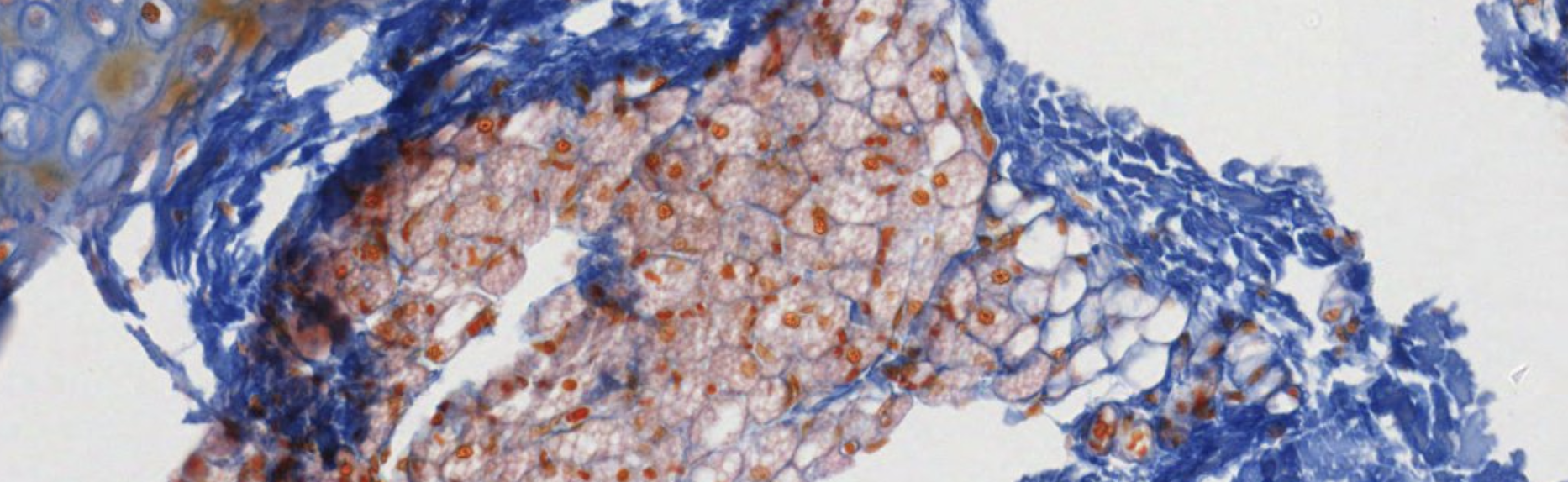
Definition & Composition
Connective tissue provides the supportive and connecting framework (stroma) for all other body tissues.
It is composed of three elements:
- Cells
- Fibers
- Extracellular matrix (ECM) — also called ground substance
ECM Definition
The ECM is a combination of collagens, non-collagenous glycoproteins, and proteoglycans surrounding the cells of the connective tissue.
Resident (fixed) cells: fibroblasts
Immigrant (transient) cells: macrophages, mast cells, plasma cells
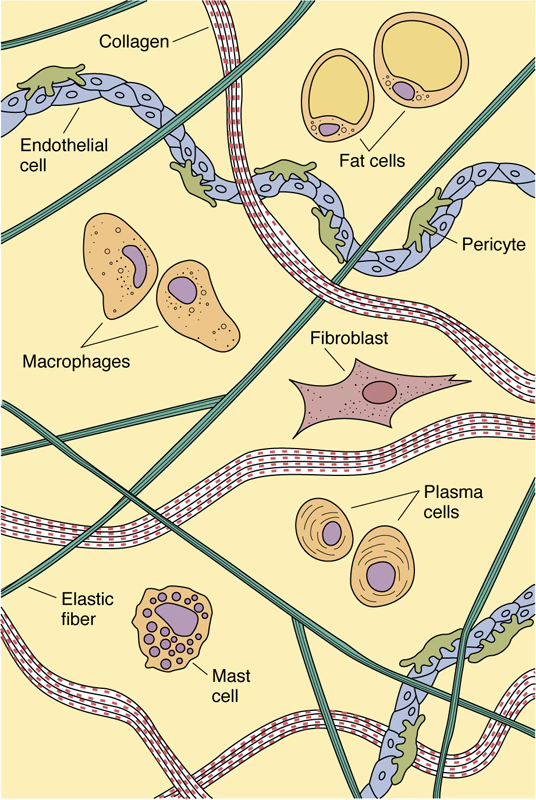
Classification of Connective Tissue
Connective Tissue
├── Connective Tissue Proper
│ ├── Embryonic / Mucous tissue
│ │ ├── Mesenchymal (e.g. pulp of young teeth)
│ │ └── Mucous (e.g. Wharton's jelly in umbilical cord)
│ ├── Loose CT — more cells (fibroblasts, macrophages), fewer fibers
│ ├── Dense CT — fewer cells, more fibers
│ │ ├── Irregular — random fiber orientation (e.g. dermis, submucosa)
│ │ ├── Regular — parallel fiber orientation (e.g. tendons, ligaments,cornea)
│ │ └── Crossed fibers — crossed collagen (e.g. cornea)
│ ├── Reticular CT
│ └── Elastic CT
└── Specialized CT
├── Cartilage
├── Bone
├── Blood
└── Adipose tissue
Dense vs. Loose
- Loose CT: cell/fiber ratio is high → cells dominate
- Dense CT: cell/fiber ratio is low → fibers dominate
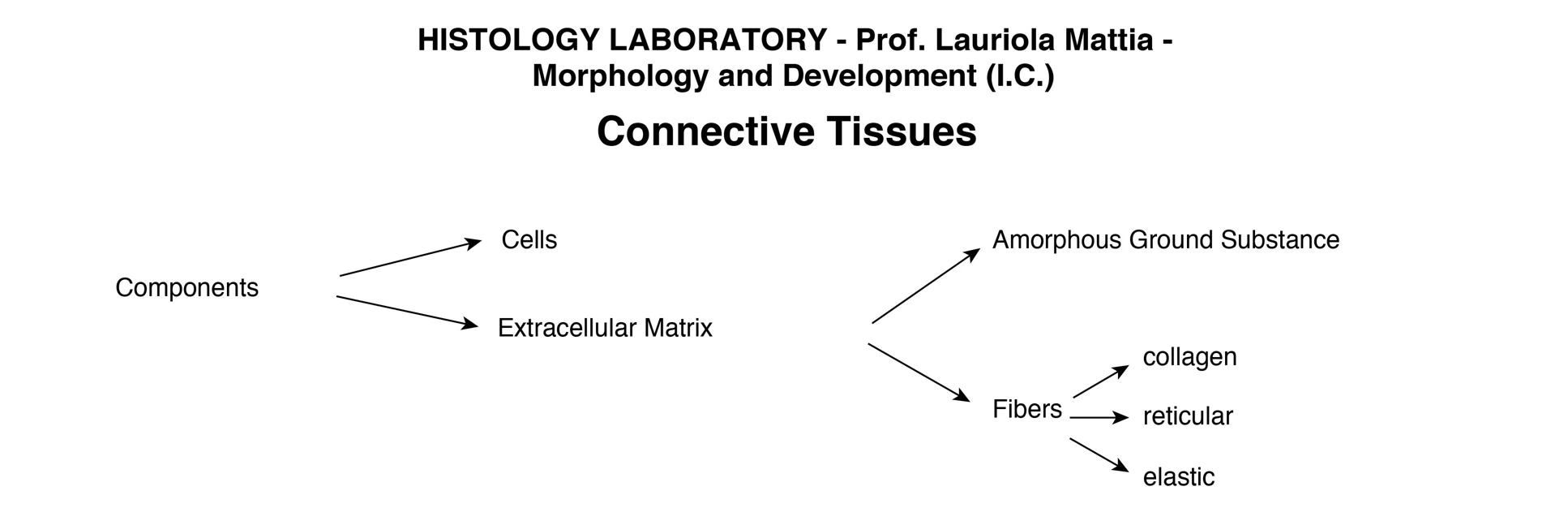
Classifying... 046 mesenchyme
Extracellular Matrix (ECM)
The ECM resists both compressive and stretching forces. It consists of ground substance and fibers.
Ground Substance
An amorphous, hydrated material composed of:
- Glycosaminoglycans (GAGs)
- Proteoglycans
- Adhesive glycoproteins
Glycosaminoglycans (GAGs)
| Type | Examples |
|---|---|
| Sulfated | Keratan sulfate, heparan sulfate, heparin, chondroitin sulfate, dermatan sulfate |
| Non-sulfated | Hyaluronic acid |
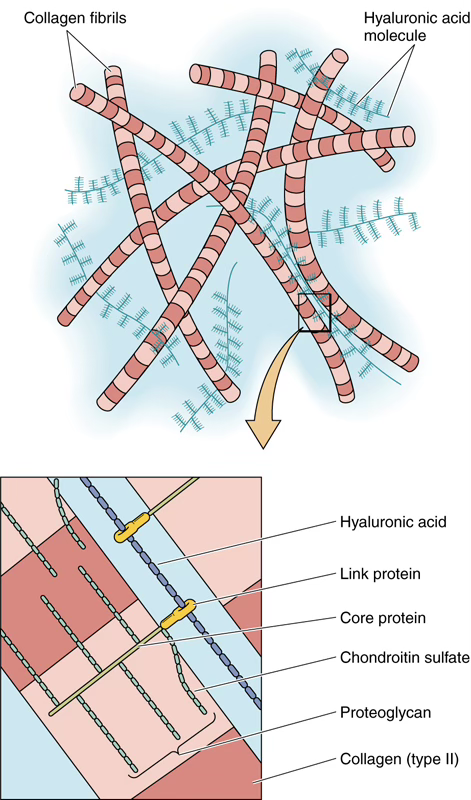
Proteoglycans
Proteoglycans are covalently linked to hyaluronic acid forming huge macromolecules called aggrecan aggregates — responsible for the gel-state of the ECM.
Molecular mass of a proteoglycan
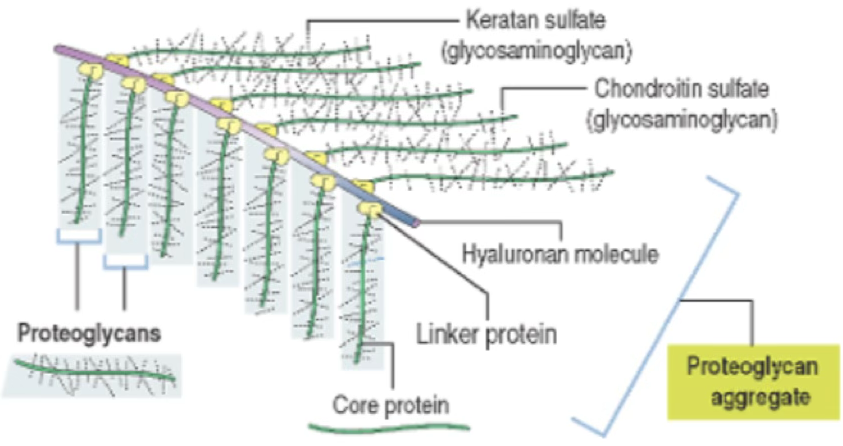
Adhesive Glycoproteins
| Glycoprotein | Location |
|---|---|
| Laminin | Basal lamina |
| Chondronectin | Cartilage |
| Osteonectin | Bone |
| Fibronectin | Throughout ECM |
Fibers of the ECM
Collagen Fibers
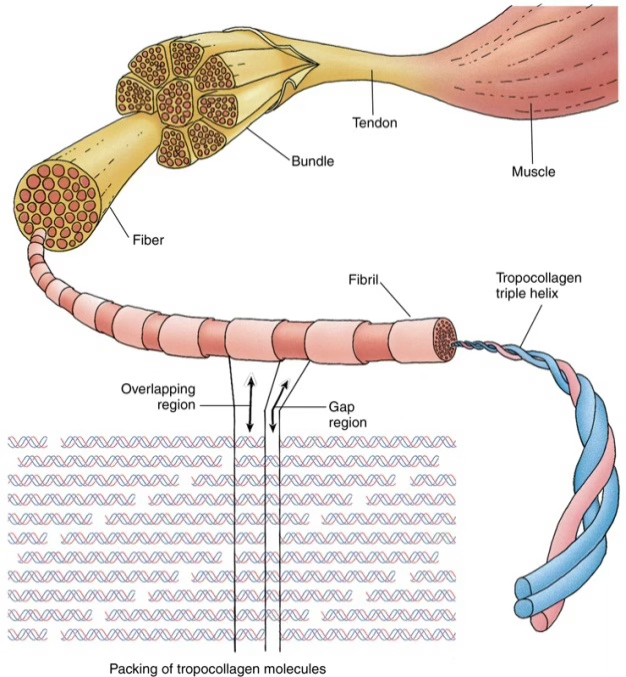
Collagen fibers are inelastic with great tensile strength.
Each fiber is composed of tropocollagen molecules — three -chains wrapped in a triple helix:
The ordered packing of tropocollagen creates gap and overlap regions, producing the characteristic 67 nm cross-banding of type I collagen.
Major Collagen Types
Type Location Notes I CT proper, bone, dentin, cementum Two + one chain II Hyaline & elastic cartilage Resists pressure III Reticular fibers Forms stroma of lymphoid organs & liver IV Lamina densa of basal lamina Network-forming; no 67 nm periodicity V Associated with type I, placenta — VII Anchoring fibrils Attaches basal lamina to lamina reticularis
Reticular Fibers (Type III Collagen)
- Form a fine meshwork (stroma) in lymph nodes, spleen, hematopoietic bone marrow, and liver
- Provide a delicate framework allowing passage of cells and fluid
Elastic Fibers
Composition
Elastic fibers = elastin (amorphous core) + microfibrils (peripheral scaffold)
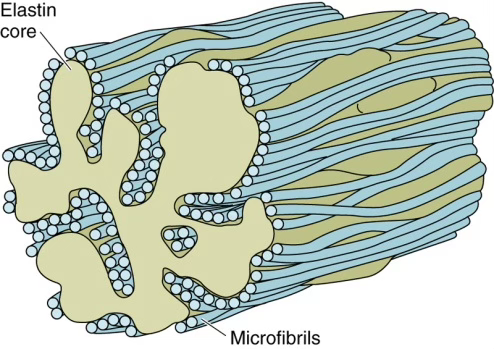
- Can be stretched to 150% of resting length without breaking
- Key amino acids in elastin: glycine, proline, lysine
- Lysine forms desmosine residues → responsible for high elasticity
- Found in: vertebral ligaments, aortic wall (concentric laminae)
Cells of Connective Tissue
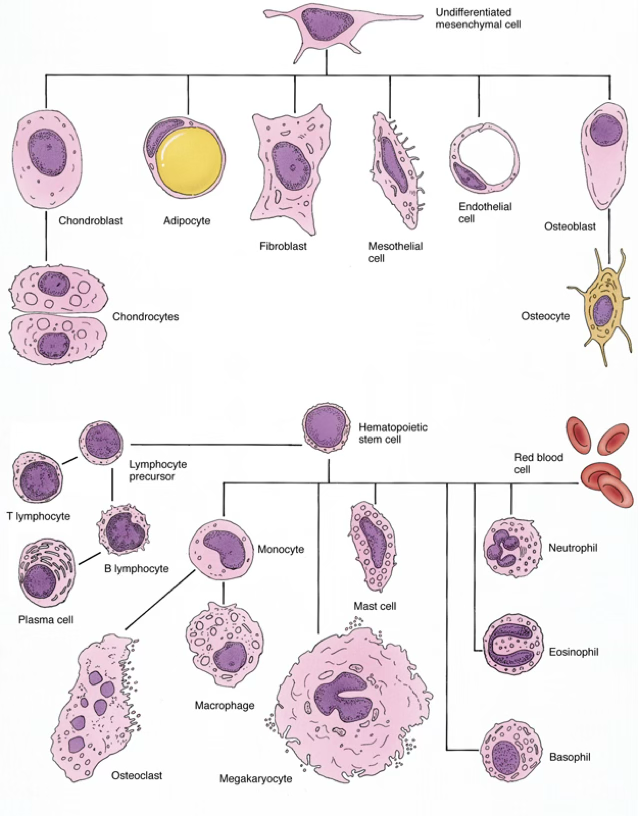
Fixed (Resident) Cells
Long-lived, develop and remain in connective tissue:
| Cell | Key Function |
|---|---|
| Fibroblasts | Manufacture & maintain ECM fibers and ground substance |
| Adipocytes | Fat storage; endocrine signaling |
| Pericytes | Support vascular walls |
| Mast cells | Immune/inflammatory mediator release |
| Macrophages* | Phagocytosis, antigen presentation |
Transient (Wandering) Cells
Originate in bone marrow, circulate in blood, migrate into CT when stimulated:
Transient cells are short-lived and must be continually replaced from stem cells.
- Plasma cells
- Lymphocytes
- Neutrophils
- Eosinophils
- Basophils
- Monocytes
- Macrophages* (some are fixed, some are transient)
Adipose Tissue
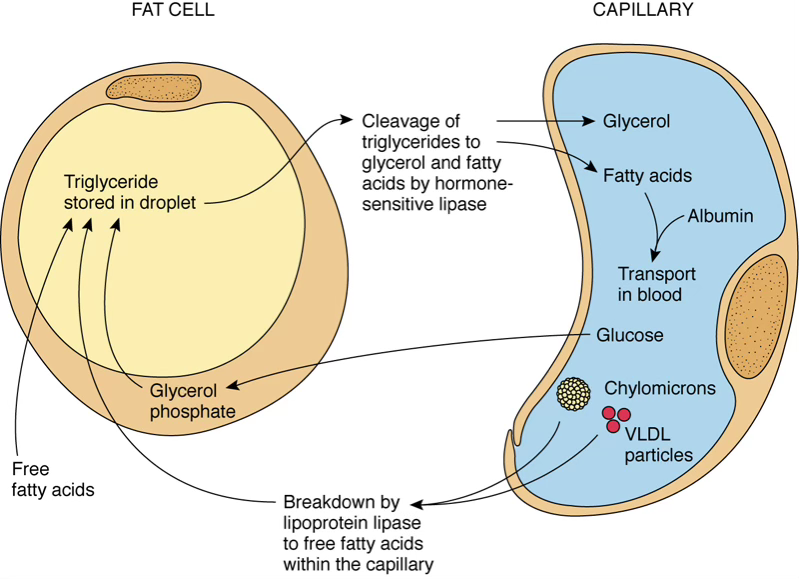
Lipid Transport
Inside the adipocyte:
On demand:
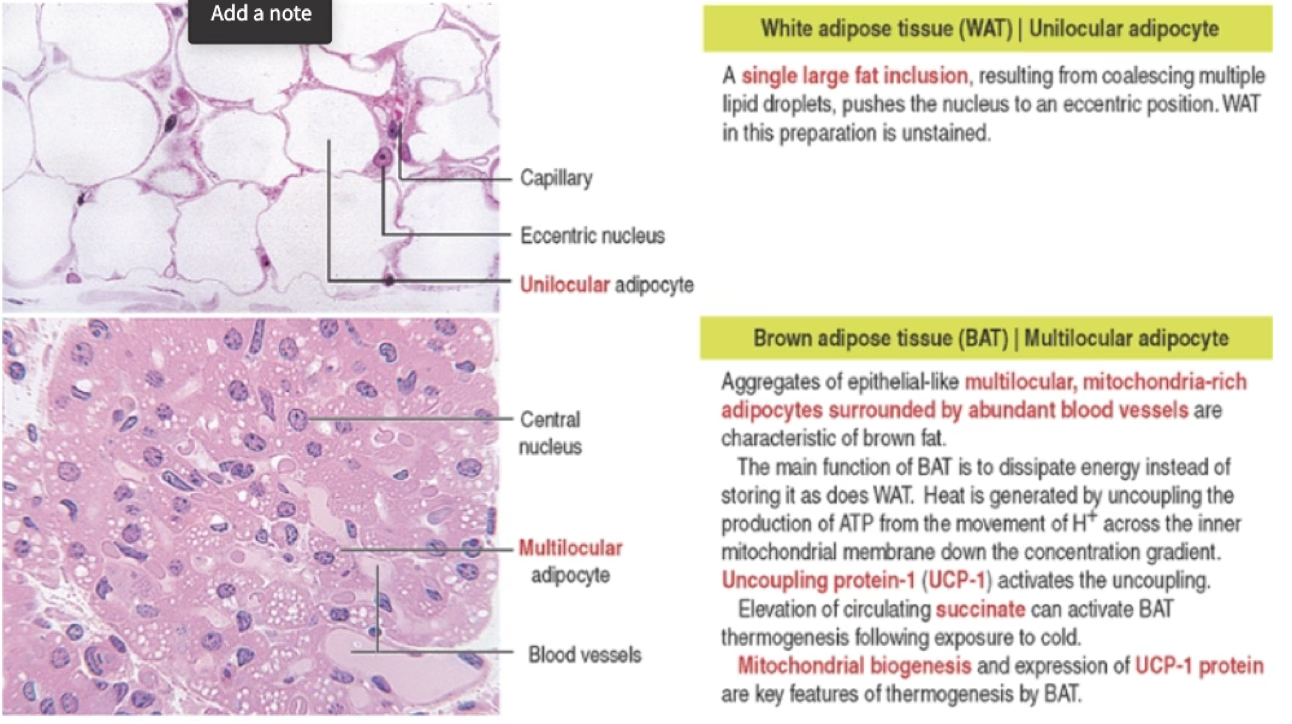
Two Types of Adipose Tissue
White vs. Brown Fat
Feature White Adipose Tissue (WAT) Brown Adipose Tissue (BAT) Droplets Single large (unilocular) Multiple small (multilocular) Nucleus Peripherally displaced Central Function Long-term energy storage; endocrine Thermogenesis; endocrine Mitochondria Few Abundant Key protein — UCP-1 (uncoupling protein-1) Abundance Very abundant Less abundant BAT dissipates energy as heat by uncoupling ATP production from H⁺ movement across the inner mitochondrial membrane (via UCP-1). Cold exposure activates BAT via circulating succinate.
Histological Visualization of Fat
- Paraffin sections: fat dissolved by xylene → empty space with a thin cytoplasmic rim
- Osmium tetroxide fixation: fat stains brown; also used for myelin
- Frozen sections + Sudan III / Sudan Black: lipid droplets stained directly
Mast Cells
Large ovoid fixed cells (), with a central spherical nucleus and membrane-bound granules.
Primary (Preformed) Mediators (from granules)
- Heparin
- Histamine
- Neutral proteases
- Aryl sulfatase
- ECF (eosinophil chemotactic factor)
- NCF (neutrophil chemotactic factor)
- Chondroitin sulfate
Secondary (Newly Synthesized) Mediators (from membrane arachidonic acid)
- Leukotrienes
- Thromboxanes
- Prostaglandins (especially )
- Various cytokines
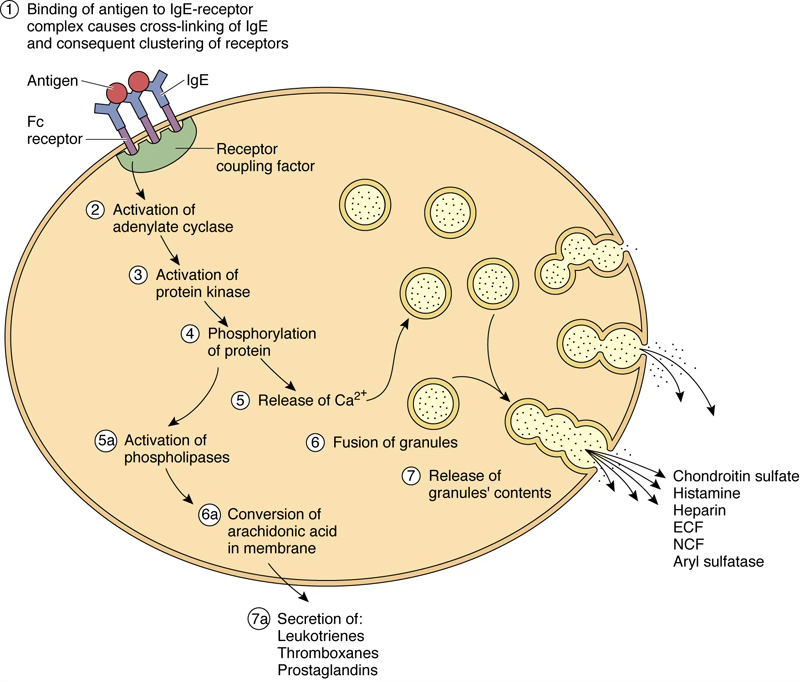
Activation Mechanism
Mast Cell Degranulation Cascade
- Antigen binds IgE already bound to surface receptors
- Cross-linking of IgE–receptor complexes
- Activation of adenylate cyclase → ↑ cAMP → protein kinase activation
- Phosphorylation events → Ca²⁺ influx
- Activation of phospholipases → arachidonic acid release
- Granule fusion with plasma membrane → release of primary mediators
- Simultaneous synthesis of secondary mediators
⚠️ Severe systemic activation → anaphylactic reaction (potentially lethal)
Plasma Cells
Derived from B lymphocytes after antigen interaction. Function: produce and secrete antibodies.
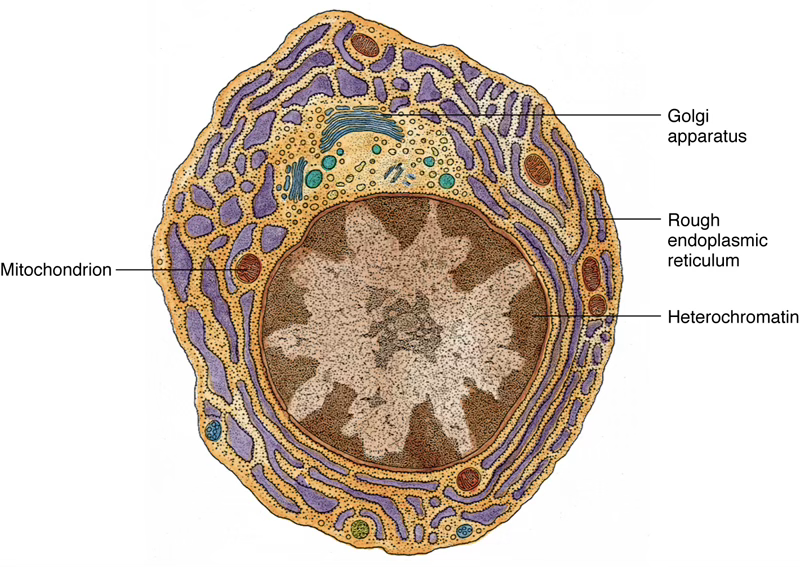
Morphology
- Large ovoid cells, diameter
- Eccentrically placed nucleus
- Characteristic “clock-face” / “spoke-wheel” chromatin pattern (heterochromatin radiates from center)
- Intensely basophilic cytoplasm (abundant RER with closely spaced cisternae)
- Large Golgi complex + centrioles visible in pale-staining perinuclear region
- Life span: 2–3 weeks
Most abundant in areas of chronic inflammation or foreign substance infiltration.
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1828/i1840/
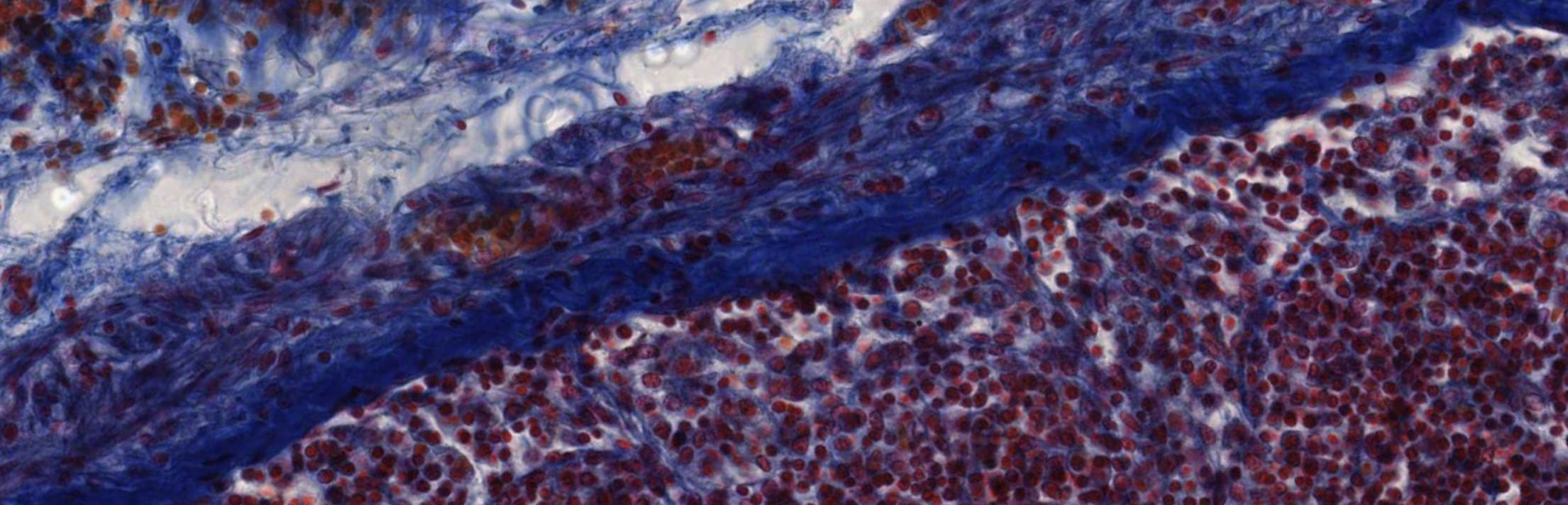
The capsule of every organ is made of dense connective tissue.
Around veins, most of the time, we have dense irregular connective tissue.
The white circles are adipocytes, while the red dots are red blood cells caused by a leakage from the vessels during the preparation of the tissue.
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1828/i1886/
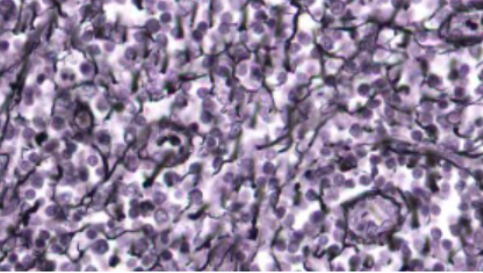
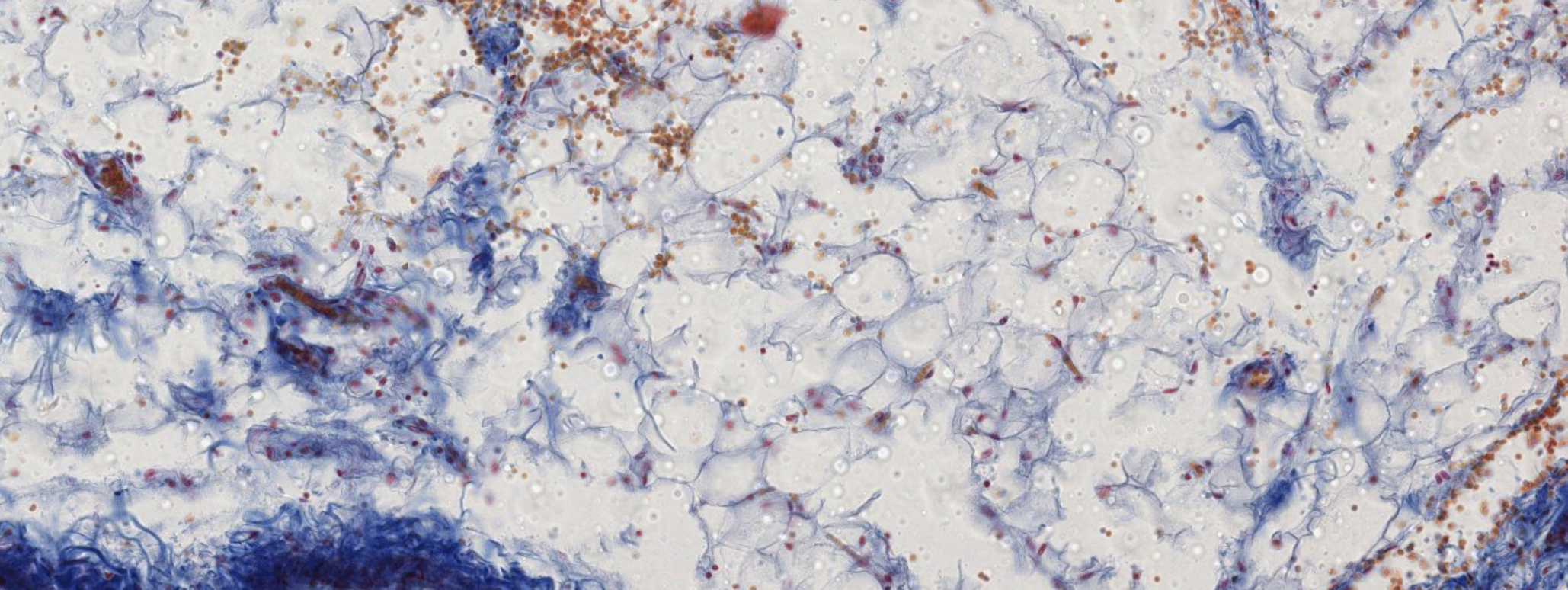
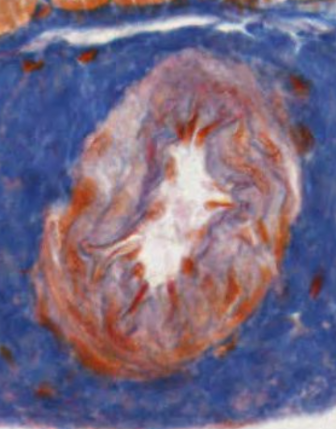
Brown adipose tissue in which the droplets of fat haven’t fused together.
Artery in which the red zig zag lines are elastic fibers, the presence of the elastic fibers allows you to tell the difference between vein and artery.
https://histologyguide.com/slideview/MH-078-lymph-node/03-slide-1.html?x=31242&y=2734&z=50.000
TLDR
Connective tissue is the body’s structural scaffolding, made of cells, fibers, and ECM (ground substance). It is broadly split into CT proper (loose, dense regular/irregular, reticular, elastic) and specialized CT (cartilage, bone, blood, adipose tissue).
The ECM is a hydrated gel of GAGs (sulfated and non-sulfated), proteoglycans (aggrecan aggregates tethered to hyaluronan), and adhesive glycoproteins (fibronectin, laminin, chondronectin, osteonectin). It resists mechanical stress.
Fibers come in three flavors: collagen (inelastic, tensile strength; ≥20 types — I in most CT, II in cartilage, III as reticulin, IV in basal lamina), reticular (type III; fine meshwork in lymphoid organs), and elastic (elastin + microfibrils; stretch to 150%; stabilized by desmosine crosslinks from lysine).
Cells are either fixed (fibroblasts, adipocytes, pericytes, mast cells, some macrophages) or transient (plasma cells, lymphocytes, neutrophils, eosinophils, basophils, monocytes, some macrophages — all bone-marrow derived).
Fat cells store triglycerides (delivered via chylomicrons/VLDLs, broken down by lipoprotein lipase) and release them via hormone-sensitive lipase activated by epinephrine → cAMP cascade. WAT (unilocular, energy storage) vastly outnumbers BAT (multilocular, thermogenesis via UCP-1).
Mast cells are the first responders of allergic/inflammatory reactions: IgE cross-linking → degranulation (histamine, heparin, ECF, NCF) + arachidonic acid–derived secondary mediators (leukotrienes, prostaglandins, thromboxanes). Extreme activation = anaphylaxis.
Plasma cells are terminally differentiated B cells with a “clock-face” nucleus, rammed with RER, that secrete antibodies. They live 2–3 weeks and accumulate at sites of chronic inflammation.
Flashcards
TARGET DECK: MED::I::Morphology and Development::Histology::06 - Connective Tissue Proper
What are the three components of connective tissue?
- Cells
- Fibers
- Extracellular matrix (ECM) / ground substance
Anki cloze
The ECM is a combination of {1:collagens}, {1:non-collagenous glycoproteins}, and {1:proteoglycans} surrounding connective tissue cells.
What are the two broad categories of connective tissue cells?
- Fixed (resident) cells: fibroblasts, adipocytes, pericytes, mast cells, some macrophages
- Transient (wandering) cells: plasma cells, lymphocytes, neutrophils, eosinophils, basophils, monocytes, some macrophages
Anki cloze
In loose CT, the cell/fiber ratio is {1:high} (cells dominate). In dense CT, the cell/fiber ratio is {1:low} (fibers dominate).
What are the subtypes of Dense CT and their examples?
- Irregular: random fiber orientation (e.g. dermis, submucosa)
- Regular: parallel fiber orientation (e.g. tendons, ligaments)
- Crossed fibers: crossed collagen (e.g. cornea)
Anki cloze
The two types of GAGs are {1:sulfated} (e.g. keratan sulfate, heparan sulfate, chondroitin sulfate) and {1:non-sulfated} (e.g. hyaluronic acid).
What is an aggrecan aggregate?
A huge macromolecule formed by proteoglycans covalently linked to hyaluronic acid via a core protein and linker protein — responsible for the gel-state of the ECM.
Match each adhesive glycoprotein to its location.
Glycoprotein Location Laminin Basal lamina Chondronectin Cartilage Osteonectin Bone Fibronectin Throughout ECM
Anki cloze
Tropocollagen consists of {1:three} -chains wrapped in a {1:triple helix}, which pack into fibrils producing a characteristic {1:67 nm} cross-banding pattern in type I collagen.
What are the major collagen types and their locations?
Type Location I CT proper, bone, dentin, cementum II Hyaline & elastic cartilage III Reticular fibers; stroma of lymphoid organs & liver IV Lamina densa of basal lamina (no 67 nm periodicity) VII Anchoring fibrils (basal lamina → lamina reticularis)
Anki cloze
Elastic fibers consist of an amorphous {1:elastin} core surrounded by peripheral {1:microfibrils}. They can stretch to {1:150%} of resting length without breaking.
Anki cloze
In elastin, {1:lysine} residues form {1:desmosine} crosslinks, which are responsible for the high elasticity of elastic fibers.
What is the lipolysis signaling cascade in adipocytes?
Compare White Adipose Tissue (WAT) vs. Brown Adipose Tissue (BAT).
Feature WAT BAT Droplets Unilocular (single large) Multilocular (multiple small) Nucleus Peripherally displaced Central Function Energy storage; endocrine Thermogenesis; endocrine Mitochondria Few Abundant Key protein — UCP-1
Anki cloze
BAT produces heat by {1:uncoupling} ATP production from H⁺ movement across the inner mitochondrial membrane via {1:UCP-1}. Cold exposure activates BAT via circulating {1:succinate}.
How is fat visualized histologically?
- Paraffin sections: fat dissolved by xylene → empty space with thin cytoplasmic rim
- Osmium tetroxide: fat stains brown (also used for myelin)
- Frozen sections + Sudan III / Sudan Black: lipid droplets stained directly
What are the primary (preformed) mediators released by mast cell granules?
- Heparin
- Histamine
- Neutral proteases
- Aryl sulfatase
- ECF (eosinophil chemotactic factor)
- NCF (neutrophil chemotactic factor)
- Chondroitin sulfate
What are the secondary (newly synthesized) mediators of mast cells?
Derived from membrane arachidonic acid:
- Leukotrienes
- Thromboxanes
- Prostaglandins (especially )
- Various cytokines
Anki cloze
Mast cell degranulation is triggered when antigen binds {1:IgE} already attached to surface receptors, causing cross-linking → activation of adenylate cyclase → {1:cAMP} → protein kinase activation → {1:Ca²⁺} influx → granule fusion and release of primary mediators.
Anki cloze
Severe systemic mast cell activation leads to an {1:anaphylactic} reaction, which can be potentially lethal.
What is the morphology of a plasma cell?
- Large ovoid, diameter
- Eccentrically placed nucleus
- “Clock-face” / “spoke-wheel” chromatin pattern
- Intensely basophilic cytoplasm (abundant RER)
- Large Golgi complex in pale perinuclear region
- Life span: 2–3 weeks
Anki cloze
Plasma cells are derived from {1:B lymphocytes} after antigen interaction and function to {1:produce and secrete antibodies}. They are most abundant in areas of {1:chronic inflammation}.
Anki cloze
Reticular fibers are composed of type {1:III} collagen and form a fine meshwork (stroma) in {1:lymph nodes}, {1:spleen}, hematopoietic bone marrow, and {1:liver}.