TARGET DECK: MED::I::Morphology and Development::Histology::08 - Cartilage
Overview
Cartilage possesses cells: chondrocytes, which occupy small cavities called lacunae, within the extracellular matrix they secreted.
Avascular
Tissue The cartilage is neither vascularized nor supplied with nerves or lymphatic vessels; however, the cells receive their nourishment from blood vessels of surrounding connective tissues by diffusion through the matrix.
The extracellular matrix is composed of glycosaminoglycans and proteoglycans, which are intimately associated with the collagen and elastic fibers embedded in the matrix.
The flexibility and resistance of cartilage to compression permit it to function as a shock absorber, and its smooth surface permits almost friction-free movement of the joints of the body as it covers the articulating surfaces of the bones.
What type of tissue is cartilage regarding vascularization?
Cartilage is avascular, aneural, and alymphatic. Nutrients reach chondrocytes by diffusion through the extracellular matrix from surrounding connective tissue blood vessels.
Anki cloze
Chondrocytes occupy small cavities called {1:lacunae} within the extracellular matrix they secreted.
Types of Cartilage
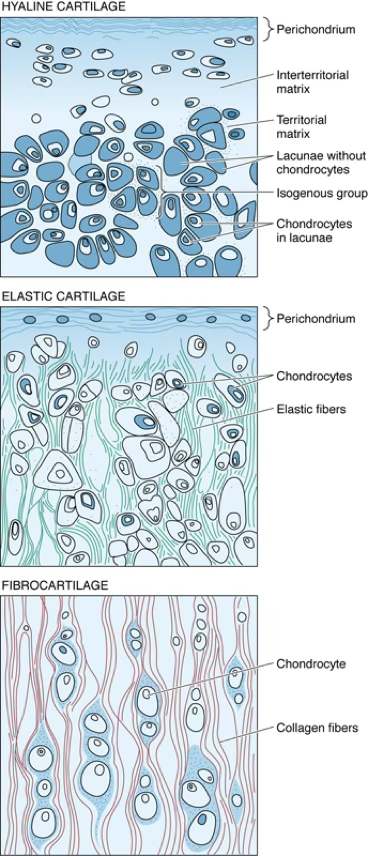
| Type | Main Collagen | Key Feature | Perichondrium | Calcifies? |
|---|---|---|---|---|
| Hyaline | Type II | Most abundant; glassy appearance | Yes (except articular cartilage & epiphyseal plates) | Yes (e.g., endochondral ossification, aging) |
| Elastic | Type II + elastic fibers | More pliable; abundant elastic fibers | Yes | No |
| Fibrocartilage | Type I (dense, coarse) | Withstands strong tensile forces; no perichondrium | No | Yes (e.g., fibrocartilaginous callus in bone repair) |
Mnemonic — Cartilage Types "HEF" — Hyaline, Elastic, Fibro
- Hyaline = Highly abundant, Hyalos (glass)
- Elastic = Ears and Epiglottis
- Fibro = Force-bearing (intervertebral discs, pubic symphysis)
Anki cloze
Hyaline cartilage contains {1:type II} collagen; elastic cartilage contains {1:type II} collagen plus abundant {1:elastic fibers}; fibrocartilage contains dense {1:type I} collagen fibers.
Hyaline Cartilage
General Characteristics
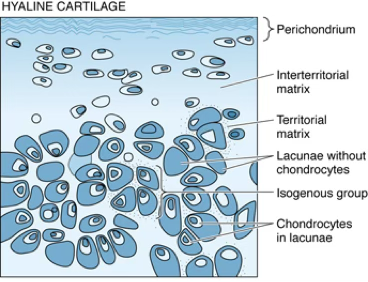
- Hyaline cartilage is the most widespread cartilage in humans.
- Its name derives from the clear appearance of the matrix (Greek hyalos, glass).
- Appearance: glassy, blue/grey, transparent/translucent.
- It is the most abundant, located in the nose, larynx, tracheal rings, ventral end of the ribs.
Articular Cartilage — Special Case
The articular surface of synovial joints (knees, shoulders) is hyaline cartilage and does not participate in endochondral ossification. Articular surfaces are not lined by an epithelium/perichondrium.
Development (Fetal and Adult)
- In the fetus, hyaline cartilage forms most of the skeleton before it is reabsorbed and replaced by bone by a process known as endochondral ossification.
- In adults, hyaline cartilage persists as the nasal, laryngeal, tracheobronchial, and costal cartilage.
- Forms the cartilage template for the long bones during embryonic development.
Where does hyaline cartilage persist in adults?
In adults, hyaline cartilage persists as the nasal, laryngeal, tracheobronchial, and costal cartilages, and as the articular surfaces of synovial joints.
Hyaline Cartilage — Histogenesis
- Differentiate from mesenchymal cells, that retract their processes and round up, forming the chondrification centers.
- Differentiate into chondroblasts and secrete collagen II and aggrecan (matrix) → lacunae chondrocytes, which upon few divisions give rise to isogenous groups.
- Interstitial growth occurs.
- Mesenchymal cells at the periphery differentiate into fibroblasts, producing dense irregular connective tissue (perichondrium).
Anki cloze
During hyaline cartilage histogenesis, mesenchymal cells form {1:chondrification centers}, then differentiate into {1:chondroblasts}, which secrete {1:collagen II} and {1:aggrecan}, eventually forming isogenous groups within lacunae.
Perichondrium
Responsible for the growth and maintenance of the cartilage.
- Outer fibrous layer: fibroblasts, Collagen I, and blood vessels.
- Inner layer (chondrogenic layer): chondrogenic cells that undergo division and differentiation to chondroblasts, which deposit matrix to the periphery → (appositional growth).
Two Layers of Perichondrium
Layer Cells Contents Function Outer fibrous Fibroblasts Collagen I, blood vessels Structural support, nutrition Inner chondrogenic Chondrogenic cells → Chondroblasts — Appositional growth
What are the two layers of the perichondrium and their functions?
Outer fibrous layer: fibroblasts, Collagen I, blood vessels — structural/nutritional support. Inner chondrogenic layer: chondrogenic cells → chondroblasts, responsible for appositional growth by depositing matrix peripherally.
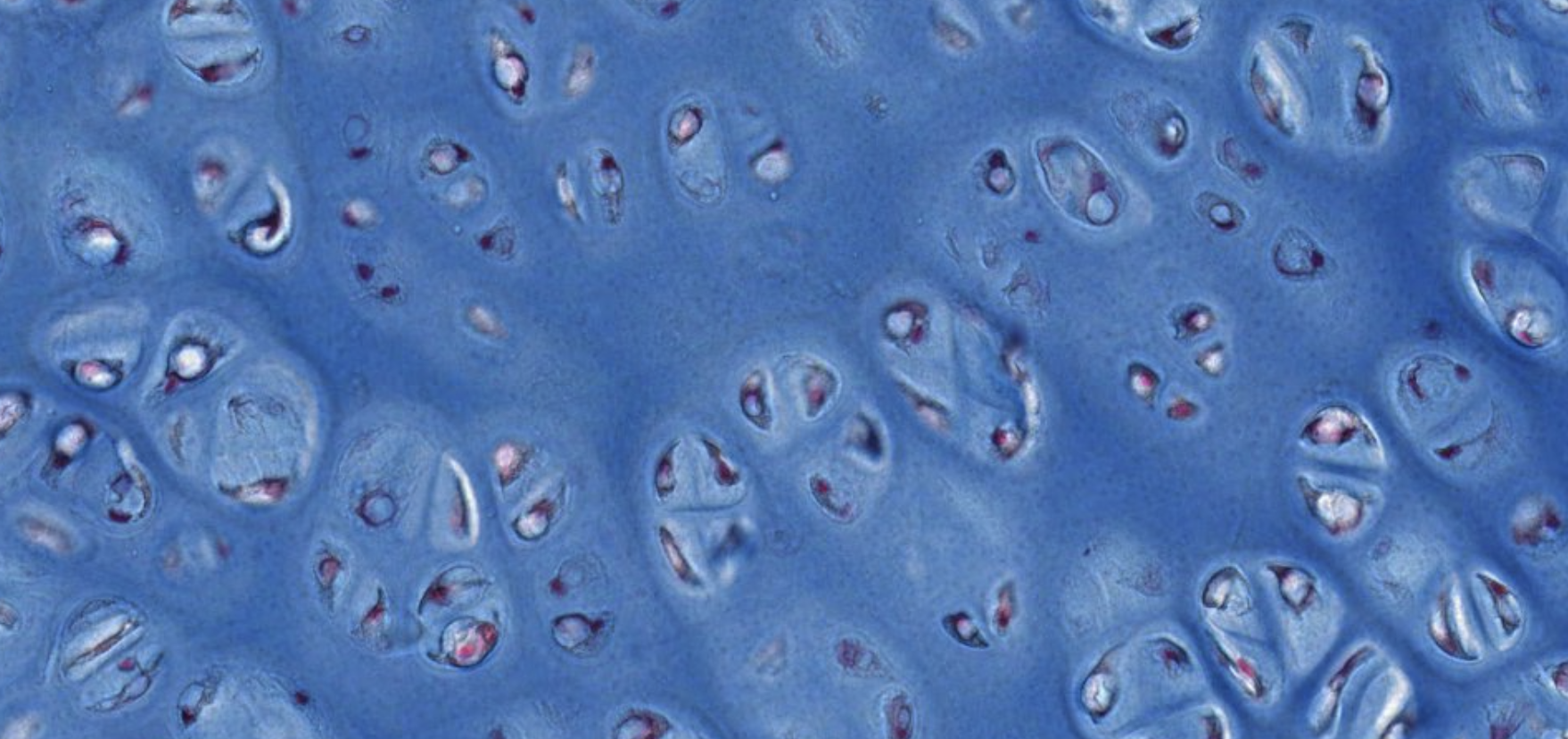
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1841/i1842/
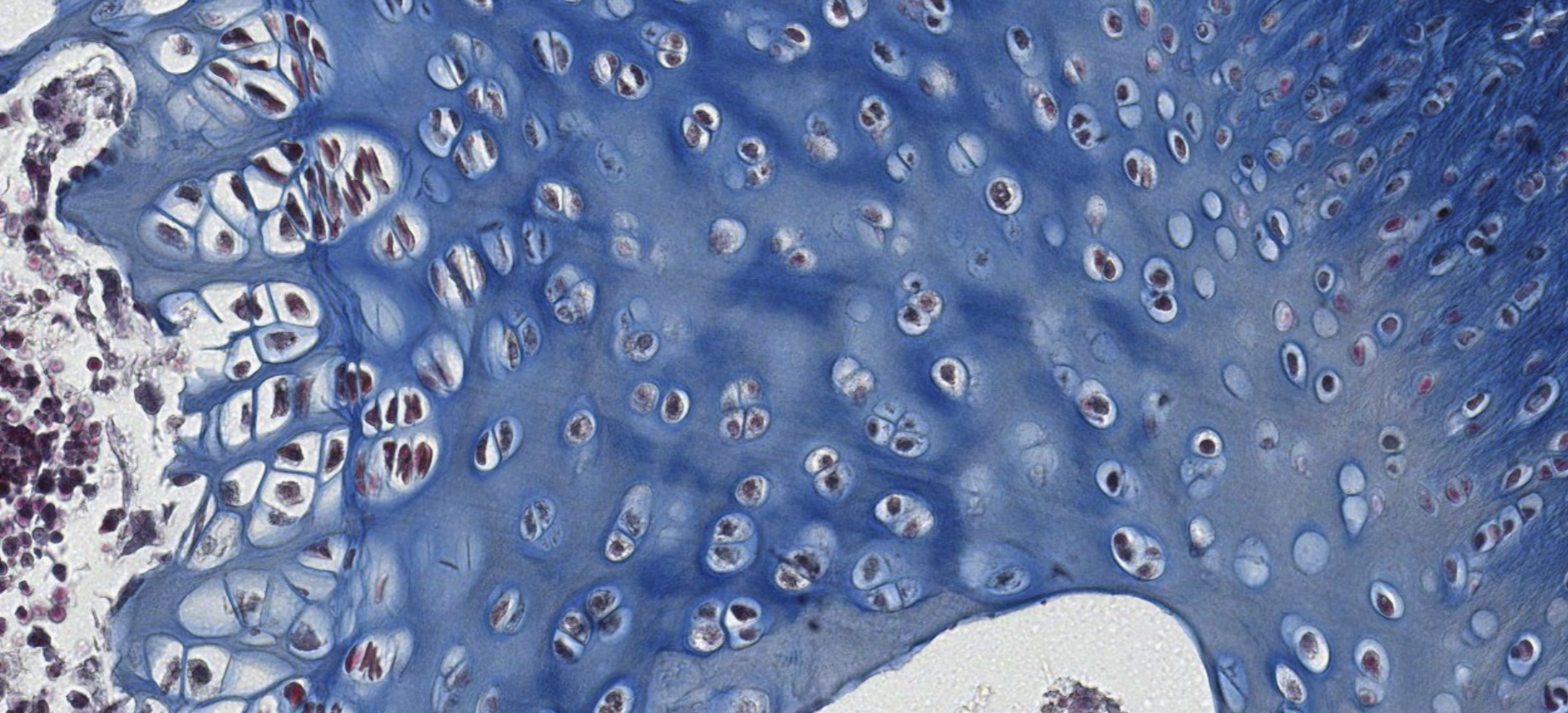
These chondroblasts belong to the same lacune because soon after the proliferation ? the chondroblasts remain trapped. Territorial Matrix is located inside the lacuna.
The ones that look more white are chondrocytes.
In order to increase the size of the cartialge we need to increase the number of chondroblasts.
This is called interstitial growth.
Here we find the reserve of stem cells.
These are chondroblast precursors, which will receive the signals to start dividing and differentiating into chondroblasts and secreting the matrix.
This is apositional growth, different from intestitial.
The only way to repair the cartilage is through the pericordium.
In the joints, for example, where there is the need to move, there is no fibrous pericordium, so the cartilage reparation ability is highly hindered
Cartilage Cells — 3 Types
- Chondrogenic cells (precursors): spindle-shaped cells derived from mesenchymal cells (can differentiate into Chondroblasts/Chondrocytes).
- Chondroblasts: derived directly from mesenchymal cells or from chondrogenic cells of the inner layer of perichondrium (as in appositional growth) — basophilic cells. Note: interstitial growth happens only in the early phase of development.
- Chondrocytes: chondroblasts surrounded by matrix; ovoid in the periphery and rounded deeper in the cartilage (–).
Anki cloze
The three types of cartilage cells are: {1:chondrogenic cells} (precursors), {1:chondroblasts} (active secretors), and {1:chondrocytes} (mature, embedded in matrix).
Matrix of Hyaline Cartilage
- Type II collagen, about
- Proteoglycan aggregates
- Glycoproteins
- Extracellular fluid
Matrix Zones
| Zone | Location | Collagen Content | Proteoglycan Content | |
|---|---|---|---|---|
| Territorial matrix | Around each lacuna | Poor | Rich | 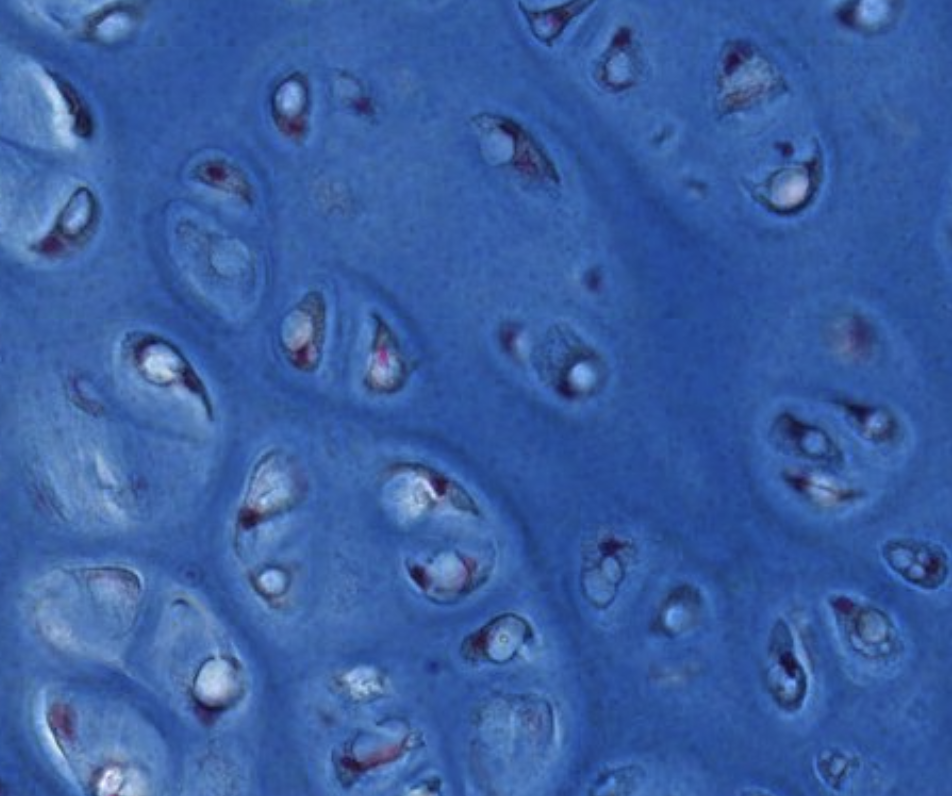 Lighter stained appearance, inside the lacune. Lighter stained appearance, inside the lacune. |
| Inter-territorial matrix | Between lacunae | Rich | Poor | |
| Pericellular capsule | Immediately surrounding each lacuna | — | — | 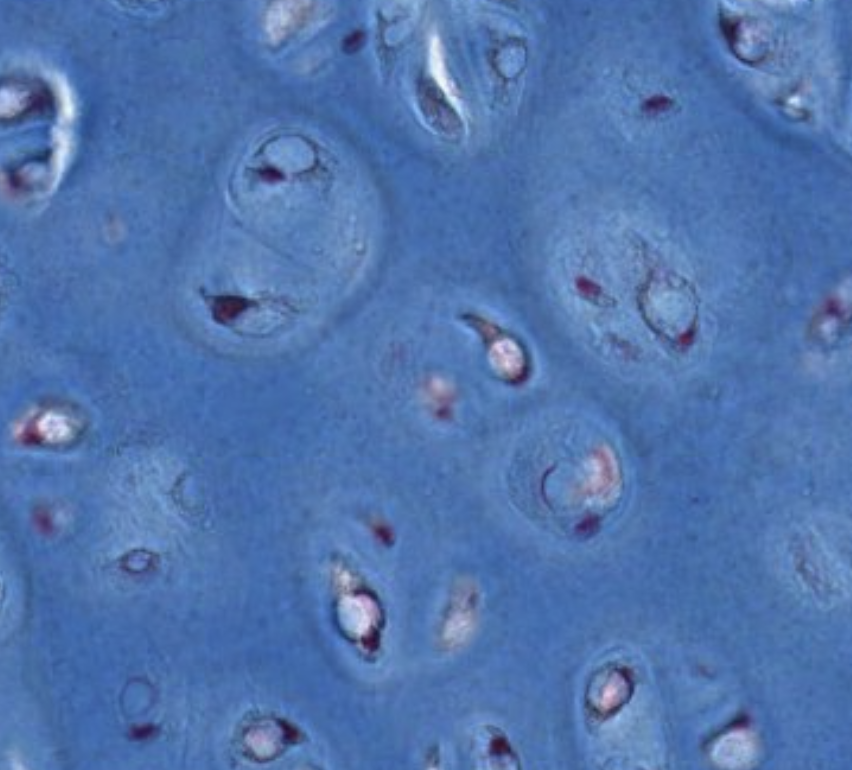 Very clear in certain parts. |
Anki cloze
The territorial matrix is {1:rich} in proteoglycans and {1:poor} in collagen, while the inter-territorial matrix is {1:rich} in collagen and {1:poor} in proteoglycans.
Histopathology
- In cartilage, chondroblasts and chondrocytes are sustained by diffusion of nutrients and metabolites through the aqueous phase of the extracellular matrix.
- At all ages, chondrocytes have significant nutritional requirements, but their metabolic rate is low.
Cartilage Repair After Injury
Limited Repair Capacity
Cartilage has a modest capacity of chondrogenesis (cartilage growth).
- Cartilage injuries result in the formation of repair cartilage from the perichondrium.
- This repair cartilage contains undifferentiated cells with a potential to differentiate into chondrocytes that synthesize components of the cartilage matrix. This important property facilitates the healing of a bone fracture.
- The repair cartilage has a matrix composition intermediate between hyaline and fibrous cartilage (for example, it contains both types I and II collagen).
What is the collagen composition of repair cartilage?
Repair cartilage has a matrix composition intermediate between hyaline and fibrous cartilage, containing both type I and type II collagen.
Chondrogenesis
Cartilage grows by two mechanisms:
1. Interstitial Growth
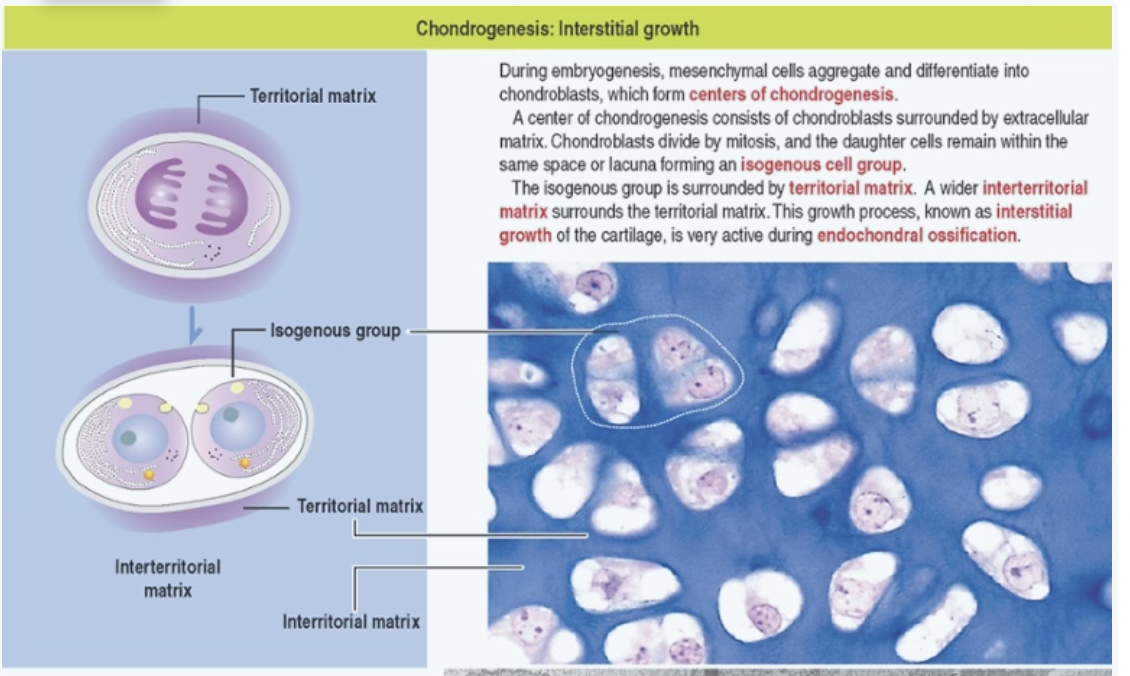
- From chondrocytes within the cartilage (inside lacunae) — early in development.
- During embryogenesis, mesenchymal cells aggregate and differentiate into chondroblasts, which form centers of chondrogenesis.
- A center of chondrogenesis consists of chondroblasts surrounded by extracellular matrix.
- Chondroblasts divide by mitosis, and the daughter cells remain within the same space or lacuna forming an isogenous cell group.
- The isogenous group is surrounded by territorial matrix; a wider interterritorial matrix surrounds the territorial matrix.
- This growth process is very active during endochondral ossification.
2. Appositional Growth
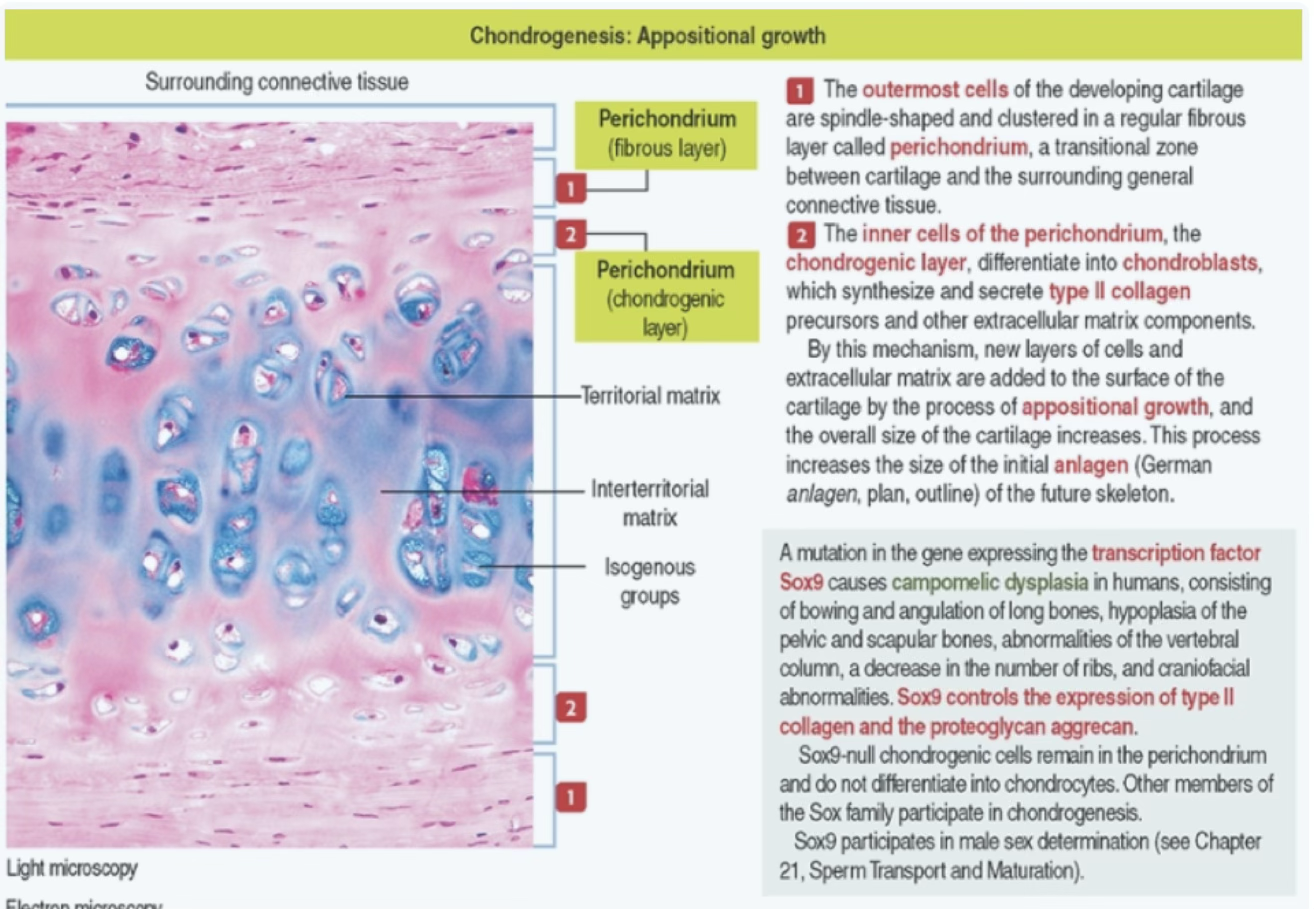
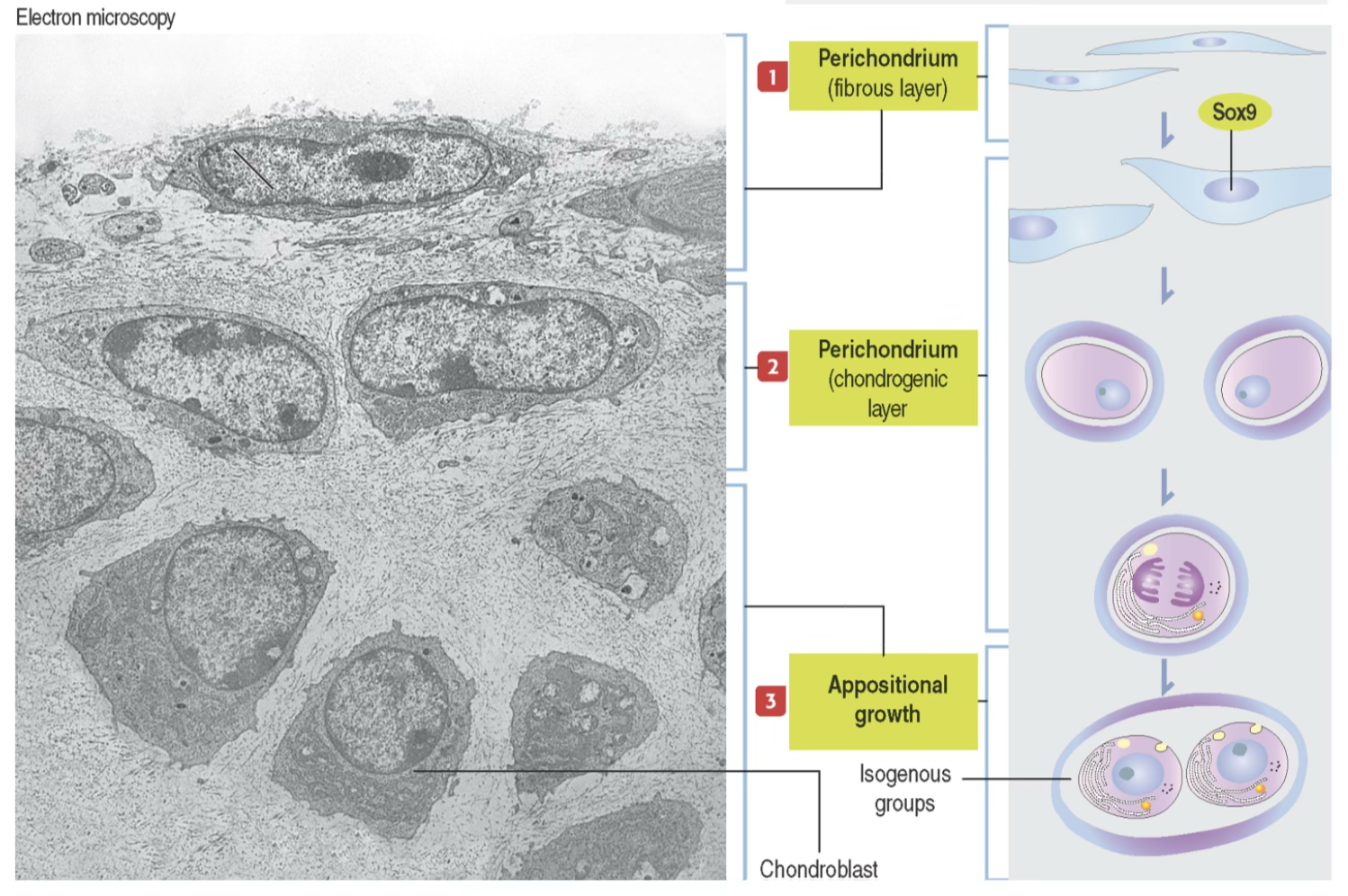
- From undifferentiated cells at the surface of the cartilage, the perichondrium.
- The outermost cells of the developing cartilage are spindle-shaped and clustered in a regular fibrous layer called perichondrium, a transitional zone between cartilage and the surrounding general connective tissue.
- The inner cells of the perichondrium (chondrogenic layer) differentiate into chondroblasts, which synthesize and secrete type II collagen precursors and other extracellular matrix components.
- By this mechanism, new layers of cells and extracellular matrix are added to the surface of the cartilage, and the overall size of the cartilage increases.
Mnemonic — Growth Mechanisms "I Am Growing"
- Interstitial = Inside (early, embryonic)
- Appositional = Added at the surface (via perichondrium)
What are the two mechanisms of cartilage growth?
- Interstitial growth: from chondrocytes within lacunae (active early in development/endochondral ossification).
- Appositional growth: from chondrogenic cells of the inner perichondrium layer, adding new layers to the surface.
Chondrogenesis: Formation of Chondrocytes
Chondrogenesis Definition
Chondrogenesis is the earliest phase of skeletal development, involving mesenchymal cell condensation and chondroprogenitor cell differentiation and maturation, resulting in the formation of cartilage.
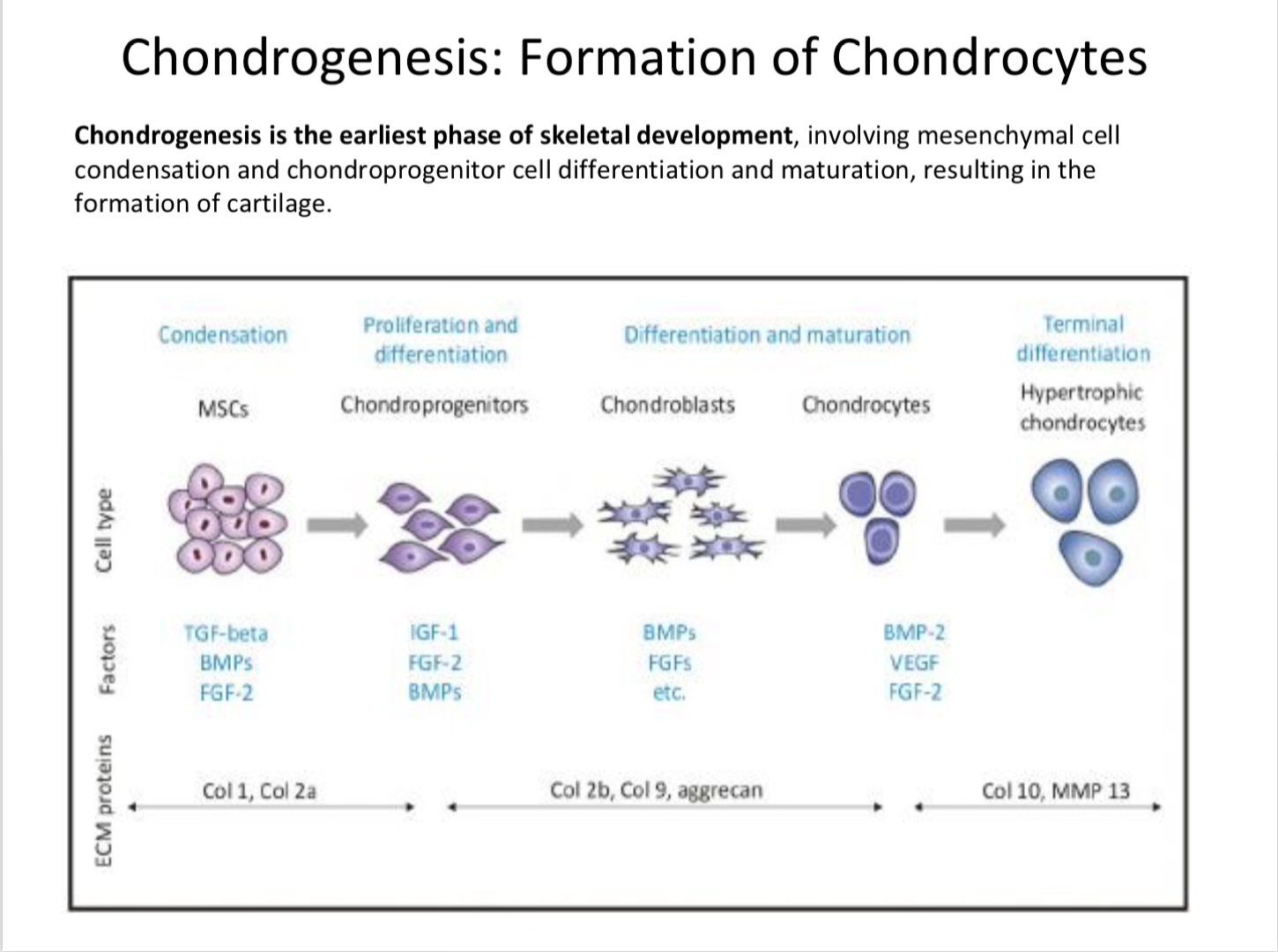
Cellular Progression
Key Factors and ECM at Each Stage
| Stage | Key Factors | ECM Proteins |
|---|---|---|
| Condensation (MSCs) | TGF-β, BMPs, FGF-2 | Col 1, Col 2a |
| Proliferation & Differentiation (Chondroprogenitors) | IGF-1, FGF-2, BMPs | Col 2b, Col 9, aggrecan |
| Differentiation & Maturation (Chondroblasts) | BMPs, FGFs, FGF-2 | Col 2b, Col 9, aggrecan |
| Terminal Differentiation (Chondrocytes → Hypertrophic) | BMP-2, VEGF | Col 10, MMP 13 |
Anki cloze
Chondrogenesis is the earliest phase of skeletal development and involves {1:mesenchymal cell condensation} and chondroprogenitor cell differentiation and maturation.
Chondrogenesis: Two Interdependent Processes
Cell Fate Determination
Cell fate determination is the process by which the combinatorial interactions of genetic and environmental factors serve to direct the developmental progression of a cell lineage. Cell fate is progressively restricted, and tissue specificity is gradually committed.
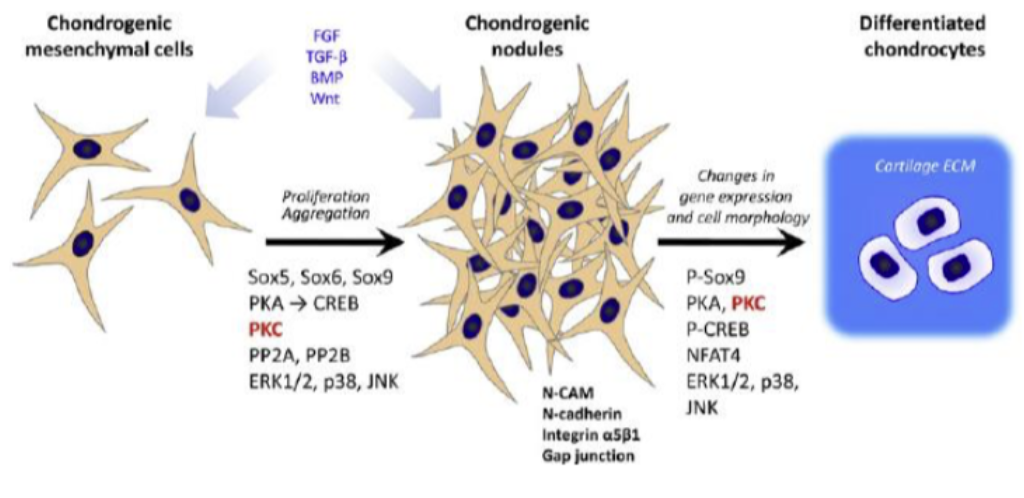
Pattern Formation
Pattern formation is the process during which number, size, and shape of the cartilaginous template is delineated and established.
Key Molecular Signals
| Step | Signals/Factors |
|---|---|
| Proliferation, Aggregation | Sox5, Sox6, Sox9; PKA → CREB; ERK1/2, p38, JNK; N-cadherin; integrin α5β1; Gap junction |
| P-Sox9 activation | PKA, PKC, PP2A, PP2B, NFAT4 |
| Further differentiation | ERK1/2, p38, JNK; loses mesenchyme character; steroids |
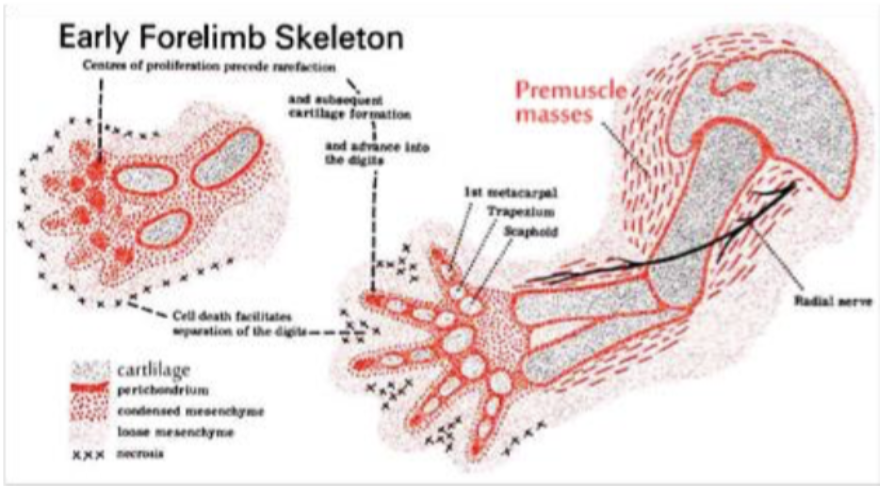
Chondrogenesis: Step 1 — MSC Condensation
- Chondroprogenitor mesenchymal cells aggregate into a mass of cells called a CHONDROGENIC NODULE, following FGF and Bone Morphogenic Protein (BMP) signaling.
- Condensation is signaled by changes in cell adhesion and cytoskeletal architecture as well as by the cell’s response to growth and differentiation factors in the extracellular environment.
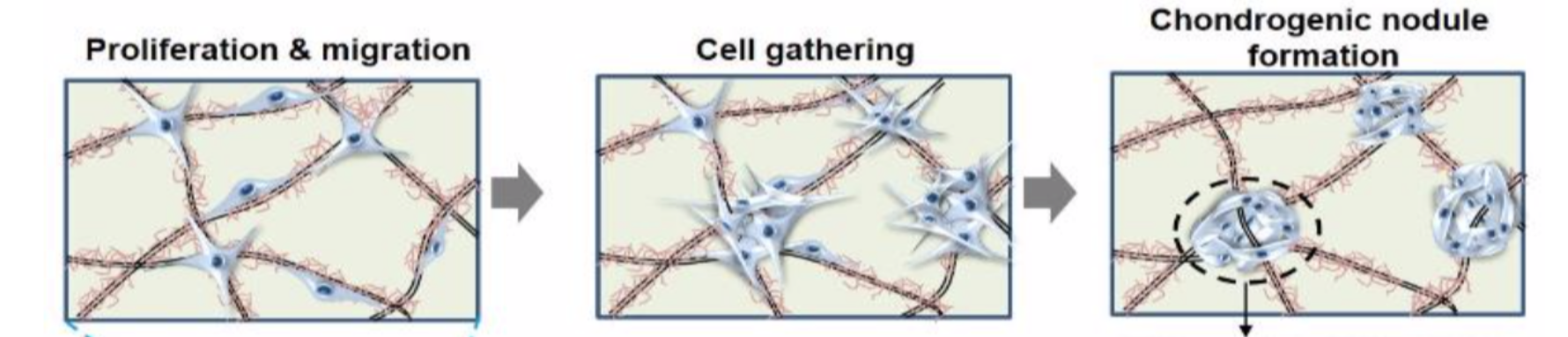
What signals drive MSC condensation into a chondrogenic nodule?
Condensation is driven by FGF and Bone Morphogenic Protein (BMP) signaling, and involves changes in cell adhesion and cytoskeletal architecture in response to extracellular growth and differentiation factors.
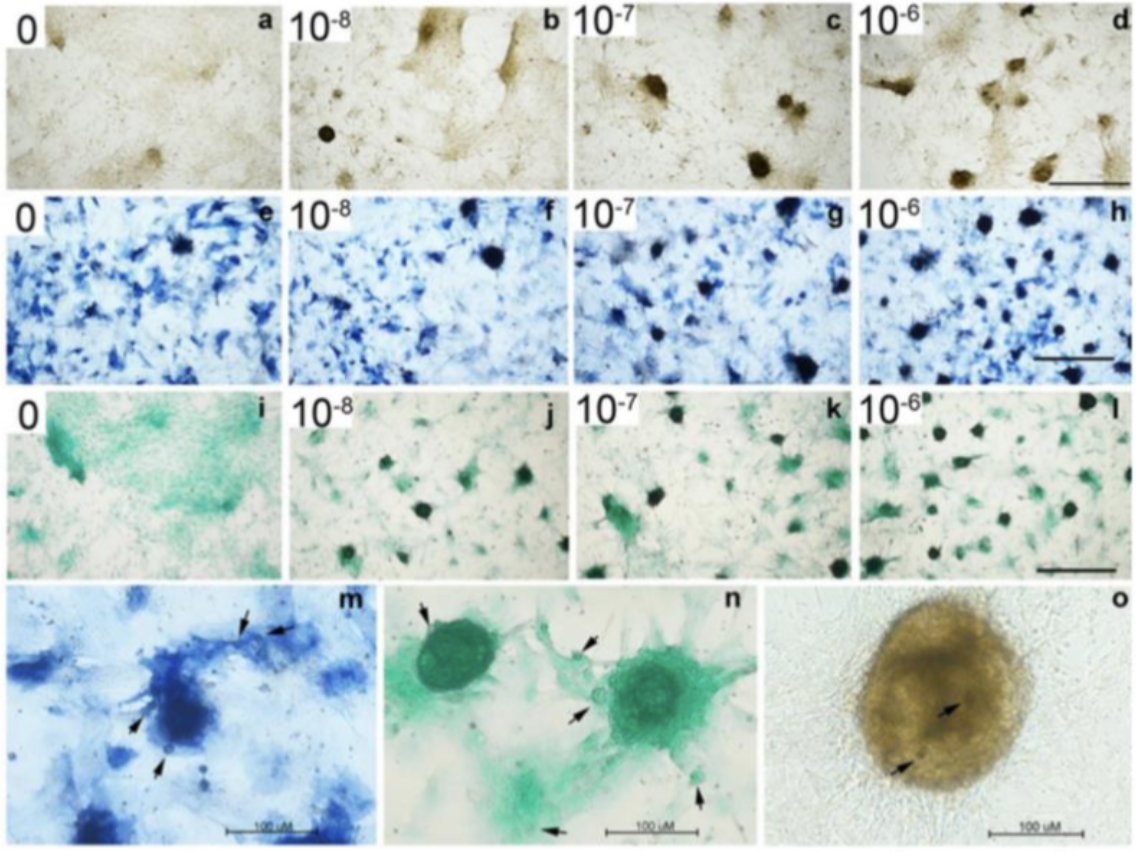
Chondrogenesis: From Chondrogenic Nodule to Chondrocyte
- Expression of transcription factor Sox-9 triggers differentiation of the nodule into chondroblasts.
- Chondroblasts with euchromatic nuclei, stained by basic dyes, secrete cartilage ECM components like aggrecan and Collagen II and progressively move apart as matrix is deposited.
- When completely surrounded by matrix, the cells undergo terminal differentiation into chondrocytes, distributed either singularly or as isogenous groups of 4 cells, displaying extensive rER and Golgi due to secretion of ground substance.
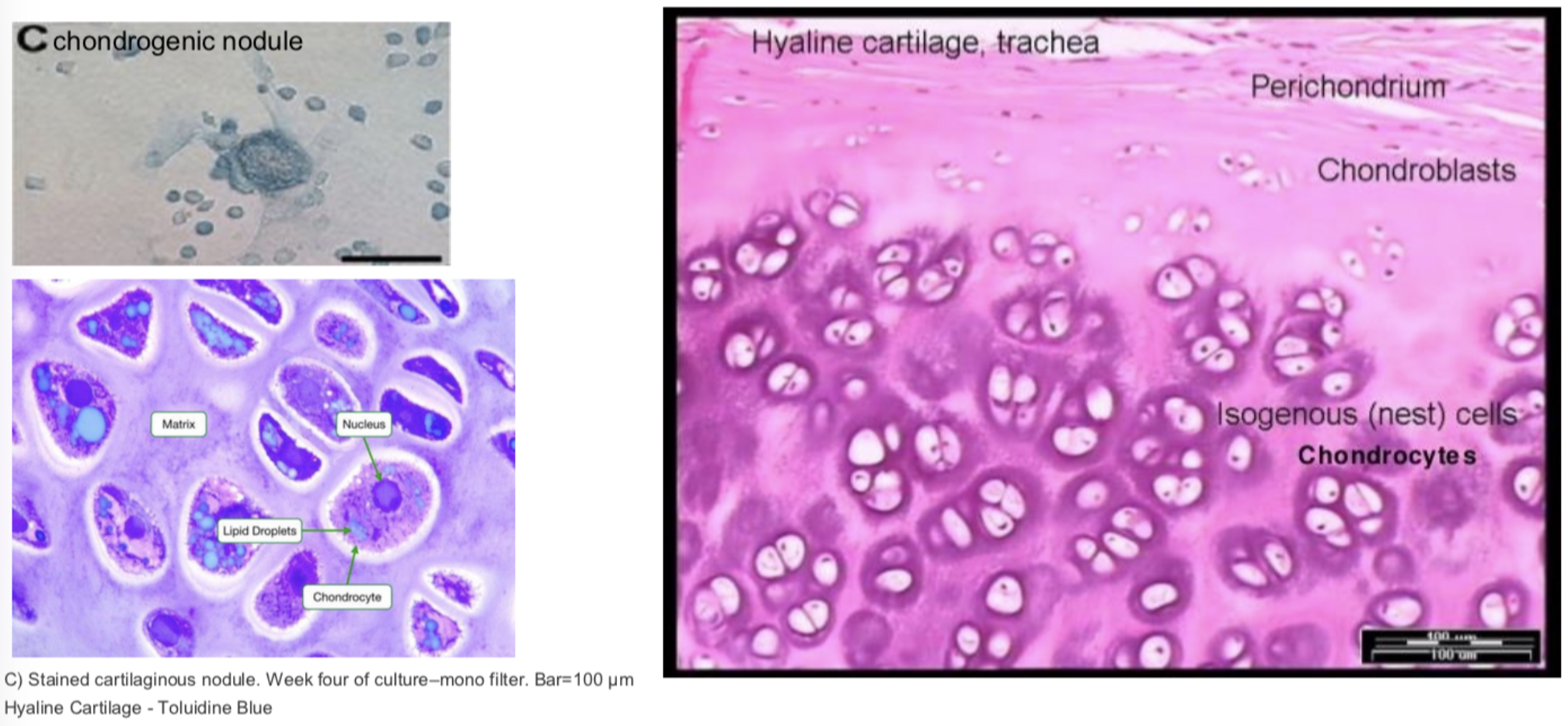
Anki cloze
The transcription factor {1:Sox-9} triggers differentiation of the chondrogenic nodule into chondroblasts.
Anki cloze
When chondroblasts are completely surrounded by matrix, they undergo terminal differentiation into {1:chondrocytes}, distributed as isogenous groups of {1:4} cells, with extensive {1:rER} and {1:Golgi}.
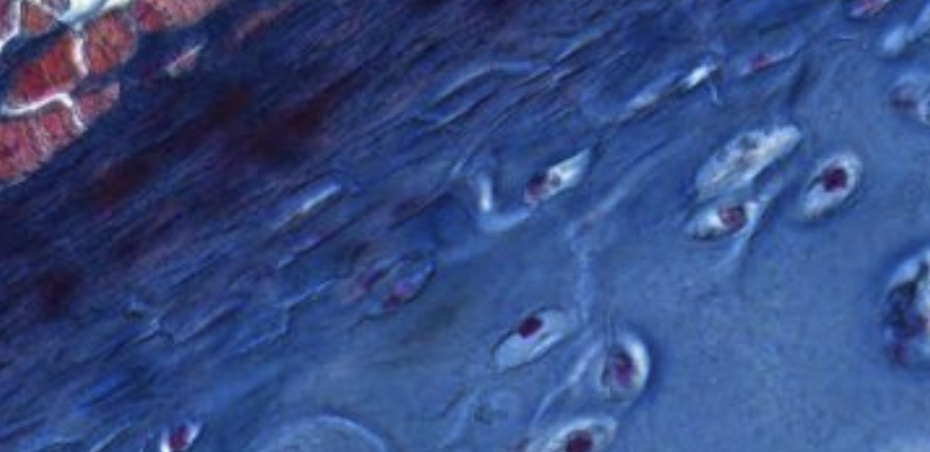
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1828/i1829/
Elastic Cartilage
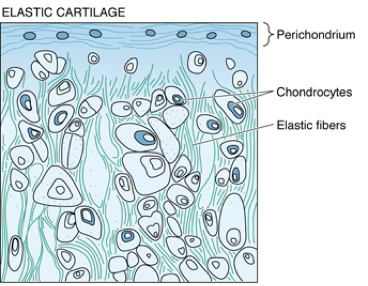
- The structure of the elastic cartilage is similar to that of hyaline cartilage except that the ECM contains abundant elastic fibers synthesized by chondrocytes.
- Elastic cartilage predominates in the auricle of the external ear, a major portion of the epiglottis, and some of the laryngeal cartilages.
Where is elastic cartilage found?
Elastic cartilage is found in the auricle of the external ear, a major portion of the epiglottis, and some of the laryngeal cartilages.
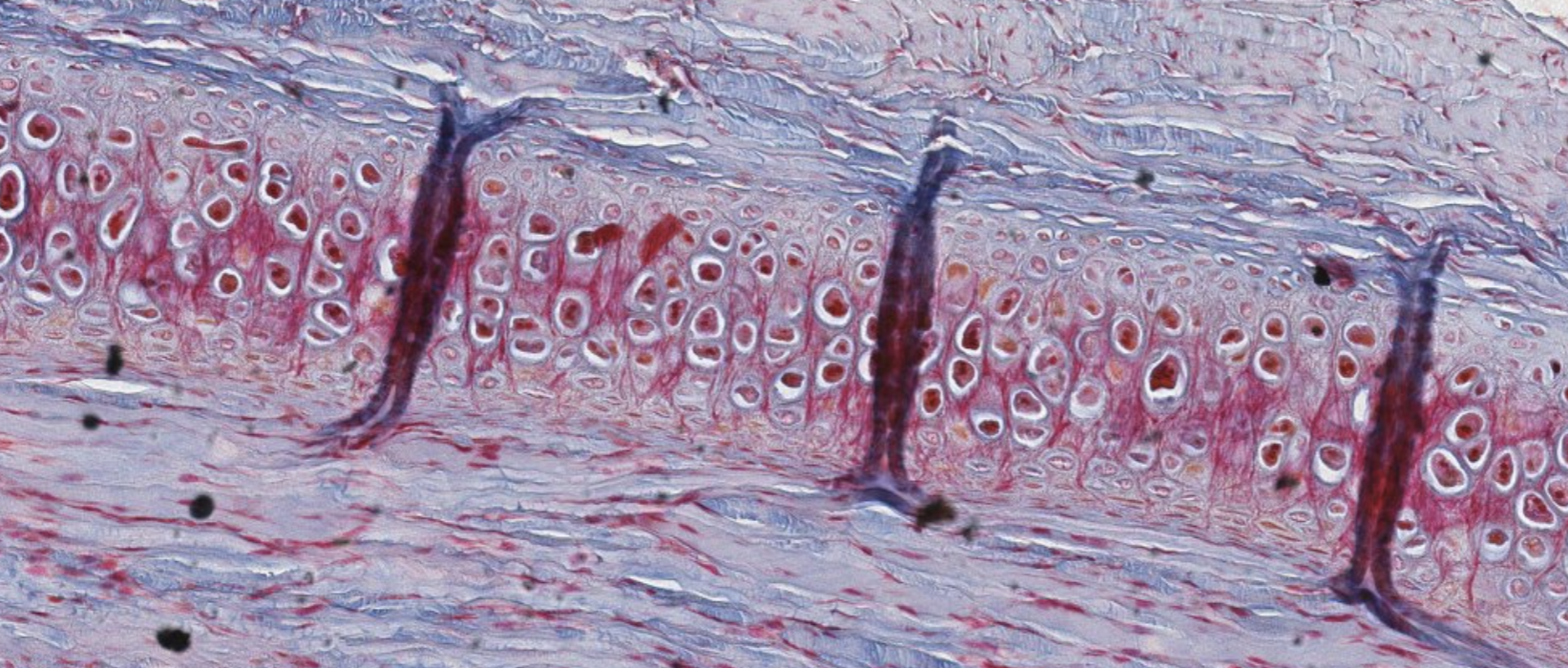
Classifying… https://unibo.smartzoom.com/s1241/course1776/f1841/i1843/
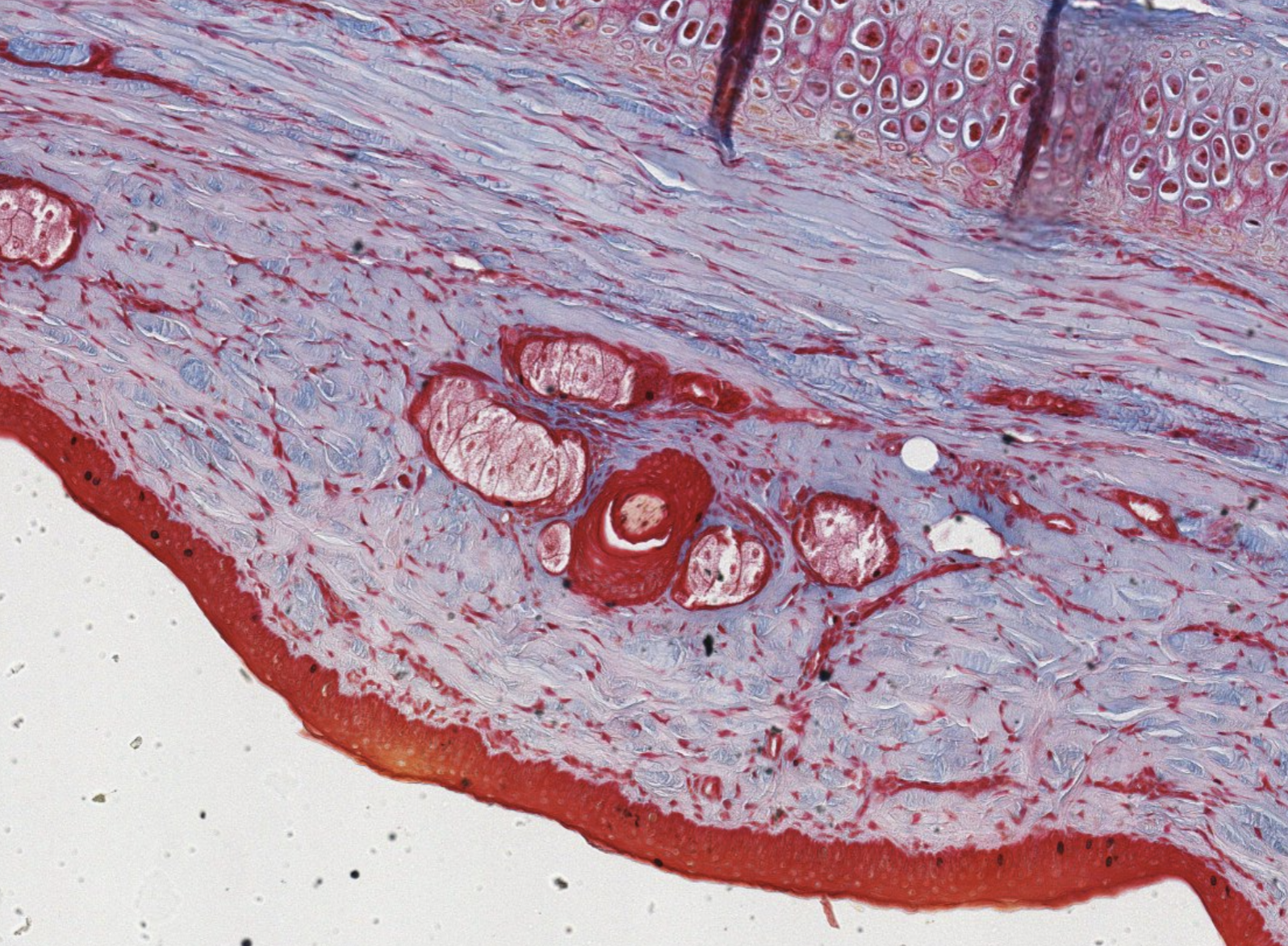
We can clearly see the pericondrium.
The major marker here is the presence of the elastic fibres, very visible as pink stained in the center of the capsules.
What are these vertical gray strands? These are artifacts of slide preparation. These happen only for the elastic cartilage, it’s a folding of the tissue itself, since it’s not able to be stretched (?)
WTF is down here? Glandular epithelia? Dense connective?
Surely something is glandular. Exocrine since the big red things have ducts in the middle.
The parts with the lil red borders are the glandular part. Acinar/alveolar in the secreting parts (?). Branched!
Fibrocartilage
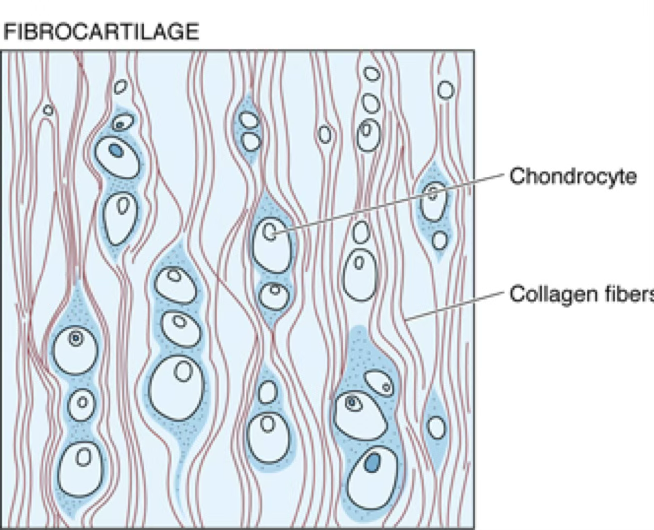
- Opaque matrix; contains type I collagen fibers.
- ECM has a low concentration of proteoglycans and water.
- Lacks a perichondrium.
- Has great tensile strength.
- Forms part of the intervertebral disc, pubic symphysis, and sites of insertion of tendon and ligament into bone.
- Sometimes difficult to distinguish from dense regular connective tissue of some regions of tendons and ligaments.
- Fibrocartilage is recognized by characteristic chondrocytes within lacunae, forming short columns.
Distinguishing Fibrocartilage
Fibrocartilage can be difficult to distinguish from dense regular connective tissue of tendons/ligaments.
The key distinguishing feature is the presence of chondrocytes within lacunae forming short columns.
What are the locations of fibrocartilage in the body?
Fibrocartilage forms part of the intervertebral disc, pubic symphysis, and sites of insertion of tendon and ligament into bone.
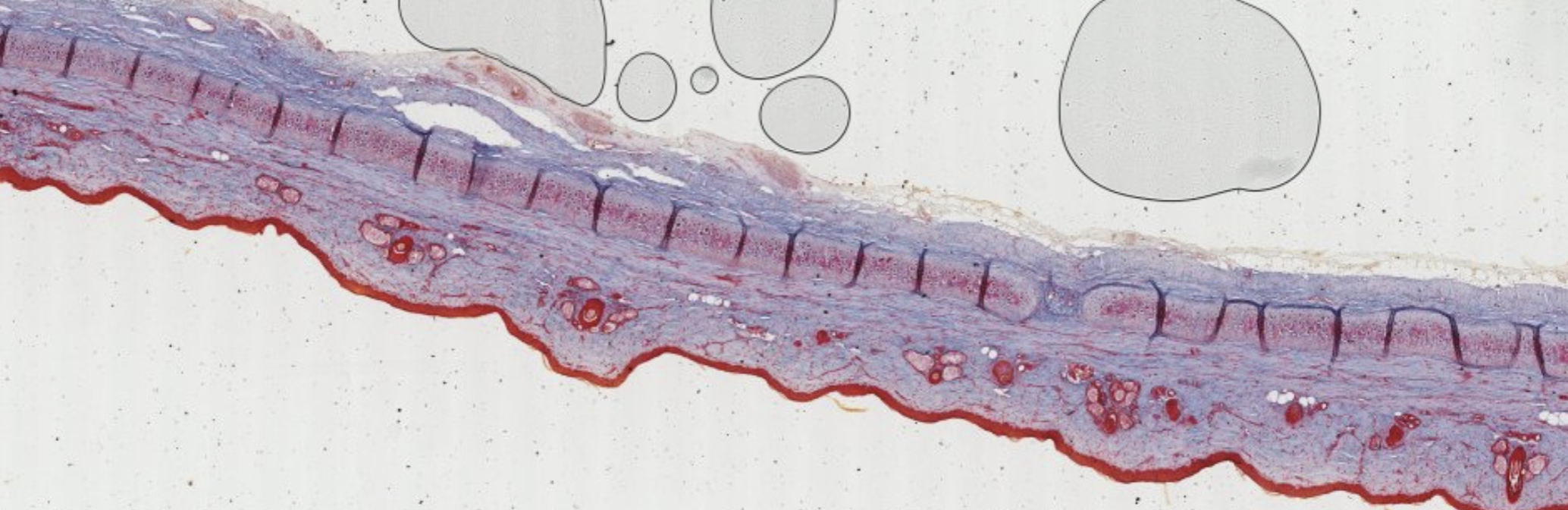
Classifying... https://unibo.smartzoom.com/s1241/course1776/f1841/i1845/
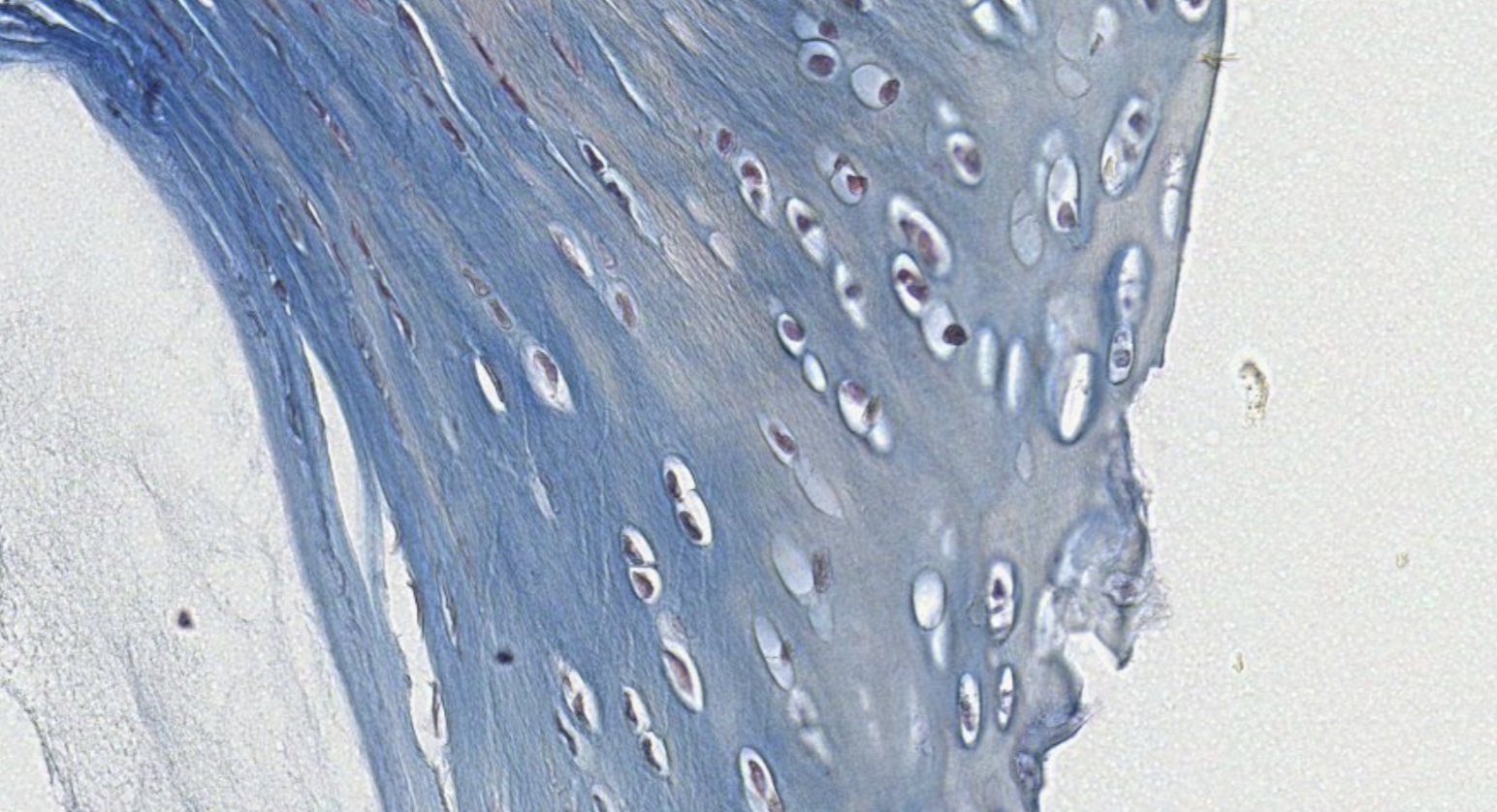
Here the chondrocytes are visible in this columnar organization, the collagen fibers here are collagen type I, this is very easy to classify…
What’s this? Here it’s a hyalin something that is becoming BONE!! WOW!
Summary of Cartilage Features
| Feature | Hyaline | Elastic | Fibrocartilage |
|---|---|---|---|
| Function | Resists compression; cushioning/low-friction joint surface; structural support in respiratory system; template for endochondral bone formation | Provides flexible support for soft tissues | Resists deformation under stress |
| Perichondrium | Yes (except articular cartilage and epiphyseal plates) | Yes | No |
| Calcifies? | Yes (endochondral bone formation, aging) | No | Yes (fibrocartilaginous callus during bone repair) |
| Main cell types | Chondroblasts and chondrocytes | Chondroblasts and chondrocytes | Chondrocytes and fibroblasts |
| ECM characteristics | Type II collagen fibrils, aggrecan monomers | Type II collagen fibrils, elastic fibers, aggrecan monomers | Types I and II collagen fibers; aggrecan (from chondrocytes) and versican (from fibroblasts) |
| Growth | Interstitially and appositionally; very limited in adults | Interstitially and appositionally; very limited in adults | Interstitially and appositionally; very limited in adults |
| Repair | Very limited capability; commonly forms scar → fibrocartilage | Very limited capability; commonly forms scar → fibrocartilage | Very limited capability; commonly forms scar → fibrocartilage |
Anki cloze
Fibrocartilage contains proteoglycan monomers {1:aggrecan} (secreted by chondrocytes) and {1:versican} (secreted by fibroblasts).
Which type of cartilage lacks a perichondrium?
Fibrocartilage lacks a perichondrium.
Additionally, articular hyaline cartilage and epiphyseal plates also lack perichondrium.
TLDR
Cartilage — Complete Summary
- Cartilage is avascular, aneural, alymphatic — nutrients reach cells by diffusion through ECM.
- Three cell types: chondrogenic cells (precursors) → chondroblasts (active secretors) → chondrocytes (mature, in lacunae, –).
- Three cartilage types: Hyaline (type II collagen, most abundant), Elastic (type II + elastic fibers, most pliable), Fibrocartilage (type I collagen, no perichondrium, greatest tensile strength).
- Hyaline cartilage: glassy appearance; found in nose, larynx, trachea, costal cartilage; forms fetal skeletal template; articular cartilage has no perichondrium and does not ossify.
- Perichondrium: two layers — outer fibrous (fibroblasts, collagen I, vessels) and inner chondrogenic (source of appositional growth).
- Matrix zones: pericellular capsule → territorial matrix (proteoglycan-rich, collagen-poor) → inter-territorial matrix (collagen-rich, proteoglycan-poor).
- Hyaline matrix: ~ type II collagen, proteoglycan aggregates (aggrecan), glycoproteins, ECF.
- Two growth mechanisms: interstitial (from within lacunae, early development) and appositional (from perichondrium, surface addition).
- Chondrogenesis sequence: MSCs → chondroprogenitors → chondroblasts → chondrocytes → hypertrophic chondrocytes; driven by TGF-β, BMPs, FGFs, IGF-1; Sox-9 is the key transcription factor.
- Step 1 of chondrogenesis: FGF/BMP-driven MSC condensation into a chondrogenic nodule.
- Isogenous groups: daughter cells from mitosis of chondroblasts remaining within the same lacuna (up to 4 cells); enclosed by territorial matrix.
- Elastic cartilage: same structure as hyaline + abundant elastic fibers; found in auricle, epiglottis, laryngeal cartilages.
- Fibrocartilage: type I collagen, low proteoglycan/water, no perichondrium, great tensile strength; intervertebral discs, pubic symphysis, tendon/ligament insertion sites; chondrocytes in short columns.
- Repair: very limited; perichondrium-derived repair cartilage contains both type I and II collagen (intermediate composition); commonly results in fibrocartilage scar.
- Calcification: hyaline (during ossification and aging) and fibrocartilage (during bone repair) calcify; elastic cartilage does not.