chief cells: contain PTH granules; stimulated by low → release PTH
- Oxyphil cells: deeply eosinophilic; function unknown; thought to represent inactive/senescent chief cells
What is the normal blood calcium range maintained by PTH?
– mg/dL
How does PTH act on bone, kidney, and intestine?
- Bone: binds osteoblast receptors → stimulates osteoclast activity → releases
- Kidney: prevents urinary loss; produces calcitriol (active )
- Intestine: calcitriol enables intestinal absorption
Anki cloze
PTH {1:raises} blood calcium, while calcitonin {1:lowers} it — they are functional {1:antagonists}.
What is the GFR mnemonic for the adrenal cortex?
- Zona Glomerulosa → Salt (mineralocorticoids: aldosterone)
- Zona Fasciculata → Sugar (glucocorticoids: cortisol)
- Zona Reticularis → Sex (androgens: DHEA)
What are the embryological origins of the adrenal cortex and medulla?
- Cortex: mesoderm → steroid hormones
- Medulla: neural crest → catecholamines (epinephrine, norepinephrine)
Anki cloze
The zona glomerulosa is stimulated by {1:angiotensin II} and {1:ACTH} and produces {1:aldosterone} (mineralocorticoids).
Anki cloze
The cells of the zona fasciculata are called {1:spongiocytes}. They are stimulated by {1:ACTH} and produce {1:cortisol} (glucocorticoids).
What are chromaffin cells and what do they secrete?
Modified postganglionic sympathetic neurons in the adrenal medulla. Stimulated by preganglionic sympathetic splanchnic nerves. Secrete epinephrine and norepinephrine.
What is the characteristic histological finding of the pineal gland?
Brain sand (corpora arenacea) — darkly staining calcified concretions scattered among pinealocytes. Essential for identifying the gland.
What does the pineal gland produce and how is secretion regulated?
Produces melatonin and serotonin. Regulated by light/dark cycles — it is the biological clock interface between environment and endocrine system.
Anki cloze
{1:–} of the transcriptome is circadian-regulated. Circulating {1:glucocorticoids} show circadian rhythmicity, peaking at the onset of {1:activity}.
What are the five cell types of the islets of Langerhans and their hormones?
Cell Hormone Function β-cells Insulin, Amylin ↓ blood glucose; inhibits gastric emptying α-cells Glucagon ↑ blood glucose δ-cells Somatostatin, VIP Inhibits endocrine + exocrine secretion PP cells Pancreatic polypeptide Regulates exocrine secretion G cells Gastrin Stimulates HCl in stomach
What do Leydig cells produce and what stimulates them?
Stimulated by LH (anterior pituitary).
- Testosterone → spermatogenesis
- INSL3 (insulin-like factor 3) → testicular descent into scrotum during fetal life
Which stages of ovarian follicle development are FSH-independent vs FSH-dependent?
- FSH-independent: primordial and primary follicles (driven by local ovarian factors)
- FSH-dependent: secondary (antral) and Graafian follicles
How is estradiol ( ) produced in the developing ovarian follicle?
Theca interna cells produce androstenedione → enters granulosa cells → converted by aromatase to estradiol ().
Anki cloze
An LH surge triggers {1:ovulation}. Post-ovulation, the follicle becomes the {1:corpus luteum}, which secretes {1:progesterone}.
Anki cloze
If no fertilization occurs, the corpus luteum degenerates into the {1:corpus albicans} (fibrous scar). If fertilization occurs, the corpus luteum persists for {1:three months} until the {1:placenta} takes over progesterone secretion.
What are the two zones of the ovary?
- Cortex: connective tissue stroma with follicles at various development stages
- Medulla: large blood vessels, lymph vessels, nerve fibers in connective stroma